April 2024
Dr. Timothy Young discusses what to expect after Lapiplasty bunion surgery, focusing on post-op recovery.
Here are the key points:
- Day of Surgery:
- Arrival at the surgery center, where preparation and anesthesia discussions occur.
- The surgery typically lasts around 2 hours, involving incisions, bunion removal, and toe joint realignment.
- Recovery Timeline:
- Post-operative care in the recovery room with monitoring and pain management.
- Most patients go home on the same day.
- First Weeks After Surgery:
- Pain management with prescribed medication.
- Swelling and bruising are normal; ice packs and elevation help.
- Weight-bearing timeline varies, with gradual progression from non-weight bearing to partial weight bearing over weeks.
- First 2 weeks after the Lapiplasty, using a scooter or crutches and keeping weight off week 3-6 after surgery you start to progressively bear weight with your boot. For example, at the beginning of week 3 you will spend 15 minutes per hour allowing weight with the boot on your heel. The following week you'll spend 20 - 30 minutes per hour with the boot and with the final week 45 minutes per hour with the boot.
- Long-Term Recovery:
- Physical therapy may be recommended after 4-6 weeks to restore strength and flexibility.
- Driving can be as early as 6 weeks after surgery.
- Using the stationary bike and upper body workout can be done as early as week 5 - 6 after surgery.
- Gradual return to normal activities over several months. Bone healing and stability of the fusion site usually occurs after the initial 4 months. This is why it's necessary to wait for high-impact activities like jumping and running until 4 months.
- Full recovery can take six months to a year.
- Complications:
- Working closely with our patients, our goal is to avoid complications such as infection, poor wound healing, nerve damage, or bunion recurrence.
- Following post-operative care instructions is crucial to avoid these complications.
- Conclusion:
- Bunion surgery can be life-changing and literally change the structure of your foot.
- Patients should follow their surgeon's advice for a smoother recovery and embrace a more comfortable, active lifestyle with patience and proper care.
If you have any questions or would like a consultation please call 425-391-8666 and make an appointment online.
Dr. Timothy Young
Foot & Ankle Surgeon
Issaquah’s Top Podiatrist
Dr. Brandon Nelson, A Double Board-Certified Physician & Surgeon, Discusses Neuromas
Neuromas are an inflammatory disorder of the nerves in your foot. Typically, it is in the forefoot between the 3rd and 4th toe. It most commonly presents in the 3-5th decade of life and seems to be more common in women.
Causes:
The most common cause appears to be foot structure. We see patients that have a higher arched foot put a lot of pressure on their forefoot. This reparative pressure can inflame the nerves in the front of the foot causing a neuroma to form. Footwear choices can further exacerbate this, especially narrow shoes, or high heels. Other things like repetitive stress, running, jumping, anything that causes more forefoot pressure can cause neuroma pain.
Symptoms:
The symptoms can vary from patient to patient. However, some of the most common symptoms include burning, tingling and pain. Some patients relate that taking off their shoes reduces the pain and burning. Some relate rubbing helps the symptoms and some may feel a lump with rubbing of their foot.
Treatments:
We have many options available for treatment of neuromas. Some of the most common included orthotics, NSAIDS, and injections. I personally like to use dehydrated alcohol therapy it seems to have the highest success rate approaching 90%. Before treatment the most important thing is to get a correct diagnosis.
Neuromas can be very challenging and there are a few other problems that mimic neuroma symptoms. A careful diagnosis and treatment plan can be successful and not result in the need for surgical removal of the neuroma.
If you would like a consultation for your neuroma pain I can help. Call to make an appointment with me at 425-391-8666.
Sincerely,
Dr Brandon Nelson
American College of Foot & Ankle Surgeons
Issaquah’s Top Podiatrist
Investing in Custom Orthotics Means Investing in Foot Health
Custom orthotics offer a tailored approach to foot health, providing a host of benefits that extend far beyond conventional shoe inserts. One of the primary advantages lies in their ability to address specific biomechanical issues. Unlike off-the-shelf inserts, custom orthotics are crafted based on an individual's unique foot structure, gait, and any existing foot conditions.
