June 2021
Dr. Young Discusses Shockwave Therapy Treatment for Plantar Fasciitis
The shockwave therapy is part of what we call regenerative medicine. Typically, 5 treatments of shockwave are done at weekly intervals. This actually helps the damaged tissue and fascia heal rather than just masking the problem. There are a number of pathways with this treatment works including improving the local blood flow to the damaged plantar fascia. The treatment also activates the local It is always critical to continue the other mechanical and supportive measures (Prescription orthotics night splint hoka shoes).
The majority of patients do very well with this protocol. A small number of patients will need an additional limited series of (3) additional shockwave treatments 4–6 months later into the treatment plan.
If for any reason there is not dramatic and 90% plus improvement then an MRI evaluation is recommended.
Give us a call at 425-391-8666 or make an appointment online today.
Dr. Brandon Nelson Discusses Heel Pain

Heel pain can be extremely frustrating and challenging to treat. It is most often caused by plantar fasciitis, bursitis, or a stress fracture. It is important to find out the underlying cause before treatment and I highly recommend seeing a foot and ankle specialist before initiating and sort of treatment.
Bursitis, this is basically and inflammation of a sac that is used to cushion the foot. Typically, you will have similar symptoms to plantar fasciitis. Patients experience pain in the morning or with standing and after rest. It can be hard to differentiate from plantar fasciitis. However, at our clinic we have an ultrasound unit which we can use to visualize the bursa and help initiate treatment.
Stress fractures are usually seen after one begins to exercise. There can be accompanying swelling and stiffness. This pathology hurst constantly and can lead to a complete fracture. It is vital to get an x-ray and confirm the diagnonsis.
Heel pain or plantar fasciitis is the most common cause and can be variable in presentation. Classically, patients experience pain in the morning that gets better with a few steps. Most patients have increased activity levels and find pain returns whenever they rest and get us. There is a direct correlation with early intervention and a shorter duration of symptoms. I highly recommend getting in as early as possible to see your foot and ankle physician.
If you are suffering with heal pain I can help, come see me today. Give us a call at 425-391-8666 or make an appointment online today.
Children Limping May Indicate Sever’s Disease
 Active children may be more likely to experience heel pain. This pain can be indicative of a condition known as Sever’s disease, and it often affects children and young adolescents. This uncomfortable ailment affects the growth plate in the heel and can occur as a result of extensive pressure exerted on the area where the Achilles tendon meets the heel. Parents may notice their child limping, in addition to experiencing a decrease in flexibility. Prompt treatment generally begins with stopping the activity that caused this condition, and it is beneficial to rest the affected foot. Some children find it may help to perform specific stretches that target the Achilles tendon and calf. If you notice your child has symptoms of Sever’s disease, it is strongly suggested that you schedule a consultation with a podiatrist who can determine what the most effective treatment is.
Active children may be more likely to experience heel pain. This pain can be indicative of a condition known as Sever’s disease, and it often affects children and young adolescents. This uncomfortable ailment affects the growth plate in the heel and can occur as a result of extensive pressure exerted on the area where the Achilles tendon meets the heel. Parents may notice their child limping, in addition to experiencing a decrease in flexibility. Prompt treatment generally begins with stopping the activity that caused this condition, and it is beneficial to rest the affected foot. Some children find it may help to perform specific stretches that target the Achilles tendon and calf. If you notice your child has symptoms of Sever’s disease, it is strongly suggested that you schedule a consultation with a podiatrist who can determine what the most effective treatment is.
Sever's disease often occurs in children and teens. If your child is experiencing foot or ankle pain, see the podiatrists from Issaquah Foot & Ankle Specialists. Our doctors can treat your child’s foot and ankle needs.
Sever’s Disease
Sever’s disease is also known as calcaneal apophysitis, which is a medical condition that causes heel pain I none or both feet. The disease is known to affect children between the ages of 8 and 14.
