February 2022
Dr. Brandon Nelson, Board-Certified Foot and Ankle Surgeon discusses Minimally Invasive Bunion Surgery
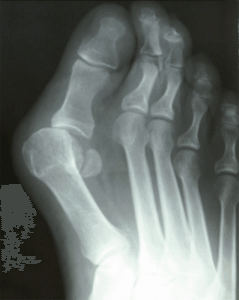
A bunion is a common forefoot condition that can be characterized by mild, moderate or severe and defined as a deviation of the big toe in the lateral direction. This condition is progressive and can lead to pain and discomfort with walking and exercise. Conservative measures are not usually successful. The traditional approach consists of an open incision and dissection of the foot that involves balancing of soft tissues and bony deformities. The procedure itself is highly successful but there is question as to whether more minimally invasive type accessible.
Minimally invasive bunion surgery has been around for years and as this technique is getting better, this becomes more of a promising type procedure. The literature is full of different types of minimally invasive bunion surgeries that can be used correct the foot. Some of the most promising new or techniques utilize screw or pin fixation and has become highly successful.
All done under direct live x-ray and results have been extremely positive. Majority of patients are weightbearing immediately after surgery and can return to normal shoes in 3-4 weeks. This is because of the soft tissues had minimal interruption and vascularity preserved. Minimally invasive bunion surgery shows promising results and can provide a fast return to activities.
If you’re suffering from bunion deformity and would like to discuss minimally invasive bunion procedure, call 425- 391-8666 or make an appointment online today.
Sincerely,
Dr. Brandon Nelson
Board-certified Foot and Ankle Physician and Surgeon
Complications With Diabetes and the Feet
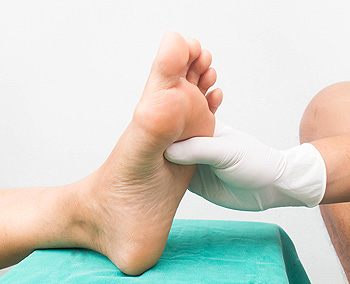 Diabetes is a systemic condition that can affect many parts of your body – including the feet. Due to the chronically raised blood sugar levels associated with diabetes, the nerves and blood vessels that supply the lower limbs can become damaged. This can cause neuropathy and poor circulation, both of which can lead to strange sensations, such as burning and tingling or numbness in the feet, a loss of sensation, and the formation of poorly healing foot wounds. The skin and nails on the feet may also change. Skin can become dry and cracked, and start to peel, and calluses may form more quickly, as well. Because diabetes can also cause immune insufficiency, foot and nail infections are more likely to occur. If you have diabetes, it is suggested that you visit a podiatrist regularly to monitor and preserve the health of your feet.
Diabetes is a systemic condition that can affect many parts of your body – including the feet. Due to the chronically raised blood sugar levels associated with diabetes, the nerves and blood vessels that supply the lower limbs can become damaged. This can cause neuropathy and poor circulation, both of which can lead to strange sensations, such as burning and tingling or numbness in the feet, a loss of sensation, and the formation of poorly healing foot wounds. The skin and nails on the feet may also change. Skin can become dry and cracked, and start to peel, and calluses may form more quickly, as well. Because diabetes can also cause immune insufficiency, foot and nail infections are more likely to occur. If you have diabetes, it is suggested that you visit a podiatrist regularly to monitor and preserve the health of your feet.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact the podiatrists from Issaquah Foot & Ankle Specialists. Our doctors can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
- Routinely inspect your feet for bruises or sores.
- Wear socks that fit your feet comfortably.
- Wear comfortable shoes that provide adequate support.
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions please feel free to contact one of our offices located in Issaquah, WA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Diabetic Foot Conditions
According to the American Diabetes Association (ADA), diabetes is a condition that affects approximately 23.6 million Americans. Around 750,000 new cases are diagnosed each year, and the disease’s most common form, Type 2 diabetes, makes up for 90 to 95 percent of these cases. Type 2 diabetes is especially prevalent among older Americans, those who are obese, and those who lead sedentary lifestyles.
Complications of the disease may lead to several foot and ankle-related conditions. The loss of nerve sensation, or neuropathy, can cause diabetics to lose feeling at the bottom of the feet and therefore leave them unaware of pain, pressure, and heat. Decreased circulation is another complication of diabetes that can slow down the healing of wounds and injuries; this can lead to the development of foot ulcers.