The personalized design of custom orthotics ensures optimal support for the arches, promoting proper alignment and distributing pressure evenly across the feet. This can be particularly beneficial for individuals dealing with issues such as overpronation or underpronation, as custom orthotics help correct imbalances that may lead to discomfort or injury.
Beyond biomechanics, custom orthotics can alleviate a range of foot problems, including plantar fasciitis, bunions, and metatarsalgia. They provide targeted relief to areas under stress, reducing pain and inflammation. Additionally, for those with specific medical conditions like diabetes, custom orthotics can play a crucial role in preventing complications associated with poor foot health.
Comfort is another key aspect of custom orthotics. By accommodating the unique contours of an individual's feet, these inserts enhance overall comfort, making daily activities more enjoyable. Whether for athletes looking to optimize performance or individuals seeking relief from chronic foot pain, custom orthotics offer a versatile solution.
Investing in custom orthotics is an investment in long-term foot health. They not only provide immediate relief but also contribute to the prevention of future issues. With the ability to seamlessly integrate into various types of footwear, custom orthotics empower individuals to prioritize foot comfort without compromising on style. In essence, custom orthotics are a personalized prescription for happy, healthy, and pain-free feet.
Tailored Design of Foot Orthotics for Foot and Ankle Problems

Orthotic design plays a pivotal role in managing various foot problems, ranging from ankle issues to functional impairments and total contact needs. Ankle orthotics are specifically crafted to provide stability and support commonly used for conditions like ankle sprains or instability. Functional orthotics aim to correct biomechanical abnormalities, such as overpronation or supination, by realigning the foot and ankle joints during movement. These orthotics often incorporate features like arch support and heel cups to enhance stability and reduce strain. For individuals requiring total contact orthotics, the design focuses on evenly distributing pressure across the entire foot surface, important for conditions like diabetic foot ulcers. These orthotics are meticulously crafted to conform to the foot's contours, minimizing pressure points and promoting healing. If you are suffering from foot or ankle pain, it is suggested that you make an appointment with a podiatrist to discuss how customized orthotics can increase your comfort, support, and overall foot health.
Custom orthotics and shoe inserts are not just for cushioning the soles; they are about supporting the foundation of our body - our feet. The advantages extend far beyond immediate relief from discomfort. These personalized solutions, that Our doctors can prescribe, can significantly impact a person’s posture, alleviate pain in various parts of the body, and even enhance athletic performance.
As we lace up our shoes each day, having the right support can make a world of difference. Custom orthotics are like tailored suites for our feet, offering a bespoke solution to address our unique biomechanical needs. They provide stability where it is lacking, correct imbalances, and ensure that every step is a confident and pain-free one.
Custom orthotics and shoe inserts offer long-term health benefits. By addressing issues such as overpronation or underpronation, heel pain, plantar fasciitis, etc. orthotics can help prevent injuries and mitigate the progression of existing conditions. It’s an investment not just in the present, but in the future health of your feet and consequently, your overall well-being.
If you have any questions please contact one of our offices located in Issaquah, WA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
What are Achilles Tendon Injuries
The Achilles tendon is the strongest tendon in the human body. Its purpose is to connect the lower leg muscles and calf to the heel of the foot. This tendon is responsible for facilitating all types of movement, like walking and running. This tendon provides an enormous amount of mobility for the body. Any injuries inflicted to this tissue should be immediately brought up with a physician to prevent further damage.
The most common injuries that can trouble the Achilles tendon are tendon ruptures and Achilles tendinitis. Achilles tendinitis is the milder of the two injuries. It can be recognized by the following symptoms: inflammation, dull-to-severe pain, increased blood flow to the tendon, thickening of the tendon, and slower movement time. Tendinitis can be treated via several methods and is often diagnosed by an MRI.
An Achilles tendon rupture is trickier to heal, and is by far the most painful injury. It is caused by the tendon ripping or completely snapping. The results are immediate and absolutely devastating, and will render the patient immobile. If a rupture or tear occurs, operative and non-operative methods are available. Once the treatment begins, depending on the severity of the injury, recovery time for these types of issues can take up to a year.
