November 2023
Toe Pain
Toe pain can originate from corns, calluses, hammertoes, and bunions, as well as ingrown toenails, sprains, fractures, and dislocations. Corns develop as the toe rubs against the inside of a shoe which causes the skin to thicken as a form of protection. A corn is typically cone-shaped and has a small, hardened spot that points inward. When a corn is pressed into the skin, the toe becomes painful. Corns usually form on the top or side of the toe. A callus is also a thickened patch of skin that generally forms on the bottom of the foot. Calluses are the result of friction from the toe rubbing against the inside of a shoe. They may also occur by walking barefoot or having flat feet. A hammertoe is a bump on the knuckle of the second toe that is produced by wearing shoes that are too short for your feet. The bony protrusion rubs against the top of the shoe causing pain and irritation. A bunion is a malformation of the big toe. The base of the big toe pushes away from the smaller toes, forcing the top of the big toe to press toward the other toes. Bunions can be hereditary, or they can result from injury to the toe joint or from wearing high heels with a narrow toe box. The toe becomes inflamed, and a bump may develop at the end of the misplaced bone. Ingrown toenails typically affect the big toe and its surrounding skin. The nail will dig into the skin and become painful. Wearing tight or narrow shoes that compress the big toe causes the nail to grow into the fleshy part of the toe. Cutting toenails incorrectly can also add to the development of an ingrown toenail. A toe sprain originates from a torn or stretched ligament. Strapping the injured toe to the toe next to it for stabilization is common. A broken or fractured toe usually occurs from trauma like dropping a heavy object on it or bumping into something extremely hard and rigid. Osteoporosis, a thinning of the bones, can also bring about toe fractures.
Any of the conditions mentioned can lead to pain and irritation. While some are more serious than others, seeking an examination and diagnosis from a podiatrist is a good idea. A podiatrist can treat each ailment and get you back on your feet again without pain.
Turf Toe Can Be a Painful Foot Condition
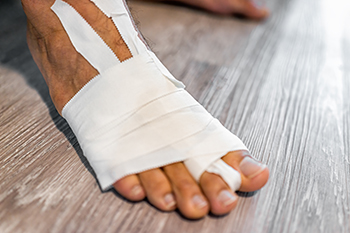
Turf toe is a specific type of injury that primarily affects the big toe. It is a sprain of the metatarsophalangeal, or MTP joint, which connects the big toe to the foot and can result in toe pain. The name turf toe is derived from its common occurrence in athletes who play on artificial turf surfaces, but it can affect anyone. This injury typically occurs when the toe is hyperextended, causing damage to the ligaments and tendons that support the MTP joint. Symptoms of turf toe include pain, swelling, and limited range of motion in the affected toe. In some cases, there may be bruising as well. Turf toe can be a painful and debilitating condition, and often requires medical attention from a podiatrist. If you have endured this type of injury, it is strongly suggested that you are under the care of this type of doctor who can effectively diagnose and treat the cause of this toe pain.
Toe pain can disrupt your daily activities. If you have any concerns, contact the podiatrists of Issaquah Foot & Ankle Specialists. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Causes Toe Pain?
Most severe toe pain is caused due to a sports injury, trauma from dropping something heavy on the toe, or bumping into something rigid. Other problems can develop over time for various reasons.
Toe pain can be caused by one or more ailments. The most common include:
- Trauma
- Sports injury
- Wearing shoes that are too tight
- Arthritis
- Gout
- Corns and calluses
- Hammertoe
- Bunions
- Blisters
- Ingrown toenails
- Sprains
- Fractures (broken bones)
- Dislocations
When to See a Podiatrist
- Severe pain
- Persistent pain that lasts more than a week
- Signs of infection
- Continued swelling
- Pain that prevents walking
Diagnosis
In many cases the cause of toe pain is obvious, but in others, a podiatrist may want to use more advanced methods to determine the problem. These can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatments for toe pain and injuries vary and may include shoe inserts, padding, taping, medicines, injections, and in some cases, surgery. If you believe that you have broken a toe, please see a podiatrist as soon as possible.
If you have any questions please feel free to contact one of our offices located in Issaquah, WA . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
How to Treat Your Toenail Fungus
While not a serious issue, toenail fungus, or onychomycosis, can be an embarrassing and uncomfortable condition to experience. Toenail fungus is often caused from public areas that harbor fungi and improper cleaning/drying of the foot. Once infected, the fungus grows deeper into the nail and can be very hard to get rid of.