To prevent foot ulcers from forming, diabetics should examine their feet every day for small cuts and wear shoes that curtail pressure. Constant monitoring for the risk factors associated with ulcer formation can allow for early detection and therefore lessen the possibility of ulcers or, even worse, amputation. The removal of calluses and ingrown toenails should be left to the podiatrist to avoid improper removal and possible infection.
Diabetic patients may also experience foot deformities due to complications in their feet, such as limited joint mobility, muscle atrophy, and decreased fat padding. These complications can increase pressure in certain areas of the foot, which in turn can cause certain deformities, such as hammertoe, to form. Another deformity, Charcot foot, develops due to the collapsing of microfractures in the bones of the feet. The resulting deformity is a foot that is flattened and wider in appearance.
To help minimize pressure and prevent the development of these diabetes-related foot and ankle conditions, your podiatrist may consider using orthotics or special shoes. Charcot foot may be treated using walkers, custom orthotic insoles, or non-weight-bearing or rigid weight-bearing casts or braces. In more serious cases, surgery may be considered to treat more developed deformities. Ulcers can be further cared for with the help of proper diet, medication to control glucose, intensive wound care, and infection treatment.
Dr. Brandon Nelson, Board-Certified Foot and Ankle Physician, Talks About Ingrown Nails
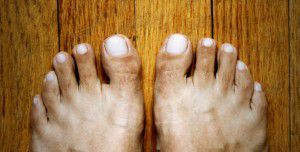
Ingrown nails can be extremely uncomfortable. They are caused from a bacterial infection typically in the big toe. Often times patients will have a history of ingrown toenails or family history of ingrown toenails. It is important to not try and treat ingrown toenails at home as this typically will make the infection worse. Ingrown nails themselves typically present as pain and swelling along the border of the toenail where the skin, patients will experience some drainage from the site and is often painful at times.
I recommend patients are evaluated when their nails are sore, red, thickened or painful with walking. There are many different options for treating an ingrown nail however typically the offending nail border has to be removed. Once removal is performed the procedure of choice is really dictated by the number of ingrown toenails the patient has experienced. The two options are an incision and drainage or what is called a matrixectomy.
Option one or incision and drainage involves removal of the offending nail border. This is typically done on just the side that is painful. Prior to removal the toe is anesthetized, cleaned and sterile prep. Nail is then removed with the hemostat appendicitis, flushed and covered with a sterile compressive dressing. Typical recovery from something like this is patients can return to activities the next day or so once a day for 1 week.
A matrixectomy involves a similar technique as described above. However once the nail is removed the nail cells are cauterized to prevent them from growing back. Matrixectomy is a procedure specifically designed for someone that has a history of recurrent ingrown toenails or long family history of ingrown nails. The patient’s toe will be red and sore often times for 2-3 weeks after the procedure.
If you’re experiencing painful swollen digit please give me a call today and I can help 425-391-8666, or make an appointment online.
Sincerely,
Board-Certified Foot and Ankle Physician and Surgeon
Dr. Brandon Nelson, Board-Certified Foot and Ankle Physician and Surgeon, Discusses Outcomes for Bunion Surgery
Bunion surgery continues to be the most common foot and ankle surgery performed and there are many different procedures available. Not all of the procedures have equal outcomes. The most common bunionectomy performed in the United States continues to be what is called an Austin bunionectomy or a head procedure. This type of procedure is primarily used to correct mild to moderate bunions. This procedure has great outcomes, as patients do well ambulatorily postoperatively. Most patients will be back to activities fairly quickly and long-term results are good as long as there are no other foot deformities. This type of bunion procedure is fairly straightforward and can be performed in 30-45 minutes. Postoperative protocol is easy and pain level is generally mildly and well controlled with oral medications.
The second most common type of bunionectomies are for severe bunions or people with foot instability. These procedures usually involve more in depth bunionectomy or stability type procedures. The most common bunionectomy for this is what is called a Lapidus bunionectomy. This procedure involves fusion of bones on the inside of the foot and provides great correction and increased stability for the foot itself. This procedure can often involve a period of nonweightbearing or modified weightbearing and usually takes longer to heal from within the previously discusses bunion. However it should be noted the recurrence rate with this type of bunionectomy is much less and the long-term outcomes are are great. Again, it is important to address other foot structure issues as these can have effect on long-term results.
If you’re suffering from a bunion or foot pain, an evaluation is essential. Call the office at 425-391-8666 or make an appointment online today so I can help.
