heel pain
Displaying items by tag: heel pain
Dr Brandon Nelson, A Double Board-Certified Physician & Surgeon, Discusses Stubborn Heel Pain
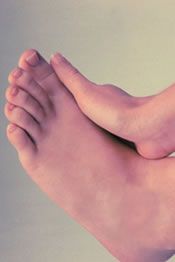
I have to say that exercise for me helps with my mental health and overall wellbeing. I typically workout 6/7 days a week and enjoy running, biking, rucking and walking the dog. It is a great stress relief and helps me clear my head after a day of work. I am sure many of you can relate and as the weather clears more of us are getting back into an exercise routine.
That being said, I always see a spike in heel pain patients this time of year. It makes sense with the weather drying up and everyone wanted to get outside and ready for summer. Heel pain can really sideline you as you return to activities. It can come on suddenly and stick around for months. As a side note, the earlier you get treatment the faster you can recover. It is usually caused by inflammation of your plantar fascia.
The plantar fascia is the main support network of the foot. It is a soft tissue structure that runs from your heel to your toes. It has the function of controlling the foot and helping with propulsion. It can get worn out with time or tired from increased loads. It is by far the most common condition I treat.
Some patients wait quite a while before coming in and these cases are often what I call “stubborn heel pain” or “chronic fasiitis”. This is because the inflammation has now become chronic, and the body has given up on trying to fix it and now coexists with this pathology. These cases are harder to treat and usually require more extensive care. I think it is important to understand that once it becomes chronic, part of the treatment usually requires a reactivation of the body’s ability to recognize this condition. You must take the chronic state of inflammation and turn it back to an acute state.
I really enjoy helping my patients get their life back and their feet pain free. If you would like a consultation for your heel pain I can help. Call to make an appointment with me at 425-391-8666 or make an appointment online.
Sincerely,
American College of Foot & Ankle Surgeons
Issaquah’s Top Podiatrist
Dr. Brandon Nelson, A Board Certified Foot Physician & Surgeon, Issaquah’s Top Podiatrist, Discusses the Best Bunion Procedure to Have
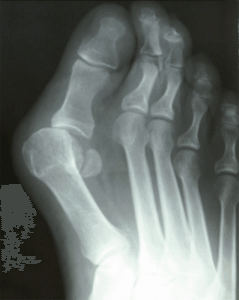
I have been practicing medicine now for about 15 years and like to look back from time to time on how it has changed. Currently there is a lot of talk about the Lapiplasty bunion and bunion surgery in general. I thought I would take a few minutes and discuss this topic.
Bunion surgery continues to be one of the most common foot surgeries in the United States if not the most common. I believe the last statistic I read was something like almost 350,000 operations per year. It is hard to believe there are that many bunions out there!
The most utilized bunion surgery is the Austin bunionectomy. This is for a couple reasons. One can correct the vast majority of bunions whether small or large. It has a much faster recovery and is technically not as challenging as other operations. It involves the cutting of the metatarsal head in a chevron pattern and shifting that bone medially. It is usually fixated in place with a few screws. Patients can bear weight immediately and are typically in a walking boot for 4-8 weeks. It has good long term results and will probably continue to be the most common bunionectomy for that reason.
The other most talked about bunion procedure is the Lapidus bunionectomy or the Lapiplasty. This procedure is the choice for very large bunions or juvenile bunions. It is technically more challenging but provides for excellent correction. This involves fusion of the metatarsal cuneiform joint to realign the metatarsal. It usually involves a period of non weight bearing from 3-8 weeks. The long term results are excellent.
That begs the question: which procedure is best for bunion patients? Well the answer is not simple. It really involves a couple key considerations. First being how does the rest of the foot look and how much motion do we have through the 1st metatarsal? Second is patient age and activity level. Third would be overall general health of the patient and bone quality. I recommend seeing a surgeon that performs a lot of bunion surgeries as their outcomes will be better.
If you have a bunion and would like to know your options and have it evaluated schedule, make an appointment with me and I will help you.
Sincerely,
Board Certified Physician & Surgeon
Issaquah’s Top Podiatrist & Foot/Ankle Surgeon
Dr Brandon Nelson, A Board Certified Physician & Surgeon, Issaquah’s Best Podiatrist, Discusses Heel Pain

Heel pain can affect people of all ages, lifestyles and activity levels. You can be an avid exerciser, a home body or just spend all day working on your feet. I will discuss some of the causes of heel pain, the symptoms and when to seek medical attention. I have been a practicing podiatrist in Issaquah for over 25 years and have treated and helped 1000’s of patients.