There are different types of fungus that cause toenail fungus. Dermatophytes, yeasts, and molds are the most frequent forms of fungus to infect the toenail. Dermatophytes are the most common among the three. Symptoms associated with fungal nails include the discoloration of the toenail, brittleness, and in some circumstances, a smell. Pain is rarely a symptom caused by toenail fungus.
Diagnosis of fungal nails is generally a rather quick process. However podiatrists will make sure that the cause is not another condition such as lichen planus, psoriasis, onychogryphosis, or nail damage. Podiatrists will make use of fungal cultures and microscopy to verify that it is fungus.
While over-the-counter ointments are readily available, most are ineffective. This is due to the fact that the nail is very protective and that the fungus slips in between the nail plate and bed. Podiatrists can offer oral medication which currently provides the best results.
Ultimately, prevention is the best line of defense against toenail fungus. Avoid unsanitary public showers. If you do use a public shower, use shower shoes to provide your foot with protection. Once you are finished showering, make sure to thoroughly dry your feet. Fungi thrive in warm, dark, and moist places like sweaty, warm feet that are left dark in shoes all day.
Recurrence of Toenail Fungus
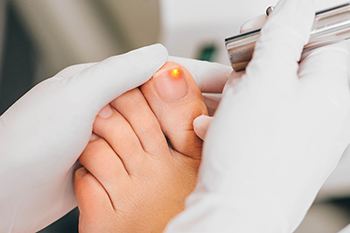
Fungal nail infections, or onychomycosis, affect a significant portion of the population, particularly the toenails. Characterized by discoloration, thickening, and sometimes detachment of the nail from its bed, these infections stem from fungi that invade through tiny breaks in the nail or surrounding skin. Anyone can contract this type of infection, but they are especially common in individuals with certain health conditions, such as diabetes, which predispose them to recurrence. Diagnosis should be professionally confirmed, and while treatments, mainly oral antifungal medications, are available, they can be lengthy and sometimes ineffective, with infections taking months to resolve. Notably, even after successful treatment, fungal nail infections can recur, particularly in people with chronic medical conditions that compromise the immune system or circulation. To manage and prevent recurrence, especially if you are at higher risk for these infections, it is suggested that you make an appointment with a podiatrist for comprehensive treatment and continual monitoring of this condition.
If left untreated, toenail fungus may spread to other toenails, skin, or even fingernails. If you suspect you have toenail fungus it is important to seek treatment right away. For more information about treatment, contact the podiatrists of Issaquah Foot & Ankle Specialists. Our doctors can provide the care you need to keep you pain-free and on your feet.
Symptoms
- Warped or oddly shaped nails
- Yellowish nails
- Loose/separated nail
- Buildup of bits and pieces of nail fragments under the nail
- Brittle, broken, thickened nail
Treatment
If self-care strategies and over-the-counter medications does not help your fungus, your podiatrist may give you a prescription drug instead. Even if you find relief from your toenail fungus symptoms, you may experience a repeat infection in the future.
Prevention
In order to prevent getting toenail fungus in the future, you should always make sure to wash your feet with soap and water. After washing, it is important to dry your feet thoroughly especially in between the toes. When trimming your toenails, be sure to trim straight across instead of in a rounded shape. It is crucial not to cover up discolored nails with nail polish because that will prevent your nail from being able to “breathe”.
In some cases, surgical procedure may be needed to remove the toenail fungus. Consult with your podiatrist about the best treatment options for your case of toenail fungus.
