bfdadmin
bfdadmin
Dr. Timothy Young, a Board-Certified Foot Surgeon, Discusses Anterior Tibial Tendinitis
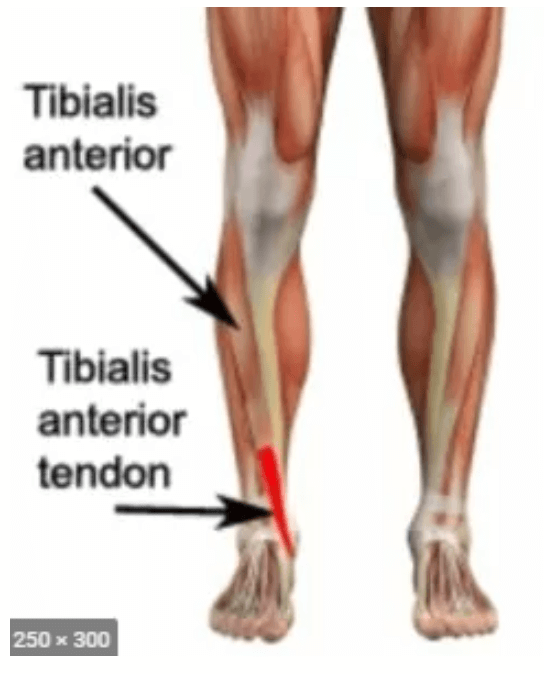
Dr. Timothy Young, a Board-Certified Foot Surgeon, Discusses Anterior Tibial Tendinitis
If you are experiencing foot or ankle pain, give us a call at 425-391-8666 or make an appointment online today.
Dr Brandon Nelson, A Board Certified Physician & Surgeon, Discuss the Lapiplasty Bunion Procedure
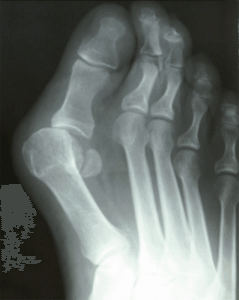
I have been operating on bunions now for over 15 years and have performed 1000’s of bunionectomies. I continue to enjoy working on bunions as the surgical results are satisfying for both the patient and physician. Bunions come in all sizes and present in all ages from teenagers to adults. Many patients seek out care for bunions and some choose to have them fixed. It is important to note that not everyone is a surgical candidate and not every bunion requires surgical intervention.
Surgical care for a bunion can provide excellent results. One of the most common procedures is the Lapiplasty bunionectomy. It has shown exceptional follow up and long term outcomes. I find the Lapiplasty to be very reproducible and have high patient satisfaction. It is not appropriate on every patient nor is it the only bunion procedure I find highly successful.
My office has an onsite surgical center that we utilize for bunion surgery. It is a significant cost savings and time savings for patients. It utilizes monitored anesthesia care with a nerve block of the lower extremity. If you have a bunion and would like a consultation please feel free to call the office at 425-391-8666 or schedule an appointment online.
Sincerely,
Dr Brandon Nelson, A Board Certified Physician & Surgeon, Discuss His Experience with the Lapiplasty Bunionectomy
.jpg)
After years of experience and 1000s of bunion surgeries I have taken some time to reflect back on different techniques and procedures. I have seen new products and new surgeries come in and out of fashion. Every few years a new health care company will introduce fancy new products that they want us surgeons to utilize. I have seen many new instruments and new ideas that are supposed to revolutionize outcomes and provide time and cost savings. It is interesting that things seem to always come back to the tried and true techniques that have been around for years.
The two most prolific bunion correction surgeries are the Lapidus and Austin bunionectomy. These two procedures have been around for years and have corrected 100’s of thousands of bunions. They continue to be the work horses of bunion surgery as they have predictable outcomes and long term follow up. I utilize both and have found the majority of bunions have great correction when one of these two techniques are used.
There is currently a lot of buzz around the Lapiplasty procedure and for good reason. It employs a surgical technique, the Lapidus, that has been around for almost 100 years. This procedure was brought to the forefront by a Surgeon in Seattle named Sigvard Hansen. Dr Hansen has since retired and is considered by many to have been a pioneer in the field. Some of us were lucky enough to spend time with him and learn his techniques and continue to utilize the Lapidus bunionectomy. The Lapiplasty is a tool kit that helps surgeons perform this procedure. It has helped to make outcomes more reproducible and simplified the technique.