Sincerely,
Board-Certified Foot and Ankle Physician and Surgeon
What Is Medial Tibial Stress Syndrome?
Medial tibial stress syndrome (MTSS), more commonly known as shin splints, is an injury to the shin bone that occurs due to excess pressure being placed on it during physical activity. Shin splints are characterized by pain, tenderness, or soreness on the inside of the lower leg bone, particularly during exercise. Shin splints are typically treated through conservative methods. You may be encouraged to rest the injured leg, taking pressure off of it and giving it time to heal. Applying ice to the affected leg and taking over-the-counter medications can help reduce pain. Doing strengthening and stretching exercises may also help. To prevent shin splints, you should make sure that your shoes fit well and are supportive. When exercising, increase the length and intensity of your workouts slowly over time to avoid placing too much stress on the shin bones. For more information about shin splints, please consult with a podiatrist.
Ankle and foot injuries are common among athletes and in many sports. They can be caused by several problems and may be potentially serious. If you are feeling pain or think you were injured in a sporting event or when exercising, consult with the podiatrists from Issaquah Foot & Ankle Specialists. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
Common Injuries
The most common injuries that occur in sporting activities include:
- Achilles Tendonitis
- Achilles Tendon Rupture
- Ankle Sprains
- Broken Foot
- Plantar Fasciitis
- Stress Fractures
- Turf Toe
Symptoms
Symptoms vary depending upon the injury and in some cases, there may be no symptoms at all. However, in most cases, some form of symptom is experienced. Pain, aching, burning, bruising, tenderness, tightness or stiffness, sensation loss, difficulty moving, and swelling are the most common symptoms.
Treatment
Just as symptoms vary depending upon the injury, so do treatment options. A common treatment method is known as the RICE method. This method involves rest, applying ice, compression and elevating the afflicted foot or ankle. If the injury appears to be more serious, surgery might be required, such as arthroscopic or reconstructive surgery. Lastly, rehabilitation or therapy might be needed to gain full functionality in the afflicted area. Any discomfort experienced by an athlete must be evaluated by a licensed, reputable medical professional.
If you have any questions please contact one of our offices located in Issaquah, WA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Sports Related Foot and Ankle Injuries
Foot and ankle injuries are common among athletes and those who exercise frequently. Most of these injuries are non-life-threatening and can heal in weeks with proper treatment and care. Serious injuries, however, require urgent medical treatment.
Common minor injuries include ankle sprains, ankle strains, Achilles tendonitis, plantar fasciitis, stress fractures, and turf toe. An ankle sprain is when the ligaments in the ankle have either become stretched or torn. When the muscle or tendon is stretched or torn, it is an ankle strain. When the big toe is sprained, it is known as turf toe. Achilles tendonitis is the overuse and inflammation of the Achilles tendon. Plantar fasciitis is the inflammation of the plantar fascia and generally occurs from overuse in athletics. Stress fractures are also caused from overuse and are small cracks in the bone.
Achilles tendon ruptures are common, but more serious. This injury occurs when the Achilles tendon, the largest tendon in the body, ruptures. In most cases, this causes severe pain and difficulty walking; some who have experienced this injury have reported, however, no signs or symptoms. A laceration is a deep cut that can occur anywhere on the body. Lacerations on the foot are rarer, but can occur from things like metal cleats landing on the foot.
Treatment options cover a wide range of methods based upon the injury and its severity. Conditions like plantar fasciitis, stress fractures, Achilles tendonitis, turf toe and ankle sprains/ strains can heal on their own without immediate medical care, but seeing a podiatrist to monitor the injury is always recommended. Following the RICE (Rest, Icing, Compression, and Elevation) protocol is generally enough to treat minor injuries. This means resting the foot by either keeping pressure off the foot or not walking at all. Icing the injury will help reduce swelling and pain. Compressing the wound with a wrap will immobilize and help promote healing. Finally, keeping the wound elevated will also reduce swelling and also help the healing process.
It is important to note that even minor injuries can vary in severity, with grade one being a minor injury and grade three requiring urgent care by a podiatrist. Achilles tendon ruptures and lacerations on the foot generally require urgent medical care and treatment options that need a podiatrist. These could include imaging tests, stitches for cuts, rehabilitation, and casts or braces. Every case is different, however, so it is always recommended to see a podiatrist when pain in the foot does not disappear.