If you have any questions, please feel free to contact one of our offices located in Issaquah, WA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Dr Brandon Nelson, A Board-Certified Physician & Surgeon Discusses The Lapiplasty Bunion Procedure
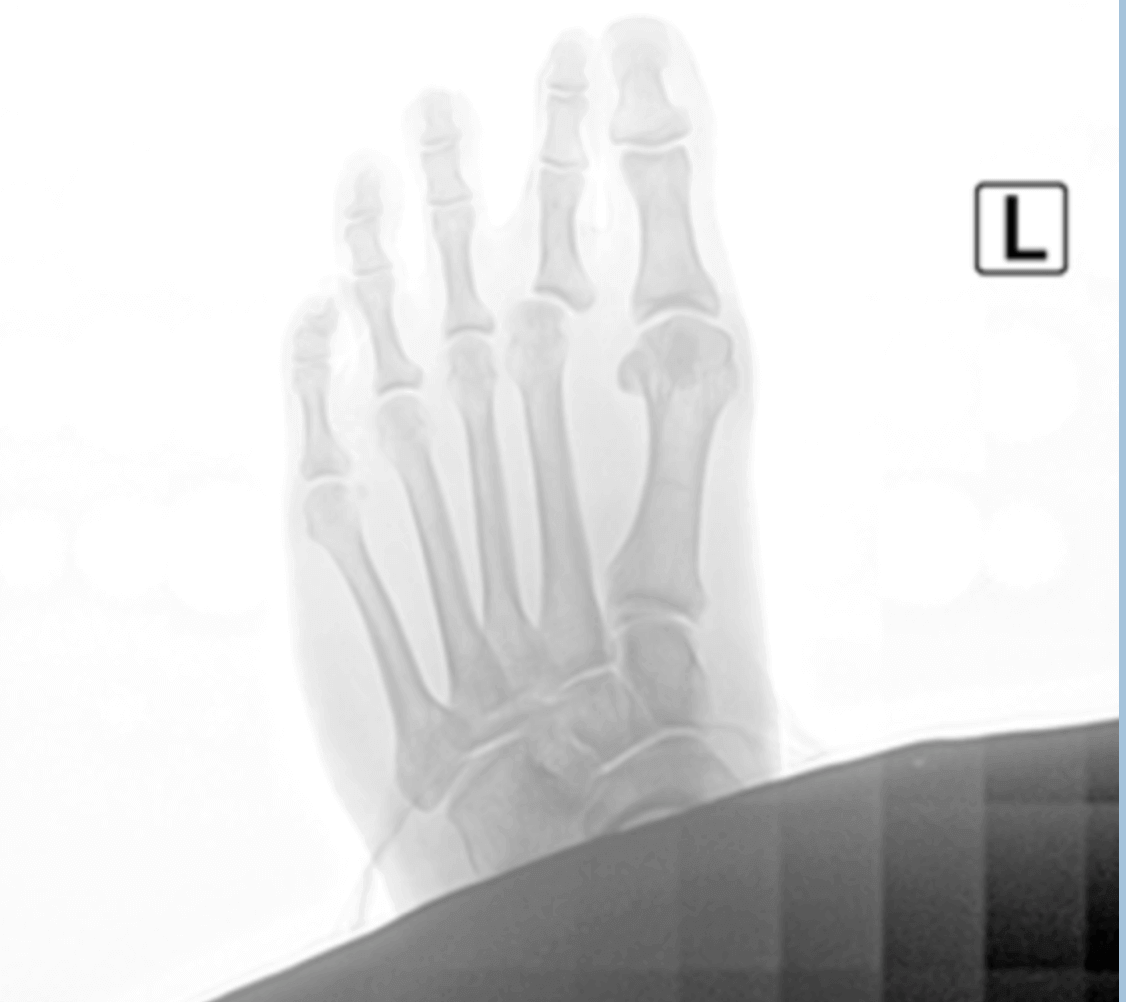
Dr Brandon Nelson, A Board-Certified Physician & Surgeon Discusses The Lapiplasty Bunion Procedure
Bunion and bunion pain affects millions of people per year. It creates pain around your big toe and can decrease quality of life. The pain can become so intense or make it difficult to wear shoes often people would like it removed. Bunion surgery has been around for over 100 years however recently a new technique called the Lapiplasty has changed the recovery times and improved outcomes.
The lapiplasty is a 3-D bunion correction system that has helped to address the bunion at its origin. This procedure works to stabilize the foot and realign the metatarsal bone. It has been shown to have very low recurrence rates and great long-term outcomes.
There are a few reasons it has proved to be a game changer. One, is correcting the bunion deformity by fixing both the angular and rotational deformity of the bunion. Two, it has a faster recovery over the traditional bunion surgery. Three, it reduces complications including stiffness and improved joint stability.
I have found this new system to be revolutionary for my patients. I find it to be the future of bunion surgery. If you would like a consultation on your bunion I can help. Call to make an appointment with me at 425-391-8666 or schedule an appointment online.
