September 2021
Dr Brandon Nelson, A Board-Certified Foot & Ankle Surgeon, Discusses the Most Common Causes of Heel Pain in Children
Heel pain can be common in children especially as they return to sports. We typically see girls between the ages of 8-12 and boys around 10-14. This increased incidence of heel pain at this time can be correlated with growth spurts or changes in activities. There is often a family history of heel pain as well from a parent or siblings. Unlike adults, very few children will have plantar fasciitis as the cause of heel pain. So, what are the main causes of heel pain in children? I will discuss a couple below.
Coalitions, these are where you have an abnormal connection between bones in the feet that should not be connected. Often, we see this type of pathology becoming painful after an injury, like an ankle sprain. Usually, an x-ray in needed to diagnosis this. This can differ based on location and there are two general locations of the coalitions. The two main locations are a calcaneal navicular and a talar calcaneal as the most common. The types of coalitions can vary, from bone to cartilage and even soft tissue.
Another common cause of heel pain in kids is Sever’s disease. This is basically an irritation of a growth plate that was first described by Dr Sever. This is especially common in cleated sports like soccer or football. There is usually a family history and common in flatfeet and kids with tight calf muscles. While this list is not exhaustive of all types of heel pain it is two of the most common, others can include a bone tumor, stress fracture or even a nerve irritation. Please make an appointment online or give us a call at 425-391-8666 if your child is having heel pain so we can help.
Dr Brandon Nelson, A Board-Certified Foot & Ankle Surgeon, Discusses the Most Common Bunionectomy
Bunion surgery is by far the most common foot surgery in the United States. The number of bunion surgeries performed per year in the U.S. is about 150,000. The majority of these bunion surgeries are done in an outpatient setting and take less than 1.5 hours.
What is a bunion?
Please watch the following video for more information on a bunion;
https://www.bestfootdoc.com/patient-education-videos
So, what is the most common bunionectomy to date? The answer is a distal osteotomy or cutting of the bone towards the head of the metatarsal. This procedure is called an Austin bunionectomy.
Please watch the following video to learn more about bunion procedures; https://www.youtube.com/watch?v=U_D0NhTZOyY
Bunion surgery does not need to be scary or overwhelming we are here to help.
Give us a call today at 425-391-8666 or make an appointment online.
Why Are My Toenails Thick?
Thickened toenails are typically a sign of a fungal toenail infection, which can cause changes in the texture and color of the toenail. An infected toenail can often thicken, become brittle or crumbly, and develop white, yellow, or brown discoloration. But while fungal infections are the most common cause of thickened toenails, they are not the only cause. Psoriasis, a skin condition, can also affect the toenails, making them thicker, pitted, and discolored. Paronychia, a nail disease caused by a bacterial infection, can thicken the toenail, make it discolored, and cause redness, pain, and inflammation around the nail. Diabetes can cause toenails to thicken because not enough nutrients are reaching the toenails to maintain their health. Other reasons your toenails may be thickened include onychogryphosis (Ram’s Horn), aging, a toenail injury, or a rare condition called yellow nail syndrome. If you notice changes in the thickness, color, or shape of your toenails, it is suggested that you schedule an appointment with a podiatrist.
If left untreated, toenail fungus may spread to other toenails, skin, or even fingernails. If you suspect you have toenail fungus it is important to seek treatment right away. For more information about treatment, contact the podiatrists of Issaquah Foot & Ankle Specialists. Our doctors can provide the care you need to keep you pain-free and on your feet.
Symptoms
- Warped or oddly shaped nails
- Yellowish nails
- Loose/separated nail
- Buildup of bits and pieces of nail fragments under the nail
- Brittle, broken, thickened nail
Treatment
If self-care strategies and over-the-counter medications does not help your fungus, your podiatrist may give you a prescription drug instead. Even if you find relief from your toenail fungus symptoms, you may experience a repeat infection in the future.
Prevention
In order to prevent getting toenail fungus in the future, you should always make sure to wash your feet with soap and water. After washing, it is important to dry your feet thoroughly especially in between the toes. When trimming your toenails, be sure to trim straight across instead of in a rounded shape. It is crucial not to cover up discolored nails with nail polish because that will prevent your nail from being able to “breathe”.
In some cases, surgical procedure may be needed to remove the toenail fungus. Consult with your podiatrist about the best treatment options for your case of toenail fungus.
If you have any questions, please feel free to contact one of our offices located in Issaquah, WA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Treating Toenail Fungus
Fungal infection of the toenail, or onychomycosis, typically appears as a gradual change in a toenail’s texture and color that involves brittleness and darkening. The fungal infection itself occurs beneath the surface of the nail. Aside from discoloration, other symptoms include the collection of debris beneath the nail plate, white marks on the nail plate, and a foul odor emanating from the nail. If ignored, the infection can spread into other nails and the skin; in severe cases, it can hinder one’s ability to work or walk.