Sever’s disease occurs when part of the child’s heel known as the growth plate (calcaneal epiphysis) is attached to the Achilles tendon. This area can suffer injury when the muscles and tendons of the growing foot do not keep pace with bone growth. Therefore, the constant pain which one experiences at the back of the heel will make the child unable to put any weight on the heel. The child is then forced to walk on their toes.
Symptoms
Acute pain – Pain associated with Sever’s disease is usually felt in the heel when the child engages in physical activity such as walking, jumping and or running.
Highly active – Children who are very active are among the most susceptible in experiencing Sever’s disease, because of the stress and tension placed on their feet.
If you have any questions, please feel free to contact one of our offices located in Issaquah, WA . We offer the newest diagnostic and treatment technologies for all your foot and ankle injuries.
Sever's Disease
Sever’s disease, also known as calcaneal apophysitis is a common bone disorder that occurs during childhood. The disease is defined as an inflammation of the growth plate in the heel. When a child has a growth spurt, his heel bone grows faster than the muscles, tendons, and ligaments in his leg. This disease is a result of overuse. The people who are most likely to be affected by this disease are children who are in a growth spurt, especially boys who are from the ages of 5 to 13 years old. 60% of children with Sever’s disease have both heels involved.
Symptoms of this disease are heel pain that intensifies during running and jumping activities. The pain is typically localized to the posterior part of the heel. Symptoms may be severe, and they can easily interfere with daily activities. Children who play soccer, baseball, and basketball are more likely to develop Sever’s disease.
Your doctor will diagnose your child based on his or her symptoms, x-rays are generally not helpful in diagnosing this disease. Your doctor may examine both heels and ask your child questions about his or her activity level in sports. Your doctor may then use the squeeze test on your child’s heel to see if there is any pain. Nevertheless, some doctors might still use x-rays to rule out any other issues such as fractures, infections, and tumors.
Sever’s disease can be prevented by maintaining good flexibility while your child is growing. Another prevention method is to wear good-quality shoes that have firm support and a shock-absorbent sole. Sever’s disease can be treated by ceasing any activity that causes heel pain. You should apply ice to the injured heel for 20 minutes 3 times a day. Additionally, orthotics should be used for children who have high arches, flat feet, or bowed legs.
If you suspect your child has Sever’s disease, you should make an appointment with your podiatrist to have his or her foot examined. Your doctor may recommend nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen or naproxen to relieve pain. In more severe cases, your child may need a cast to rest his or her heel. Fortunately, Sever’s disease does not cause long-term foot problems. After treatment, your child should start to feel better within two weeks to two months.
Dr. Timothy Young, a Board Certified Foot Surgeon, Discusses How to Tell if a Fracture is Healing
If you are experiencing foot or ankle pain, give us a call at 425-391-8666 or make an appointment onine today.
Dr. Brandon Nelson, A Board Certified Physician, Discusses Toe Pain And Plantar Plate Injuries
Toe pain, especially of the 2nd, 3rd and 4th toe can be quite common and have a few different sources of pain. The 2nd toe often has pain associated with a bunion or instability of the inside of the foot. A lot of patients have a foot structure that can overload the 2nd toe and cause mechanical pressures that eventually fatigue the joint. The 3rd and 4th toe are more likely to have an entrapped nerve. The anatomy in this location causes a compression issue where the nerve exists and can create problems for patients.
The 2nd toe or 2nd metatarsal phalangeal joint has a thickening called a plantar plate. This thickening acts like a cushion and helps protect the toe and joint when walking. If your foot structure places too much pressure on this joint, you can tear the plantar plate. One will often see the toe start to drift towards the 1st or inside of the foot. The pain is often like a neuroma, burning, tingling, and swelling. Often patients will require an MRI to confirm the tear. Once the tear is confirmed the plantar plate usually requires surgical repair. There are two methods one from the top of the toe and the other from the bottom. I often will decide which is appropriate for the patient based on any other foot pathology that may need to be addressed, like a bunion.
