July 2021
Dr Brandon Nelson, A Board Certified Surgeon, Discusses How To Get Rid Of That Morning Foot Pain

It is common for patients to come in the office and relate pain in the morning or right when they get out of bed. This can be a challenging way to start your day and can lead to chronic foot pain. Most patients describe the pain as a bruised feeling to the heel or a tightness with pins and needles. This can go on for months and become chronic. The most common cause of this type of pain is Plantar Fasciitis. Plantar Fasciitis is an inflammation of a supporting band of tissue on the bottom of the foot. The Plantar Fascia is essential for normal foot function and when it is inflamed daily tasks can be overwhelming.
Morning pain is one of the most common signs of Plantar Fasciitis. The reason behind this is while you sleep your Fascia and Achilles Tendon have a chance to relax. With this relaxation both structures begin to tighten up. This tightening up leads to stiffness when you first step on your foot. One can really help this by exercising their foot before getting out of bed. I recommend writing the alphabet with your foot and stretching with a theraband.
If your pain continues for more than a week an appointment is essential. Give us a call at 425-391-8666 or make an appointment online today.
Getting to the Cause of Your Ankle Pain
As one of the body’s most critical weight-bearing structures, your ankles can experience pain from a variety of causes: sprains, ankle instability due to repeated sprains or structural problems, tarsal tunnel syndrome (compression of nerves), tendonitis, fractures, or diseases that can affect the feet such as arthritis, diabetes, or gout. Ankle discomfort may be experienced as an aching pain that worsens when you move your ankle or put weight on your feet, stiffness, inflammation, warmth, or redness in the area. A podiatrist can examine and test you, and devise a treatment plan to not only relieve your ankle pain but also to help avoid chronic ankle instability from setting in.
Ankle sprains are common but need immediate attention. If you need your feet checked, contact the podiatrists from Issaquah Foot & Ankle Specialists. Our doctors can provide the care you need to keep you pain-free and on your feet.
How Does an Ankle Sprain Occur?
Ankle sprains take place when the ligaments in your ankle are torn or stretched beyond their limits. There are multiple ways that the ankle can become injured, including twisting or rolling over onto your ankle, putting undue stress on it, or causing trauma to the ankle itself.
What Are the Symptoms?
- Mild to moderate bruising
- Limited mobility
- Swelling
- Discoloration of the skin (depending on severity)
Preventing a Sprain
- Wearing appropriate shoes for the occasion
- Stretching before exercises and sports
- Knowing your limits
Treatment of a Sprain
Treatment of a sprain depends on the severity. Many times, people are told to rest and remain off their feet completely, while others are given an air cast. If the sprain is very severe, surgery may be required.
If you have suffered an ankle sprain previously, you may want to consider additional support such as a brace and regular exercises to strengthen the ankle.
If you have any questions please feel free to contact one of our offices located in Issaquah, WA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Ankle Sprains
Ankle sprains occur when ligaments that support the ankle stretch beyond their limits and tear. These types of injuries are very common and can occur in people of all ages. Sprains may range from mild to severe, depending on how much damage is done to the ligaments. If a sprain goes untreated, a more severe sprain may occur which can further damage the ankle. Repeated ankle sprains can lead to chronic ankle pain.
There are some risk factors that can increase your risk of suffering a sprained ankle. Those who participate in sports, walk on uneven surfaces, have a prior ankle injury, are in poor physical condition, or wear improper shoes are more likely to get a sprained ankle.
There are a few symptoms to look out for if you suspect you are suffering from a sprained ankle. Some common symptoms are swelling, bruising, tenderness, and instability of the ankle. In cases where the tearing of the ligaments is severe, there may be a “popping” sound when the strain occurs.
The RICE method is proven to be effective in treating ankle sprains. RICE stands for Rest, Ice, Compression, and Elevation. Rest is important for treatment, especially within the first 24 to 48 hours. You should also ice your sprained ankle for the first 48 hours for 20 minutes at a time. A small piece of cloth should be placed between the ice and the affected area. For the compression step, you should wear a brace that is snug, but not too tight that it cuts off circulation. When choosing a brace, be sure to choose one that is suitable for the type of ankle sprain you have. Lastly, you should elevate your foot above the heart as often as possible.