Dr. Timothy Young, a Board Certified Foot Surgeon, Discusses My Top 5 Reasons Why I Recommend the Lapiplasty Bunion Repair
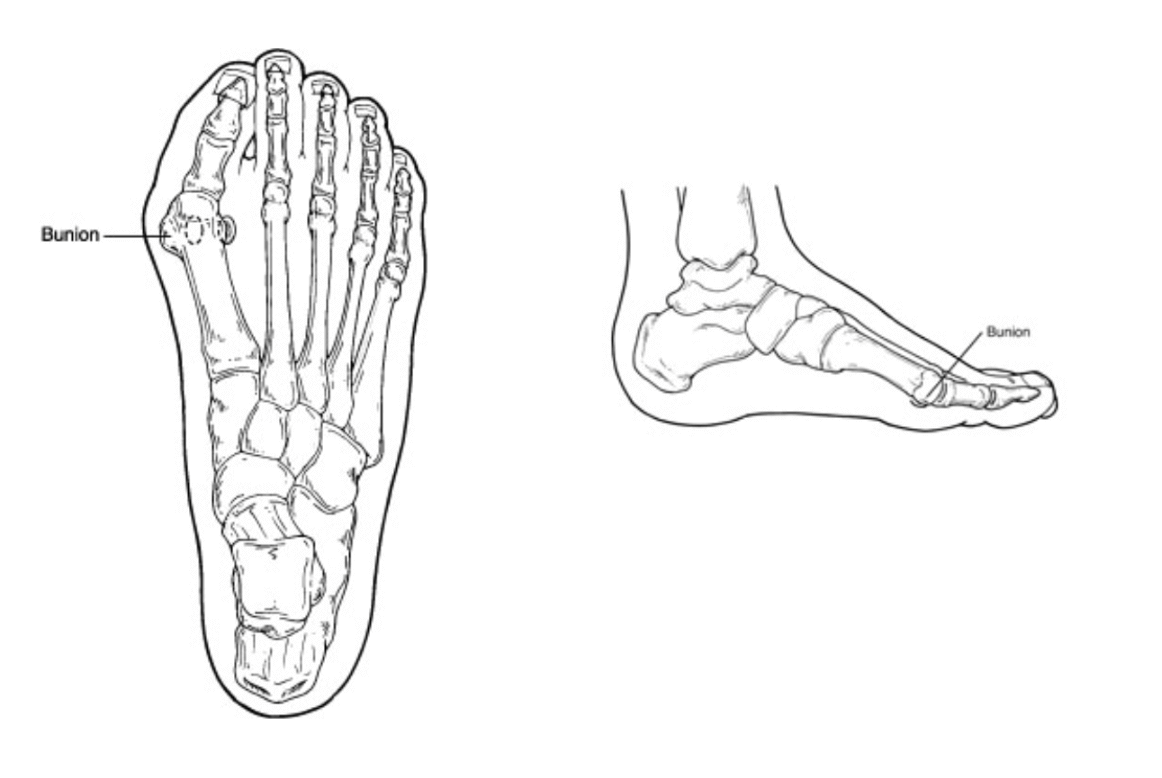
Dr. Timothy Young, a Board Certified Foot Surgeon, Discusses My Top 5 Reasons Why I Recommend the Lapiplasty Bunion Repair
Introduction
Bunions can be painful and disruptive, affecting the quality of life for many individuals. Traditional bunion surgery, also known as a bunionectomy, has been the standard approach for decades. However, in recent years, a groundbreaking surgical technique called Lapiplasty has emerged as a game-changer in the field of bunion repair. Surgeons worldwide are increasingly recommending Lapiplasty for several compelling reasons. In this blog, I will review the top 5 reasons why I recommend the Lapiplasty Procedure for bunion surgery.
1. Superior Three-Dimensional Correction
One of the most remarkable aspects of Lapiplasty is its ability to correct bunions in three dimensions, addressing the root cause of the deformity. Traditional bunion surgery often focuses on the visible bony bump, leaving the underlying bone misalignment uncorrected. Lapiplasty, on the other hand, repositions the metatarsal bone, restoring its proper alignment in all three planes—sagittal, transverse, and frontal. This three-dimensional correction not only provides better cosmetic results but also reduces the risk of bunion recurrence, making it a preferred choice among surgeons.