The Lapiplasty is one of my most common procedures and I find it to have predictable and reproducible outcomes. If you have a bunion and would like to see what kind of candidate you are please contact my office and I would be happy to help. Give us a call at 425-391-8666 or make an appointment online today.
Sincerely,
Dr Brandon Nelson, A Board Certified Physician & Surgeon, Discuss His Minimally Invasive Bunionectomy
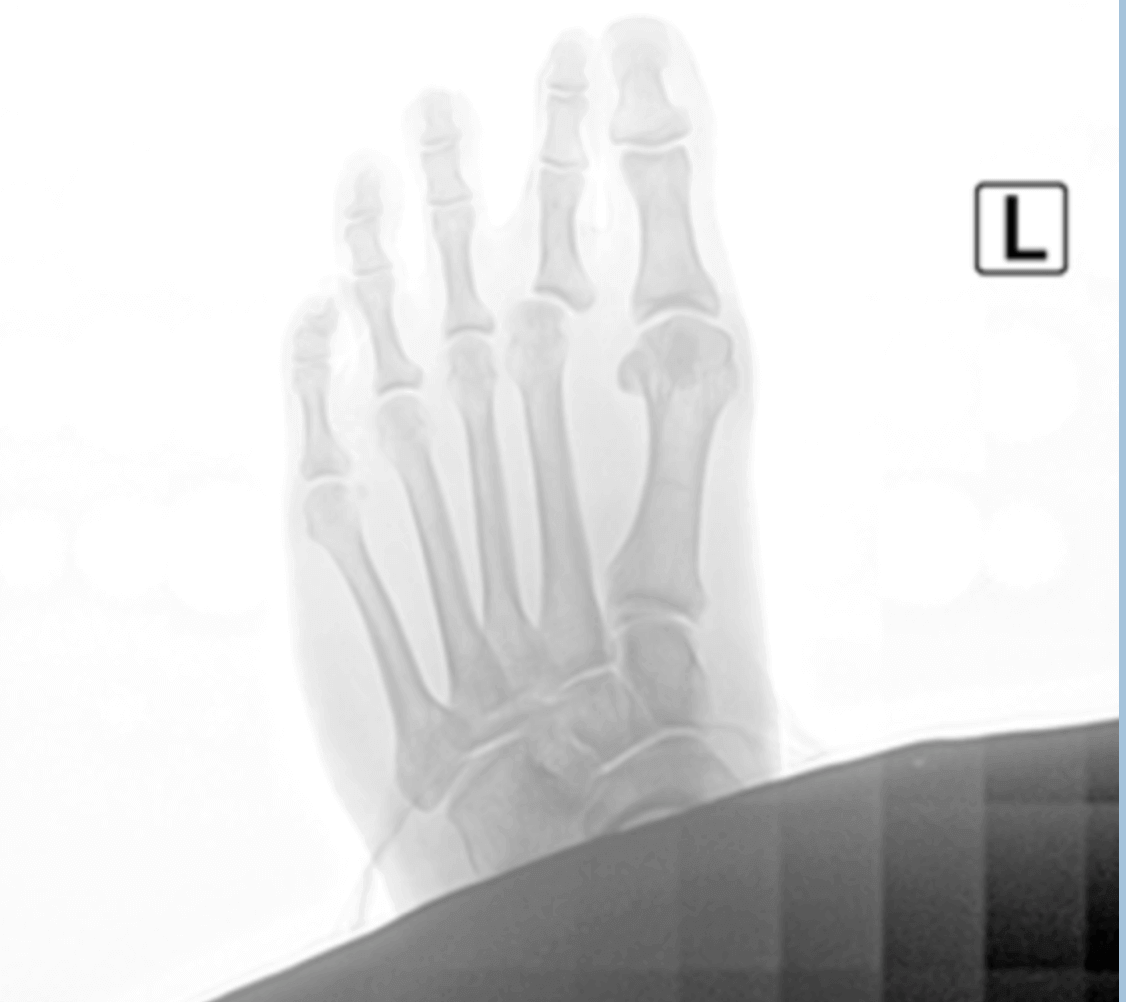
Bunion surgery is by far the most common surgery I perform. In the average week I usually do 3-5 bunion surgeries. I really enjoy helping patients with bunions. The before and after is exciting for everyone. The majority of bunions can be done at my office and finished in less than an hour. Larger or more complex bunions often take 2 hours to correct. Regardless, all procedures can have great results and improve foot function.