Simple preventative measures can be taken as a means to avoid both injuries. Prior to any movement, taking a few minutes to stretch out the tendon is a great way to stimulate the tissue. Calf raises, squats, leg curls, leg extensions, leg raises, lunges, and leg presses are all suggested ways to help strengthen the lower legs and promote Achilles tendon health.
Many problems arise among athletes and people who overexert themselves while exercising. Problems can also happen among those who do not warm up properly before beginning an activity. Proper, comfortable shoes that fit correctly can also decrease tendon injuries. Some professionals also suggest that when exercising, you should make sure that the floor you are on is cushioned or has a mat. This will relieve pressure on the heels. A healthy diet will also increase tendon health.
It is very important to seek out a podiatrist if you believe you have an injury in the Achilles region. Further damage could result in severe complications that would make being mobile difficult, if not impossible.
Definition and Causes of an Achilles Tendon Rupture
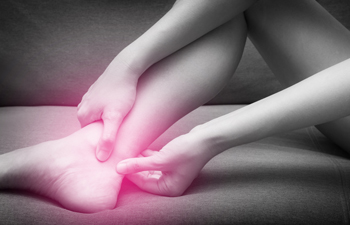
Achilles tendon rupture, a distressing injury affecting the tendon at the back of the ankle, can be debilitating and necessitate prompt attention. This critical tendon connects the calf muscles to the heel bone, facilitating movement like walking, running, and jumping. When subjected to excessive force or strain beyond its capacity, the Achilles tendon can tear partially or completely, resulting in a rupture. These types of injuries are frequently observed during activities involving sudden bursts of acceleration, abrupt changes in direction, or inadequate warm-up routines. Athletes, particularly those engaging in sports demanding rapid movements or high-impact activities, are at increased risk. Additionally, factors such as age weakened tendons due to degeneration, improper footwear, and inadequate conditioning contribute to susceptibility. Recognizing the signs and symptoms, including a sudden sharp pain in the heel, swelling, and difficulty walking or pointing toes downward, is vital for early diagnosis. If you have endured an Achilles tendon rupture, it is strongly suggested that you consult a podiatrist who can offer you effective treatment methods.
Achilles tendon injuries need immediate attention to avoid future complications. If you have any concerns, contact the podiatrists of Issaquah Foot & Ankle Specialists. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Is the Achilles Tendon?
The Achilles tendon is a tendon that connects the lower leg muscles and calf to the heel of the foot. It is the strongest tendon in the human body and is essential for making movement possible. Because this tendon is such an integral part of the body, any injuries to it can create immense difficulties and should immediately be presented to a doctor.
What Are the Symptoms of an Achilles Tendon Injury?
There are various types of injuries that can affect the Achilles tendon. The two most common injuries are Achilles tendinitis and ruptures of the tendon.
Achilles Tendinitis Symptoms
- Inflammation
- Dull to severe pain
- Increased blood flow to the tendon
- Thickening of the tendon
Rupture Symptoms
- Extreme pain and swelling in the foot
- Total immobility
Treatment and Prevention
Achilles tendon injuries are diagnosed by a thorough physical evaluation, which can include an MRI. Treatment involves rest, physical therapy, and in some cases, surgery. However, various preventative measures can be taken to avoid these injuries, such as:
- Thorough stretching of the tendon before and after exercise
- Strengthening exercises like calf raises, squats, leg curls, leg extensions, leg raises, lunges, and leg presses
If you have any questions please feel free to contact one of our offices located in Issaquah, WA . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Wounds That Don't Heal Need to Be Checked
What is Morton's Neuroma?
Morton’s neuroma, (also referred to as Morton’s metatarsalgia, Morton’s neuralgia, plantar neuroma or intermetatarsal neuroma) is a condition that is caused when the tissue around one of the nerves between your toes begins to thicken. This thickening can result in pain in the ball of the foot. Fortunately, the condition itself is not cancerous.