There are many common causes of heel pain. However a few are the most common and these include; plantar fasciitis, Achilles tendonitis, stress fractures and Baxter’s neuritis.
Plantar fasciitis is caused from an inflammation of a band of tissue running on the bottom of the foot. The job of the fascia is to support the arch of the foot and control 3 dimensional movement. It often occurs with repetitive stress like standing all day or running.
Achilles tendonitis is usually located more towards the back of the heel. The Achilles tendon helps to push off the foot during the gait cycle. Often any activity that increases load like jumping rope can cause the Achilles to become inflamed. People often feel swelling or a thickening of this tendon in the ankle.
Stress fractures are usually related to overtraining and time. They occur with repetitive loading of a bone. The bone I am speaking of in this case is the calcaneus. These can be tricky to diagnose.
Baxter’s neuritis is rare but is often confused for plantar fasciitis. There is usually more of a burning or tingling that occurs. Often there is not an increase in activities and no correlation with time spent on your feet and pain.
I recommend seeking early treatment for heel pain. I see that patients that wait longer have a harder time recovering and often need more therapeutic interventions. This is especially true for athletes, get in early and get a head of the pathology.
If you have heel pain and would like an appointment with Issaquah’s top Podiatrist at 425-391-8666 or make an appointment online.
Sincerely,
Board Certified Foot & Ankle Surgeon
Dr Brandon Nelson, A Board-Certified Physician & Surgeon Discusses Plantar Fasciitis

Plantar fasciitis or heel pain is the most common cause to seek help from a foot and ankle physician. There are many causes of heel pain but by far the most common is plantar fasciitis. So, let’s discuss first what the plantar fascia is, second why it occur and lastly how to fix it.
What is your plantar fascia? The plantar fascia is located on the bottom of your foot. It runs the entire length of your foot from your heel to your toes. It starts with an attachment at the calcaneus, your heel bone, and runs to your metatarsal head, where your toes start. It is a thick dense fascial type of tissue. Its main function is to support your arch. It also helps flex your toes and provides stability to your foot with ambulation.
Why does plantar fasciitis happen? There are many schools of thought on this one but let’s talk about a few of the most common. The first and probably most accepted theory is overuse. The fascia never gets a chance to rest, it is the workhorse of the foot. Every step you take it is activated and over time this can fatigue the structure. Secondly foot genetics can play a role in it as well. People with a flatfoot tend to need more arch support and this can put pressure on the plantar fascia. Lastly there is a thought that tight calf muscles can pull on the fascia making it irritated. I think all of these can have merit in certain circumstances and I often see multiple etiologies.
Lastly, how do we treat plantar fasciitis? This is a more complex question. I think this one is very hard to answer as every case can be different. I think a careful history and physical is essential for proper treatment. I also find length of time and activity level to be important. But a couple general things can help like calf stretching and activity medication can be essential.
If you would like a consultation on your heel pain, I can help. Call to make an appointment with me at 425-391-8666 or schedule an appointment online today.
Sincerely,
American College of Foot & Ankle Surgeons
Dr Brandon Nelson, A Board Certified Physician and Surgeon, Discussed When Your Heel Pain Will Not Go Away and You Need A Second Opinion

Heel pain can be difficult for patients and physicians alike. It can provide a challenge for all parties involved. I have seen hundreds or maybe even thousands of second opinions for heel pain. Over the years I have learned many valuable lessons that can be extremely beneficial to treating heel pain.
One of the first lessons I learned was to listen to the patient. Often patients provide great clues to the cause and origin of heel pain. The history and story a patient tells often paints the perfect picture for how the pain is continuing to cause discomfort. Not all heel pain is the same and although plantar fasciitis is the number one cause remain open to other sources. This leads me to lesson number two.
Lesson number two not all heel pain is plantar fasciitis. I have seen so many other causes and as a provider we need to be diligent. The back can be a source of chronic heel pain. Patients with back issues can have manifestations in the feet. Another common cause is nerve pain. Over the years I would say this is the most common reason heel pain does not get better. The clinician is missing a nerve entrapment. This is not all of the other reasons for heel pain but a few examples to illustrate the importance of recognizing there are other sources of heel pain.