The 3rd and 4th MTPJ or 3rd interspace, the area between the 3rd and 4th toes is common spot for a Morton’s neuroma. The foot has two large nerves on the bottom the lateral and medial plantar nerves. These two nerves come together in the 3rd interspace and are often compressed between the metatarsal bones. This squeezing affect can result in burning to these two digits. A neuroma can be treated very effectively with alcohol injections. The alcohol injection series is 89% successful in eliminating nerve pain.
If you are suffering from burning, tingling, or swelling in your foot we can help. Give us a call at 425-391-8666 or make an appointment online.
How Nerve Damage Can Affect a Diabetic Patient’s Feet
Neuropathy, or nerve damage, is a condition many people with diabetes also suffer from. Heightened levels of sugar in the bloodstream due to diabetes can cause impaired nerve and blood vessel functionality. Peripheral neuropathy—the most common form of neuropathy in diabetics—affects the feet and legs. It can damage blood vessels’ ability to provide nutrients and oxygen to nerves in the feet and also reduce the signals those nerves send to the brain. Symptoms of peripheral neuropathy may include a burning sensation—or numbness, tingling, tightness or sharp pains—in the feet. Excessive sweating or a heaviness in the legs or arms may also occur. Diabetic patients may help reduce or prevent nerve damage by controlling blood sugar levels, reducing blood pressure, refraining from smoking or drinking alcohol, and losing weight. If you have diabetes, it is suggested that you contact a podiatrist to help manage the impact this disease can have on your feet.
Neuropathy
Neuropathy can be a potentially serious condition, especially if it is left undiagnosed. If you have any concerns that you may be experiencing nerve loss in your feet, consult with the podiatrists from Issaquah Foot & Ankle Specialists. Our doctors will assess your condition and provide you with quality foot and ankle treatment for neuropathy.
What Is Neuropathy?
Neuropathy is a condition that leads to damage to the nerves in the body. Peripheral neuropathy, or neuropathy that affects your peripheral nervous system, usually occurs in the feet. Neuropathy can be triggered by a number of different causes. Such causes include diabetes, infections, cancers, disorders, and toxic substances.
Symptoms of Neuropathy Include:
- Numbness
- Sensation loss
- Prickling and tingling sensations
- Throbbing, freezing, burning pains
- Muscle weakness
Those with diabetes are at serious risk due to being unable to feel an ulcer on their feet. Diabetics usually also suffer from poor blood circulation. This can lead to the wound not healing, infections occurring, and the limb may have to be amputated.
Treatment
To treat neuropathy in the foot, podiatrists will first diagnose the cause of the neuropathy. Figuring out the underlying cause of the neuropathy will allow the podiatrist to prescribe the best treatment, whether it be caused by diabetes, toxic substance exposure, infection, etc. If the nerve has not died, then it’s possible that sensation may be able to return to the foot.
Pain medication may be issued for pain. Electrical nerve stimulation can be used to stimulate nerves. If the neuropathy is caused from pressure on the nerves, then surgery may be necessary.
If you have any questions, please feel free to contact one of our offices located in Issaquah, WA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Neuropathy
Neuropathy is a condition in which the nerves in the body become damaged from a number of different illnesses. Nerves from any part of the body, including the foot, can be damaged. There are several forms of neuropathy including peripheral neuropathy, cranial neuropathy, focal neuropathy, and autonomic neuropathy. Furthermore there is also mononeuropathy and polyneuropathy. Mononeuropathies affect one nerve while polyneuropathies affect several nerves. Causes of neuropathy include physical injury, diseases, cancers, infections, diabetes, toxic substances, and disorders. It is peripheral neuropathy that affects the feet.
The symptoms of neuropathy vary greatly and can be minor such as numbness, sensation loss, prickling, and tingling sensations. More painful symptoms include throbbing, burning, freezing, and sharp pains. The most severe symptoms can be muscle weakness/paralysis, problems with coordination, and falling.