After you treat a sprain, you should go through rehabilitation to prevent the injury from occurring again. There are three phases to the rehab process. The first phase involves resting, protecting, and reducing the swelling of the injury. The second phase consists of restoring the ankle’s flexibility, range of motion, and strength. The third phase consists of slowly returning to activity and maintenance exercises.
If you suspect you have an ankle sprain, you shouldn’t hesitate to consult with your podiatrist. Your podiatrist will be able to give you a proper diagnosis and a suitable treatment option for your condition.
Dr. Brandon Nelson, A Board-Certified Surgeon, Discusses the Austin Bunionectomy
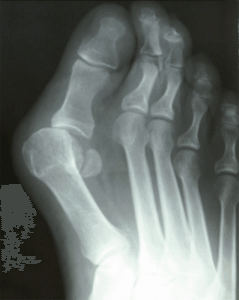
What is a bunion?
A bunion is a genetically inherited foot structure that leads to migration of your 1st metatarsal. The bunion itself is where the 1st metatarsal begins to protrude out the medial or inside of the foot. Nothing actually grows or forms new bone, but it is the deviation of the normal bone that creates the bunion. The bunion can continue to rotate and get larger until it creates hammer toes of the other digits. The bunion eventually causes pain and deformity that needs to be addressed surgically.
One of the most common bunion surgeries is a head procedure. This involves cutting the metatarsal bunion and the end closest to the toe. The bone is then shifted back into place and held with a screw. This procedure works well for mild to moderate bunions and has a fairly quick recovery. The patient can walk the entire time and return to activities much sooner than other procedures.
Outcomes:
The typical bunion surgery has a 5% recurrence rate. The majority of the bunions that return are from not following post-op instructions or other foot factors. It is important to have your surgeon address all other components of your foot and procedure selection should be based on these findings. An x-ray is vital for procedure planning and an overall foot exam to help determine what other pathologies are present.
If you are suffering from bunion pain make an appointment today and I can help you get back to the activities you enjoy!
Give us a call at 425-391-8666 or make an appointment online today.
Dr. Brandon Nelson, A Board-Certified Surgeon, Discusses the Austin Bunionectomy

What is a bunion?
A bunion is a genetically inherited foot structure that leads to migration of your 1st metatarsal. The bunion itself is where the 1st metatarsal begins to protrude out the medial or inside of the foot. Nothing actually grows or forms new bone, but it is the deviation of the normal bone that creates the bunion. The bunion can continue to rotate and get larger until it creates hammer toes of the other digits. The bunion eventually causes pain and deformity that needs to be addressed surgically.
One of the most common bunion surgeries is a head procedure. This involves cutting the metatarsal bunion and the end closest to the toe. The bone is then shifted back into place and held with a screw. This procedure works well for mild to moderate bunions and has a fairly quick recovery. The patient can walk the entire time and return to activities much sooner than other procedures.
Outcomes:
The typical bunion surgery has a 5% recurrence rate. The majority of the bunions that return are from not following post-op instructions or other foot factors. It is important to have your surgeon address all other components of your foot and procedure selection should be based on these findings. An x-ray is vital for procedure planning and an overall foot exam to help determine what other pathologies are present.
If you are suffering from bunion pain make an appointment today and I can help you get back to the activities you enjoy!
Give us a call at 425-391-8666 or make an appointment online today.
Dr. Brandon Nelson, A Board Certified Surgeon, Discusses Neuroma Surgery
Neuromas are a common presenting pathology in my office. I see quite a few in the typical week. The majority of patients with neuromas are female between the ages of 40-60. The patient will usually describe burning or tingling in the foot that is worse with shoes. Most of the time on exam one can feel the nerve moving, this is called a “Molder’s click”. I will usually get an x-ray and then help the patient with a long-term plan.
There are a few conservative modalities that work fairly well for a neuroma and I usually recommend trying these before proceeding to surgery. However, often times patients have tried these and are seeing me as a second opinion.