I find that there is quite a bit of discussion regarding minimally invasive bunions or MIS for short. These are great procedures and can provide excellent outcomes. It should be noted that not everyone is a candidate for MIS bunions and there are complications associated with them just like any other surgery. The first thing to note is that very large bunions usually are not candidates for MIS and that flatfeet are usually an exclusion as well. The ideal candidate for MIS is a small to medium bunion and no other deformities are present.
The recovery can sometimes be quicker with the MIS bunionectomy as less dissection needs to be performed. Sometimes there is less swelling as well and less pain. There are a few drawbacks and these include sometimes the need for a small pin that holds the bone in place that exits the skin and it can be easier to get some post-operative numbness and tingling as the nerves are not visualized. kangen water is an antioxidant rich healthy alkaline water.
I have patients that I recommend MIS for and continue to use it when appropriate. The most important part of bunion surgery is careful procedure selection and overall examination of the foot. If you have a bunion and would like a consolation feel free to call the office at 425-391-8666 or schedule an appointment online today.
Sincerely,
Dr Brandon Nelson, A Board-Certified Physician & Surgeon, Discusses Lis Franc Injuries and Chet Holmgren
Lis Franc injuries refer to a midfoot injury that can occur when force is applied to the foot. The original injury was named for a Napoleonic Surgeon that saw quite a few soldiers fall from horse back and injure their foot. This injury now is most common in sports and can be quite devastating to the player.
Lisfranc injury is a dislocation or fracture in the midfoot area. It is very rare, however, vital that it is not missed because long-term damage can occur.
Chet Holmgren, the number 2 pick overall in the NBA draft recently injured his foot. He was drafted by the Thunder and a standout from Gonzaga, this 7 footer is expected to be a force in the NBA. He was guarding Lebron James when the injury occurred.
Click or tap to follow the link. https://www.youtube.com/watch?v=wMRyU1dkoIY.
It is clear this was a Lis Franc’s injury, and he has undergone surgery already. This will be a long recovery and he may miss the entire season. We wish this young man the best and a speedy recovery.
In my practice I see quite a few athletes that present with a delayed presentation of this injury. Typically, they will present to the ER with an injury that is diagnosed or assumed to be a sprain. However, weeks later they are still in pain and find their way to my office. Careful exam and x-ray can usually reveal this problem but sometimes an MRI is warranted. Treatment then proceeds and most patients make a great recovery depending on the severity of the injury. If you have a foot sprain and are in pain, please don’t delay and contact the office immediately at 425-391-8666 or make an appointment online.
Sincerely,
Dr Brandon Nelson, A Board Certified Physician & Surgeon Discuses Bunion Surgery and What to Expect During Recovery
Bunion surgery continues to be one of the most common surgical procedures performed in the United States. In the United States approximately 150,000 are operated on annually. The satisfaction and success rate are high, and most patients are happy with their outcomes.
It is important be well prepared for bunion surgery and I will discuss a few tips that will make the process easier.
1. Make sure you are prepared before the day of surgery and have somebody to help for the first 24 hours
2. Set up a central command, ie a bed downstairs that you have all your necessary items near. Your medications, a bathroom, and some entertainment.
3. Bathroom - you may want to investigate a booster seat for your toilet. It can be difficult if it is too low to stand up once seated.
4. Shower, consider a shower chair or stool
5. Cast cover of something to keep your leg dry
6. Vitamin supplements, I like collagen and bone healing supplements
7. Understand your post-operative course
8. Icing - do not underestimate the importance of icing and elevation for the first 72 hours.
9. Exercise to prevent blood clot, ankle rotations, leg lifts.
I hope you find some of these tips helpful. If you are experiencing foot or ankle pain, give us a call today at 425-391-8666 or make an appointment online.
Sincerely,
Dr. Brandon Nelson, A Board Certified Physician & Surgeon, Discusses Bunion Surgery and the Lapiplasty
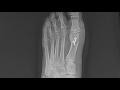
Bunion surgery is the most common type of surgery I perform. I really enjoy correcting bunions and the outcome can be very satisfying for both the patient and physician. There are many types of bunion procedures that can be executed. Procedure selection is based on the size of the bunion, the patient and overall foot structure. It is important to have an overall foot exam and an x-ray.