The toenails are particularly vulnerable to contracting infection in moist environments where people are likely to be walking barefoot, such as around swimming pools, public showers, and locker rooms. Fungal infection may also be more likely to occur in nail beds that have been injured, and sufferers of chronic diseases such as diabetes, circulatory problems, or immunodeficiency conditions are particularly prone to developing fungal nails.
Fungal nails can be primarily prevented by practicing proper hygiene and regularly examining the feet and toes. Carefully washing the feet with soap and water and thoroughly drying the feet afterwards are essential. Other tips include wearing shower shoes in public areas, changing shoes and socks daily, keeping toenails clipped at a short length, wearing breathable shoes that fit properly, wearing moisture-wicking socks, and disinfecting home pedicure tools and instruments used to cut nails.
Fungal nail treatment may vary between patients and the severity of the condition. Your podiatrist may suggest a daily routine of cleansing that spans over a period of time to ease mild infections. Over-the-counter or prescription antifungal agents may also be prescribed, including topical and/or oral medications. Debridement, or the removal of diseased nail matter and debris, may also be performed. In more severe cases, surgical treatment may be needed. In some instances, the temporary removal of the fungal nail allows for the direct application of a topical antifungal to the nail bed. In other cases, a chronically painful fungal nail that has not responded to other treatments may be permanently removed; this allows the infection to be cured and avoids the growth of a deformed nail.
Dr. Brandon Nelson, A Board Certified Foot & Ankle Surgeon, Discusses Numbness and Tingling In Your Toes
Numbness and tingling can be quite common in people experiencing forefoot discomfort. Most people will describe symptoms like burning, pinching, numbness and tingling. These are often associated with nerve type issues and can continue to get worse without treatment. The most common causes of this in the foot are neuromas and capsulitis.
Neuromas are a nerve irritation that occurs in the foot and usually is a female between the ages of 40-60. The nerves that run between the toes are sensitive and any increases pressure can cause pain. This pain is usually made worse with tight fitting shoes or high heels. Patients usually have pain to the 3rd and 4th digit and often is only on one foot. Most people will say that rubbing the front of their foot seems to help as well as removing their shoes.
Capsulitis is usually around the base of the 2nd toe. There is often an underlying deformity like a bunion or tight calf muscle. Patients will often experience swelling and tingling or digit. It is usually made worse with walking and relieved with icing.
Neuromas and capsulitis both can be challenging for the patient and the doctor. It is important to identify the root cause and an x-ray is warranted. The treatment options available are usually very successful. If you are having forefoot pain we can help, make an appointment today.
Give us a call at 425-391-8666 or make an appointment online today.
What Is This Rash on My Feet?
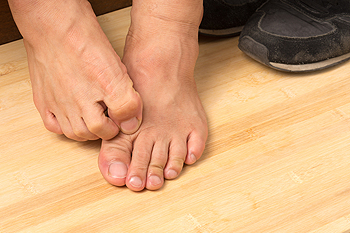 A rash on the feet can be indicative of a variety of medical conditions. One of the most common reasons for a foot rash is a fungal infection called athlete’s foot. The rash characteristic of athlete’s foot is usually scaly, flakey, itchy, and red, and it may also sting or burn. Irritant contact dermatitis is an allergic skin reaction that can affect the feet. A contact dermatitis rash features dry, cracked, scaly - but not itchy - skin in a localized area. Allergic contact dermatitis is caused by a more severe allergic reaction and often presents as small, pink or red skin bumps, spots, or blisters that are very itchy. Other conditions that can lead to a foot rash include hand foot and mouth disease, eczema, psoriasis, scabies, an insect bite, and medical conditions like chicken pox, shingles, and Lyme disease. If you have a rash on your feet, please consult with a podiatrist.
A rash on the feet can be indicative of a variety of medical conditions. One of the most common reasons for a foot rash is a fungal infection called athlete’s foot. The rash characteristic of athlete’s foot is usually scaly, flakey, itchy, and red, and it may also sting or burn. Irritant contact dermatitis is an allergic skin reaction that can affect the feet. A contact dermatitis rash features dry, cracked, scaly - but not itchy - skin in a localized area. Allergic contact dermatitis is caused by a more severe allergic reaction and often presents as small, pink or red skin bumps, spots, or blisters that are very itchy. Other conditions that can lead to a foot rash include hand foot and mouth disease, eczema, psoriasis, scabies, an insect bite, and medical conditions like chicken pox, shingles, and Lyme disease. If you have a rash on your feet, please consult with a podiatrist.