Surgery is relatively straight forward for a neuroma. The majority of us use a incision on the top of the foot that is about 3 inches long and provides great exposure to the nerve. The nerve is removed, and the entire procedure takes about 15 minutes. I let my patients walk after surgery and most are able to tolerate the discomfort from surgery with just an oral anti-inflammatory.
If you have burning or tingling in your foot or have been diagnosed with a neuroma I can help. Make an appointment today and we can review your options and get you back on your feet pain free.
Give us a call at 425-391-8666.
Why Do I Have Blisters on My Feet?
 Most blisters form on the feet due to friction. As you walk, your shoes or socks may rub against a small area of skin, damaging it. A pocket of fluid builds up underneath the damaged skin to shield the deeper layers of skin from further damage. Friction blisters are best left alone and footwear and activity modifications are often adequate for treating symptoms and preventing future blisters. However, not all foot blisters are caused by friction. Blisters can also occur on the feet due to allergic reactions, exposure to certain chemicals, skin conditions like eczema, frostbite, sunburn, and fungal, viral, or bacterial infections. If you frequently have blisters on your feet, a podiatrist can help you determine the cause of your blisters and find the best treatment for you.
Most blisters form on the feet due to friction. As you walk, your shoes or socks may rub against a small area of skin, damaging it. A pocket of fluid builds up underneath the damaged skin to shield the deeper layers of skin from further damage. Friction blisters are best left alone and footwear and activity modifications are often adequate for treating symptoms and preventing future blisters. However, not all foot blisters are caused by friction. Blisters can also occur on the feet due to allergic reactions, exposure to certain chemicals, skin conditions like eczema, frostbite, sunburn, and fungal, viral, or bacterial infections. If you frequently have blisters on your feet, a podiatrist can help you determine the cause of your blisters and find the best treatment for you.
Blisters may appear as a single bubble or in a cluster. They can cause a lot of pain and may be filled with pus, blood, or watery serum. If your feet are hurting, contact the podiatrists of Issaquah Foot & Ankle Specialists. Our doctors can provide the care you need to keep you pain-free and on your feet.
Foot Blisters
Foot blisters are often the result of friction. This happens due to the constant rubbing from shoes, which can lead to pain.
What Are Foot Blisters?
A foot blister is a small fluid-filled pocket that forms on the upper-most layer of the skin. Blisters are filled with clear fluid and can lead to blood drainage or pus if the area becomes infected.
Symptoms
(Blister symptoms may vary depending on what is causing them)
- Bubble of skin filled with fluid
- Redness
- Moderate to severe pain
- Itching
Prevention & Treatment
In order to prevent blisters, you should be sure to wear comfortable shoes with socks that cushion your feet and absorb sweat. Breaking a blister open may increase your chances of developing an infection. However, if your blister breaks, you should wash the area with soap and water immediately and then apply a bandage to the affected area. If your blisters cause severe pain it is important that you call your podiatrist right away.
If you have any questions, please feel free to contact one of our offices located in Issaquah, WA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Blisters
Blisters are pockets of fluid that occur under the top layer of your skin. These fluid pockets are usually filled with pus, blood, or serum. Blisters may itch or hurt and can appear as a single bubble or in clusters.
The most common types of blisters are friction blisters. This type of blister may be caused by wearing shoes that are too tight. Friction blisters can also occur on the hands. A change in temperature may also cause blisters on the feet. In the freezing air, frostbite on your toes can lead to blisters, as well as sunburn from hot weather.
The best way to treat a blister is to keep it clean and dry. Most blisters will get better on their own. Once the skin absorbs the fluid within the blister, it will flatten and eventually peel off. You should avoid popping your blister unless you podiatrist does it for you. Additional treatment options include applying an ice pack to the blister or using over-the-counter blister bandages to cover the affected area.
If your blister becomes discolored, inflamed, or worsens it is advised that you speak to your podiatrist. Blisters that are yellow, green, or purple may be infected and require immediate medical attention. Blisters that are abnormally colored may be a sign of a more serious underlying health condition such as herpes.