Podiatrists rely upon a full medical history and a neurological examination to diagnose peripheral neuropathy in the foot. More tests that may be used include nerve function tests to test nerve damage, blood tests to detect diabetes or vitamin deficiencies. Imaging tests, such as CT or MRI scans, might be used to look for abnormalities, and finally nerve or skin biopsies could also be taken.
Treatment depends upon the causes of neuropathy. If the neuropathy was caused by vitamin deficiency, diabetes, infection, or toxic substances, addressing those conditions can lead to the nerve healing and sensation returning to the area. However if the nerve has died, then sensation may never come back to the area. Pain medication may be prescribed for less serious symptoms. Topical creams may also be tried to bring back sensation. Electrical nerve stimulation may be used for a period of time to stimulate nerves. Physical therapy can strengthen muscle and improve movement. Finally surgery might be necessary if pressure on the nerve is causing the neuropathy.
If you are experiencing sensation loss, numbness, tingling, or burning sensations in your feet, you may be experiencing neuropathy. Be sure to talk to a podiatrist to be diagnosed right away.
Mid Foot Bone Spurs and Surgery Part Two
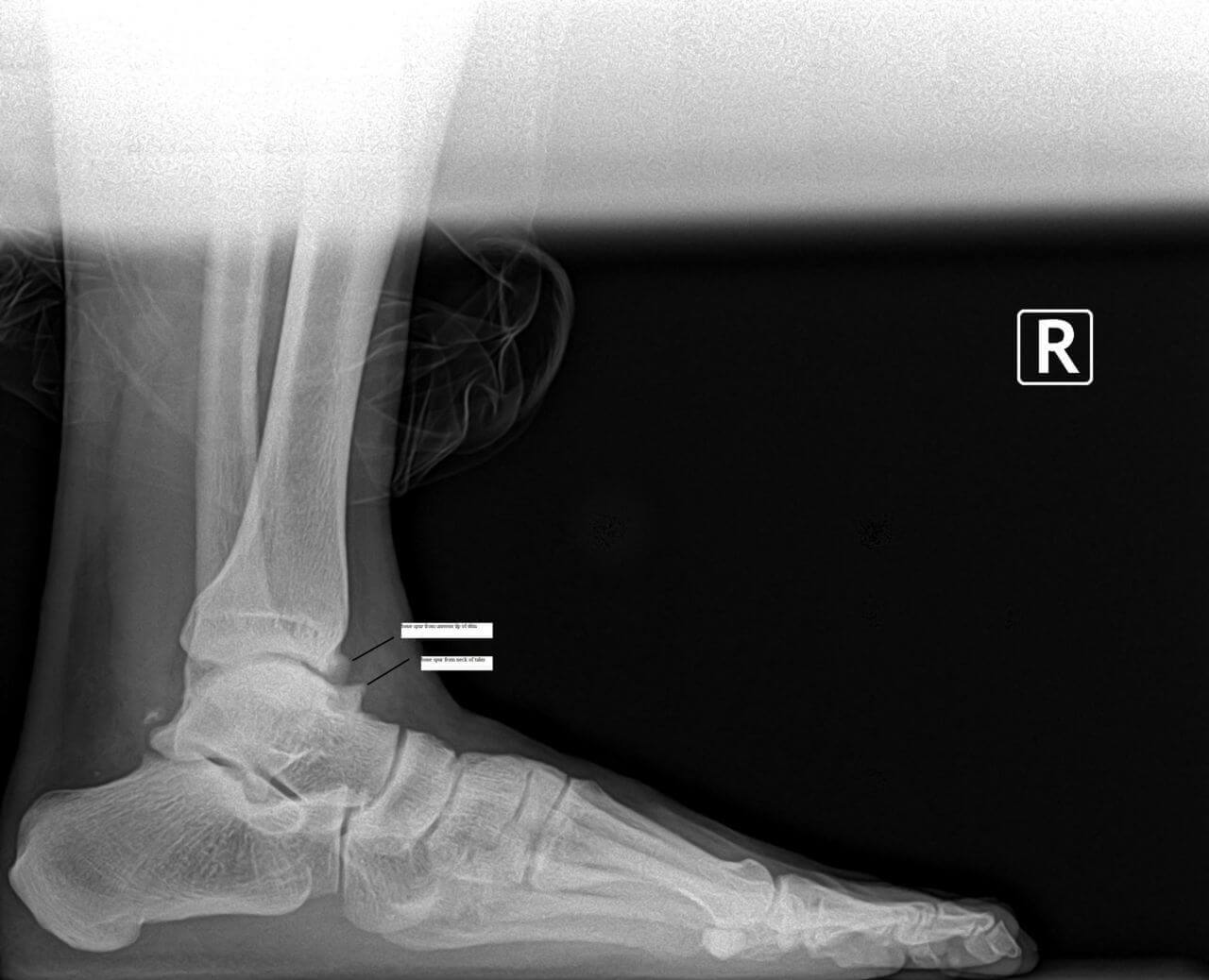
Mid foot bone spurs and surgery part two.