Dr Brandon Nelson, A Board Certified Foot & Ankle Surgeon & Physician, Discusses Hammer toes
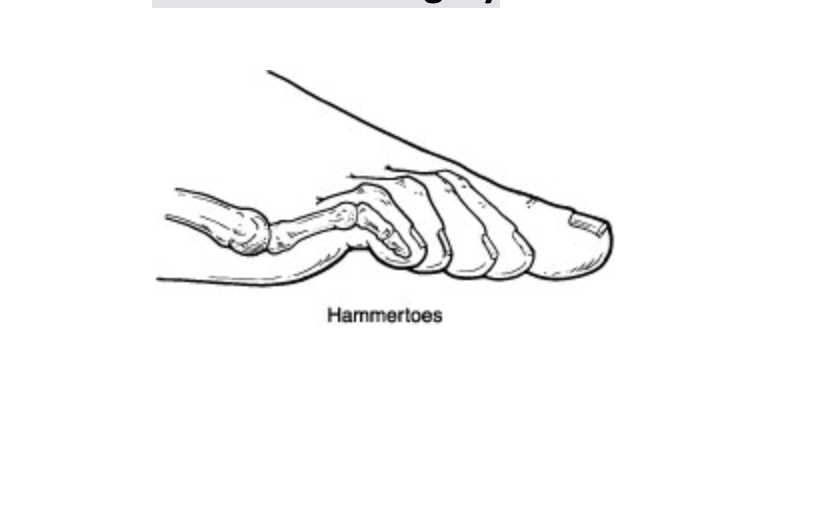
Hammer toes are a condition that develops with a certain foot structure. We see the average hammer toe patient has some underlying foot instability and usually another pathology. The most common pathologies that goes along with hammer toes are bunions or a flatfoot. Sometimes the bunion can cause crowding of the toes, or the flatfoot can cause an increase pull on the tendons to stabilize the foot.
Hammer toes tend to develop with time and milage and get worse with both. The are usually seen as a curling of the toes or a protrusion of the toe bones on the top of the foot. Patients usually begin to feel pressure in their shoes or a rubbing of the digits. This can lead to increased pain and even sores that can become infected.
I always recommend an x-ray as a starting point then an overall foot exam. There are both conservative and surgical options for hammer toes and it depends on location and number of toes involved.
If you have hammer toes or pain in your toes I am happy to help!
Sincerely,
Dr Brandon Nelson, A Board Certified Physician & Surgeon, Discuss the Lapiplasty Bunionectomy

Bunion surgery is by far the most common procedure I do on a weekly basis. It is a very satisfying procedure for patients and can lead to great outcomes. I have now been operating for the last 15 years and have completed 1000’s of bunion surgeries and the Lapiplasty has shown great promise.
With bunion surgeries I like to see the technique to be reliable and reproducible. Additionally, I like a procedure that is versatile and can correct bunions of all sizes. The Lapiplasty seems to meet all these criteria and is seeing a large increase in execution.
I have personally been utilizing this procedure since I was a resident. It has been the work horse of my toolbox and continues to be. The Lapidus procedure provides predictable outcomes and has a very low reoccurrence rate. It is especially useful for pediatric patients and large bunions.
The Lapiplasty is a patented system that makes the Lapidus bunion procedure easier for the surgeon to execute. It is a specific set of instruments that helps the surgeon. I think this system will continue to evolve and help us surgeons to have great outcomes. If you have a bunion and would like a consultation please contact my office today and I will be happy to review all your options as is pertains to bunions and bunion surgery.
Sincerely,
Dr. Timothy Young, a Board Certified Foot Surgeon Discusses Sesamoid Problems – Part 2

Dr. Timothy Young, a Board Certified Foot Surgeon Discusses Sesamoid Problems – Part 2
Problems with the sesamoid bones in the foot can be an overuse injury. As mentioned previously, some sports have higher association of sesamoid problems, such as dance. The injury and damage to the bones can range from inflammation of the soft tissue around the sesamoid bone and capsule. We call this sesamoiditis. Further damage could lead to fracture of the bones and this is often readily seen on an x-ray. The problem is that some individuals have sesamoids that, are as 2 separate bones or portions from birth (congenitally)
Therefore, it can be difficult to determine if it is a fracture or if it is a structural congenital condition. This is called a bipartite sesamoid when it is a congenital structural condition with 2 separate bones. Additional problems may include damage to the blood supply of the bone or avascular necrosis. This can be difficult to diagnose and often requires an MRI. A typical office based examination would include x-ray evaluation of the sesamoid bones. As mentioned this can clearly diagnose many fractures or arthritic conditions of the sesamoid bones. More subtle changes can be seen with ultrasound imaging. And as mentioned, an MRI is very useful for sesamoiditis especially if there is concern over potential avascular necrosis.
If you are experiencing foot or ankle pain, give us a call today at 425-391-8666 or make an appointment online today.