Athlete’s foot is an inconvenient condition that can be easily reduced with the proper treatment. If you have any concerns about your feet and ankles, contact the podiatrists from Issaquah Foot & Ankle Specialists. Our doctors will treat your foot and ankle needs.
Athlete’s Foot: The Sole Story
Athlete's foot, also known as tinea pedis, can be an extremely contagious foot infection. It is commonly contracted in public changing areas and bathrooms, dormitory style living quarters, around locker rooms and public swimming pools, or anywhere your feet often come into contact with other people.
Solutions to Combat Athlete’s Foot
- Hydrate your feet by using lotion
- Exfoliate
- Buff off nails
- Use of anti-fungal products
- Examine your feet and visit your doctor if any suspicious blisters or cuts develop
Athlete’s foot can cause many irritating symptoms such as dry and flaking skin, itching, and redness. Some more severe symptoms can include bleeding and cracked skin, intense itching and burning, and even pain when walking. In the worst cases, Athlete’s foot can cause blistering as well. Speak to your podiatrist for a better understanding of the different causes of Athlete’s foot, as well as help in determining which treatment options are best for you.
If you have any questions please feel free to contact one of our offices located in Issaquah, WA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Athlete's Foot
Athlete’s foot is an extremely contagious infection caused by a fungus that results in itching, burning, dry, and flaking feet. The fungus that causes athlete’s foot is known as tinea pedis and thrives in moist, dark areas such as shower floors, gyms, socks and shoes, commons areas, public changing areas, bathrooms, dormitory style houses, locker rooms, and public swimming pools. Athlete’s foot is difficult to treat as well because of the highly contagious and recurrent nature of the fungus.
Tinea is the same fungus that causes ringworm, and is spread by direct contact with an infected body part, contaminated clothing, or by touching other objects and body parts that have been exposed to the fungus. Because the feet are an ideal place for tinea to grow and spread, this is the most commonly affected area. It is, however, known to grow in other places. The term athlete’s foot describes tinea that grows strictly on the feet.
The most commonly infected body parts are the hands, groin, and scalp, as well as the feet. Around 70% of the population suffer from tinea infections at some point in their lives, however not all of these cases are athlete’s foot. Just like any other ailment, some people are more likely to get it than others, such as people with a history of tinea infections or other skin infections, both recurring and non-recurring ones. The extent to which a person experiences regrowth and recurrent tinea infections varies from person to person.
Sometimes people will not even know that they are infected with tinea or that they have athlete’s foot because of a lack of symptoms. However, most experience mild to moderate flaking, itching, redness, and burning. However, some of the more severe symptoms include cracking and bleeding skin, intense itching and burning, pain while walking or standing, and even blistering.
Because of the recurring nature of the tinea fungus and the athlete’s foot it causes, the best way to treat this condition is with prevention. You can take some preventative measures such as wearing flip flops or sandals in locker rooms and public showers to reduce contact with the floor. It also helps to keep clean, dry feet while allowing them to breathe. Using powders to keep your feet dry is a good idea, as well as keeping your feet exposed to light and cool air, to prevent the growth of tinea. If you do happen to get athlete’s foot, opt for using topical medicated creams, ointments or sprays. These treatments help eliminate and prevent it from coming back.
Dr Brandon Nelson, A Board Certified Physician and Surgeon, Discusses Minimally Invasive Achilles Tendon Surgery
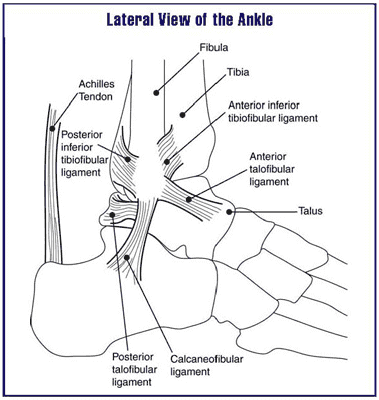
Achilles tendonitis or bone spurs in the Achilles tendon are common pathologies we see as foot and ankle surgeons. These two conditions are often started with over training or long-standing tight calf muscles. Both can lead to rupturing or a painful Achilles tendon with any sort of activity. It can be quite challenging to rest this area or rehab this tendon as it never really is inactive when ambulating.
Many patients will end up requiring surgical repair of their Achilles and new modern approaches can minimize down time. Previously all patients had required at least 6 weeks of non-weight bearing. However new techniques have improved outcomes and eliminated the need for non-weight bearings.