Surgery to treat a bony prominence in this area usually is very straightforward. It typically involves an incision directly adjacent to the prominence or bone spur. We surgically go down to the tissue layers and then expose the bony prominence. Then most commonly a power burr is used to smooth down the excessive bone in the area or sometimes a special surgical saw. The wound is cleaned up and flushed to remove any small bone fragments.
The remaining cut bony surface usually has an excellent blood supply and can cause swelling problems or even a small collection of blood like a hematoma. Therefore several different techniques can help deal with this. One is to use a small drain which allows for a path for the blood to escape the area, this is especially useful for the first several days postop. Another strategy is to use bone wax to seal the bone.
Some Surgeons use topical fibrin to help clot exposed bleeding vessels that are small and embedded in the bone. After the bone remodeling procedure is done, the soft tissue layers are closed and the procedure is then complete. Usually it’s a relatively quick recovery. Remember that we are talking about a bony prominence without significant underlying midfoot arthritis. The midfoot arthritis and surgical fusion of the involved joint can be a longer recovery.
If you have questions about spurs or bumps on the top of your feet forefoot surgery in general, and would like a consultation please let us know. Give us a call at 425-391-8666 or make an appointment online.
Dr. Brandon Nelson, A Board Certified Physician, Discusses Achilles Tendon Pain
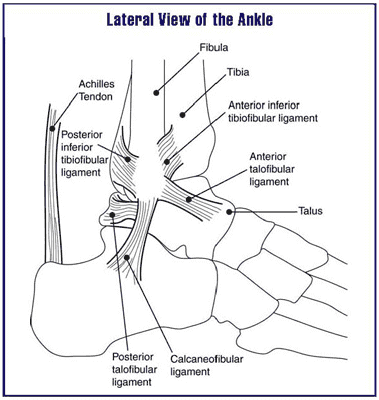
The Achilles tendon is the thickest and strongest tendon in the human body. It has more pounds per square inch applied to it than any other tendon. We consider it the work horse of the lower extremity. It is constantly in use and provides forward motion in the gait cycle. These reasons make it one of the most commonly injured or strained tendons.
Achilles tendonitis usually presents with pain and selling around the back of the ankle. Patients have usually increased activities or changed activities or even started to walk more. There is often pain when getting out of bed, that gets better as the day goes on, but returns with rest. Sometimes patients will describe weakness or a catching sensation.
Diagnosing Achilles Tendon injuries is relatively straight forward. A typical mechanical and musculoskeletal exam of the foot and ankle are performed. An ultrasound or x-ray can be helpful as well. More advanced cases can require an MRI to rule our tearing or degeneration.
Treatment is provided on a case-by-case basis. It is important to identify the cause and help eliminate or reduce this activity. Stretching is vital and reducing the mechanical burden. I always encourage people with Achilles issues to see a foot and ankle physician before implementing treatment as these measures are not always appropriate. If you are suffering from Achilles tendonitis, give us a call at 425-391-8666 or make an appointment online so we can get you back on the road to recovery.