2. Faster Recovery and Reduced Downtime
Lapiplasty's minimally invasive approach and stable fixation results in faster recovery times for patients. Unlike traditional bunion surgery, which often requires patients to remain off their feet for an extended period, Lapiplasty allows patients to bear weight on their feet and start walking within days. This accelerated recovery can significantly improve a patient's overall experience and quality of life during the healing process.
3. Long-Lasting Results
Surgeons recommend Lapiplasty due to its track record of providing more durable and longer-lasting results. Traditional bunion surgery may offer temporary relief, but recurrence rates can be high. The Lapiplasty's comprehensive correction of the deformity decreases the likelihood of bunions returning, allowing patients to enjoy a more permanent solution to their foot pain.
4. Stable Fixation
The Lapiplasty utilizes very stable plates. These allow earlier weightbearing and return to activities. This fixation helps to promote optimal bone healing and long term stability. Surgeons who recommend Lapiplasty often highlight the fixation benefits of this innovative technique, which can boost patients' confidence and satisfaction with their results.
5. Evidence-Based Success
Surgeons have confidence in recommending Lapiplasty due to the strong evidence supporting its success. Numerous clinical studies and real-world cases have demonstrated the effectiveness of this procedure in addressing bunions, relieving pain, and improving patient outcomes. These data-driven results reassure both surgeons and patients that Lapiplasty is a reliable and proven treatment option.
Conclusion
Lapiplasty has revolutionized the field of bunion repair with its three-dimensional correction, quicker recovery times, long-lasting results, stable fixation, and evidence-based success. Surgeons worldwide recommend Lapiplasty as a superior alternative to traditional bunion surgery for patients seeking a more comprehensive and permanent solution to their foot pain. If you're considering bunion repair, please contact my office so I can evaluate your specific needs and discuss the benefits of Lapiplasty as a potential solution to your bunion woes.
If you are experiencing foot or ankle pain, give us a call at 425-391-8666 or make an appointment online today.
All About Plantar Warts
Plantar warts are warts that are only found on the feet, hence the term “plantar”, which means “relating to the foot.” They are caused by the human papillomavirus, or HPV, and occur when this virus gets into open wounds on the feet. The warts themselves are hard bumps on the foot. They are easily recognizable, mostly found on the heels or ball of the foot. Plantar warts are non-malignant, but they can cause some pain, discomfort, and are often unsightly. Removing them is a common step toward treating them.
Plantar warts can cause some pain while standing, sometimes felt as tenderness on the sole of your foot. Unless the wart has grown into the foot behind a callus, you will be able to see the fleshy wart. A podiatrist should only be consulted if there is an excessive amount of pain. Plantar warts are not cancerous or dangerous, but they can affect your walking and continually reappear. Anyone who suffers from diabetes or a compromised immune system disease should seek out care immediately.
Podiatrists are easily able to diagnose plantar warts. They usually scrape off a tiny bit of the rough skin to make tiny blood clots visible and examine the inside of warts. However, a biopsy can be done if the doctor is not able to diagnose them from simply looking at them. Although plantar warts usually do not require an excessive amount of treatment, there are ways to go about removing them. A common method is to freeze them off using liquid nitrogen, removing them using an electrical tool, or burning them off via laser treatment. For a less invasive treatment option, topical creams can be used through a doctor’s prescription. This treatment method takes more time, however. Keep the wart covered for protection in between daily treatments.
The best way to avoid developing plantar warts is to avoid walking barefoot in public places. Avoid this especially if you have open sores or cuts on your feet. It is also important to avoid direct contact with warts in general, as they are highly contagious.
Definition and Risk Factors of Plantar Warts

Plantar warts, small growths caused by the human papillomavirus, or HPV, often appear on the soles of the feet. Unlike common warts, which typically grow on the hands, plantar warts can be painful due to the pressure exerted on the soles when walking or standing. These warts may have a rough, grainy appearance with tiny black dots, which are actually clotted blood vessels. Several risk factors increase the likelihood of developing plantar warts. Close contact with the virus, such as walking barefoot in damp and communal areas like locker rooms, swimming pools, or public showers, can put your feet at risk. Additionally, those with a weakened immune system, such as individuals with diabetes or HIV, are more susceptible to plantar warts. Constantly moist or sweaty feet can provide an ideal environment for the virus to thrive. If you have developed a plantar wart, it is strongly suggested that you consult a podiatrist who can provide relief with appropriate treatment methods.