Achilles tendonitis usually presents around the mid substance of the Achilles. It is usually a painful bump that can swell with exercise. In the past patients requiring repair required a standard incisional approach with a long recovery. However, I have been utilizing the Tenex procedure which has almost no downtime and can be preformed without anesthesia if patients prefer. The Tenex stimulates new growth and repair of old tendon pathology. After the procedure patients can walk and return to activities shortly.
Bones spurs in the Achilles tendon have previously requires an extensive surgery to remove the bone and repair the tendon. I have been using Tenex on these cases as well and patients can walk immediately after the procedure and require no re-attaching of the Achilles tendon. If you are looking for a quick recovery, minimal down time or minimally invasive Achilles tendon surgery I can help. Give us a call today at 425-391-8666 or make an appointment online today.
Bunion Surgery Recovery, Dr Brandon Nelson

Quite a few patients ask about bunion surgery and bunion surgery recovery. I hear a lot of stories from patients about neighbors, friends or family members that have had bunion surgery. There seems to be some misconceptions about bunion surgery and some general misconceptions. I want to help clarify this for patients and anybody thinking about fixing their bunion.
Bunion surgery can really be broken down into two different procedure locations. Bunions can be corrected at the head of the metatarsal or the base of the metatarsal. The head procedures are generally utilized for smaller bunions and base procedures are better suited for larger bunions.
Head procedures are probably the most common bunion procedure. This is often called an Austin bunionectomy and has been around for greater than 50 years. It was one of the first bunion procedures and has great success and most patients can return to a normal shoe in about 4-6 weeks. Patients can walk the entire time after surgery in a boot for about 4 weeks.
Base procedures are a little more involved surgery and therefore the recovery is longer. Most base procedures can allow patients to walk in a boot in 2-4 weeks. However, the total recovery from this type of surgery can be 8 weeks or longer.
I hope this helps to answer a few bunion surgery questions! Give us a call at 425-391-8666 or make an appointment online today.
What Is Haglund’s Deformity?
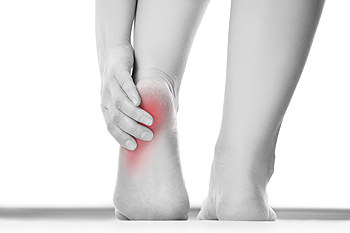 Haglund’s deformity is an enlargement of a portion of the bone on the back of the heel. The enlarged part of the bone can irritate surrounding soft tissues causing heel pain, swelling, redness, and the formation of a visible hard lump on the back of the heel. Haglund’s deformity is thought to be hereditary. Some people are genetically predisposed to this condition due to the inherited structure of their feet. Other potential causes may include calf muscle tightness, having a dysfunctional walking pattern, or wearing ill-fitting shoes. If you notice a painful bump on the back of your heel, it is suggested that you schedule an appointment with a podiatrist who can find the right treatment for you.
Haglund’s deformity is an enlargement of a portion of the bone on the back of the heel. The enlarged part of the bone can irritate surrounding soft tissues causing heel pain, swelling, redness, and the formation of a visible hard lump on the back of the heel. Haglund’s deformity is thought to be hereditary. Some people are genetically predisposed to this condition due to the inherited structure of their feet. Other potential causes may include calf muscle tightness, having a dysfunctional walking pattern, or wearing ill-fitting shoes. If you notice a painful bump on the back of your heel, it is suggested that you schedule an appointment with a podiatrist who can find the right treatment for you.
Many people suffer from bouts of heel pain. For more information, contact the podiatrists of Issaquah Foot & Ankle Specialists. Our doctors can provide the care you need to keep you pain-free and on your feet.
Causes of Heel Pain
Heel pain is often associated with plantar fasciitis. The plantar fascia is a band of tissues that extends along the bottom of the foot. A rip or tear in this ligament can cause inflammation of the tissue.
Achilles tendonitis is another cause of heel pain. Inflammation of the Achilles tendon will cause pain from fractures and muscle tearing. Lack of flexibility is also another symptom.
Heel spurs are another cause of pain. When the tissues of the plantar fascia undergo a great deal of stress, it can lead to ligament separation from the heel bone, causing heel spurs.
Why Might Heel Pain Occur?
- Wearing ill-fitting shoes
- Wearing non-supportive shoes
- Weight change
- Excessive running
Treatments
Heel pain should be treated as soon as possible for immediate results. Keeping your feet in a stress-free environment will help. If you suffer from Achilles tendonitis or plantar fasciitis, applying ice will reduce the swelling. Stretching before an exercise like running will help the muscles. Using all these tips will help make heel pain a condition of the past.
If you have any questions please contact one of our offices located in Issaquah, WA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.