Morton’s neuroma affects women more often than men with a ratio of 4:1. It tends to target women between the age of 50 and 60, but it can occur in people of all ages. There are some risk factors that may put you at a slightly higher risk of developing the condition. People who often wear narrow or high-heeled shoes are often found to be linked to Morton’s neuroma. Additionally, activities such as running or jogging can put an enormous amount of pressure on the ligament and cause the nerve to thicken.
There usually aren’t any outward symptoms of this condition. A person who has Morton’s neuroma may feel as if they are standing on a pebble in their shoe. They may also feel a tingling or numbness in the toes as well as a burning pain in the ball of their foot that may radiate to their toes.
In order to properly diagnose you, the doctor will press on your foot to feel for a mass or tender spot. He may also do a series of tests such as x-rays, an ultrasound, or an MRI. X-rays are usually done to rule out any other causes for your foot pain such as a stress fracture. Ultrasounds are used to reveal soft tissue abnormalities that may exist, such as neuromas. Your podiatrist may want to use an MRI in order to visualize your soft tissues.
There are three main options for treatment of Morton’s neuroma: Injections, decompression surgery, and removal of the nerve. Injections of steroids into the painful area have been proven to help those with Morton’s neuroma. Decompression surgery has been shown to relieve pressure on the affected nerve by cutting nearby structures such as the ligaments in the foot. Another treatment option would be to surgically remove the growth to provide pain relief.
If you suspect that you have Morton’s neuroma you should make an appointment with your podiatrist right away. You shouldn’t ignore any foot pain that lasts longer than a few days, especially if the pain does not improve.
The Truth About Morton's Neuroma
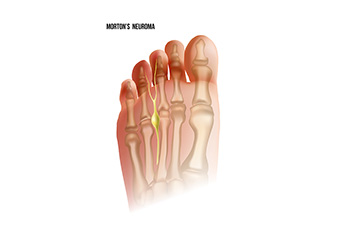
Morton's neuroma, a relatively common foot condition, occurs when a nerve between the toes becomes thickened and inflamed. Despite its name, it is not a true neuroma but rather a thickening of tissue surrounding one of the nerves that leads to the toes. This thickening can cause sharp, burning pain in the ball of the foot or between the toes, typically worsened by walking or wearing tight shoes. Although the exact cause remains unclear, factors such as wearing high heels or tight shoes, participating in high-impact activities, or having certain foot deformities may contribute to its development. Interestingly, Morton's neuroma tends to affect women more often than men. Diagnosis typically involves a physical examination and may include imaging tests such as X-rays or MRI scans to rule out other conditions. Early recognition and appropriate management are key to alleviating symptoms and preventing further complications. If you are experiencing pain in this part of your foot. It is suggested that you visit a podiatrist who can offer treatment options that are best for you.
Morton’s neuroma is a very uncomfortable condition to live with. If you think you have Morton’s neuroma, contact the podiatrists of Issaquah Foot & Ankle Specialists. Our doctors will attend to all of your foot care needs and answer any of your related questions.
Morton’s Neuroma
Morton's neuroma is a painful foot condition that commonly affects the areas between the second and third or third and fourth toe, although other areas of the foot are also susceptible. Morton’s neuroma is caused by an inflamed nerve in the foot that is being squeezed and aggravated by surrounding bones.
What Increases the Chances of Having Morton’s Neuroma?
- Ill-fitting high heels or shoes that add pressure to the toe or foot
- Jogging, running or any sport that involves constant impact to the foot
- Flat feet, bunions, and any other foot deformities
Morton’s neuroma is a very treatable condition. Orthotics and shoe inserts can often be used to alleviate the pain on the forefront of the feet. In more severe cases, corticosteroids can also be prescribed. In order to figure out the best treatment for your neuroma, it’s recommended to seek the care of a podiatrist who can diagnose your condition and provide different treatment options.
If you have any questions, please feel free to contact one of our offices located in Issaquah, WA . We offer the newest diagnostic and treatment technologies for all your foot care needs.