Plantar warts can be very uncomfortable. If you need your feet checked, contact the podiatrists from Issaquah Foot & Ankle Specialists. Our doctors will assist you with all of your foot and ankle needs.
About Plantar Warts
Plantar warts are the result of HPV, or human papillomavirus, getting into open wounds on the feet. They are mostly found on the heels or balls of the feet.
While plantar warts are generally harmless, those experiencing excessive pain or those suffering from diabetes or a compromised immune system require immediate medical care. Plantar warts are easily diagnosed, usually through scraping off a bit of rough skin or by getting a biopsy.
Symptoms
- Lesions on the bottom of your feet, usually rough and grainy
- Hard or thick callused spots
- Wart seeds, which are small clotted blood vessels that look like little black spots
- Pain, discomfort, or tenderness of your feet when walking or standing
Treatment
- Freezing
- Electric tool removal
- Laser Treatment
- Topical Creams (prescription only)
- Over-the-counter medications
To help prevent developing plantar warts, avoid walking barefoot over abrasive surfaces that can cause cuts or wounds for HPV to get into. Avoiding direct contact with other warts, as well as not picking or rubbing existing warts, can help prevent the further spread of plantar warts. However, if you think you have developed plantar warts, speak to your podiatrist. He or she can diagnose the warts on your feet and recommend the appropriate treatment options.
If you have any questions, please feel free to contact one of our offices located in Issaquah, WA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Dr Brandon Nelson, A Board Certified Physician and Surgeon, Discussed When Your Heel Pain Will Not Go Away and You Need A Second Opinion

Heel pain can be difficult for patients and physicians alike. It can provide a challenge for all parties involved. I have seen hundreds or maybe even thousands of second opinions for heel pain. Over the years I have learned many valuable lessons that can be extremely beneficial to treating heel pain.
One of the first lessons I learned was to listen to the patient. Often patients provide great clues to the cause and origin of heel pain. The history and story a patient tells often paints the perfect picture for how the pain is continuing to cause discomfort. Not all heel pain is the same and although plantar fasciitis is the number one cause remain open to other sources. This leads me to lesson number two.
Lesson number two not all heel pain is plantar fasciitis. I have seen so many other causes and as a provider we need to be diligent. The back can be a source of chronic heel pain. Patients with back issues can have manifestations in the feet. Another common cause is nerve pain. Over the years I would say this is the most common reason heel pain does not get better. The clinician is missing a nerve entrapment. This is not all of the other reasons for heel pain but a few examples to illustrate the importance of recognizing there are other sources of heel pain.
Lesson three is to understand not all heel pain can be treated the same. I have seen patients over the years that have similar heel pain but similar treatments do no work. This is why it is important to treat all patients as individuals. To make sure to look at foot structure, gait cycles and daily routines to see how each individual can be treated for the best possible outcome.
If you have heel pain and are in need of a second opinion or are just fed up with daily pain make an appointment with me today I can help. Give us a call at 425-391-8666 or make an appointment online.
Sincerely,
Dr Brandon Nelson, A Board Certified Physician & Surgeon, Discusses Why the Lapiplasty Procedure for Bunion Surgery Is His Preferred Method

Bunion surgery has been around for over 100 years. There are many techniques that have been utilized for correction of a bunion. The majority involve cutting a bone and realigning a joint. The goal of these surgeries are to straighten the 1st metatarsal and eliminate the deviation of the bone. Today with new research and modern technology we have a better understanding of function anatomy and have begun to look at bunion surgery outcomes. This has led the majority of us surgeons to utilizing the Lapiplasty technique for better long term outcomes.
I personally have been a Lapidus surgeon for over 15 years. I trained in the Northwest and have had the opportunity to work with some of the pioneers of bunion surgery. We have seen through research that the Lapidus procedure holds up the best over time. The long term outcomes show very little recurrence and better overall patient happiness. The lapiplasty system has allowed us to take the lapidus bunion procedure and make it more reproducible.
Lapiplasty is a system created by Treace Medical that has taken some of the technically challenging parts of the lapidus bunionectomy and simplified them. It has a system of cutting jigs and guides that make it simple to correct the bunion. I find patients are extremely happy and have seen incredible long term results. If you have a bunion schedule and appointment with me, I can help you review your options. Give us a call at 425-391-8666 or make an appointment online today.
Sincerely,