Lesson three is to understand not all heel pain can be treated the same. I have seen patients over the years that have similar heel pain but similar treatments do no work. This is why it is important to treat all patients as individuals. To make sure to look at foot structure, gait cycles and daily routines to see how each individual can be treated for the best possible outcome.
If you have heel pain and are in need of a second opinion or are just fed up with daily pain make an appointment with me today I can help. Give us a call at 425-391-8666 or make an appointment online.
Sincerely,
Dr Brandon Nelson, A Board-Certified Physician & Surgeon Discusses Burning Pain in Your Heel
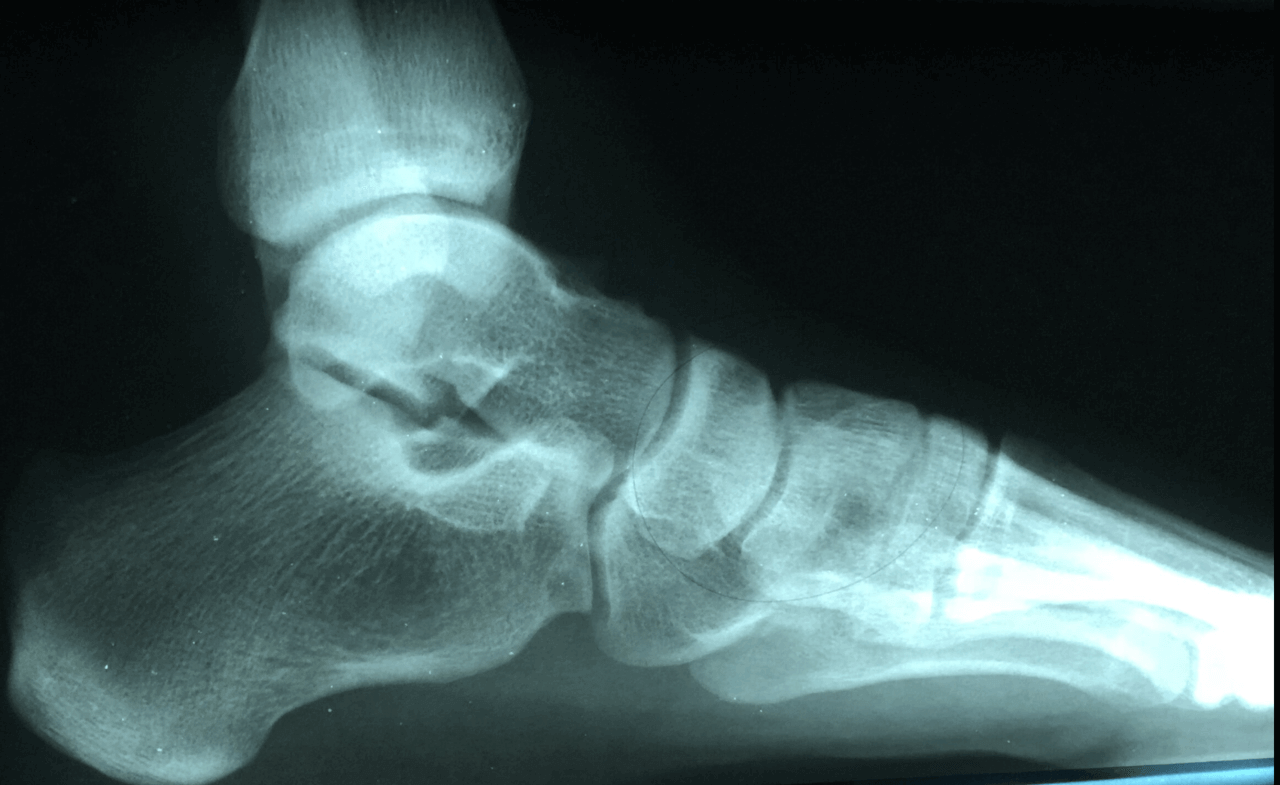
Have you experienced burning in your heel? Does your heel feel like it is on fire? Are you getting pins and needles in your heels? This could be a condition called Baxter’s neuritis or an entrapped nerve in your foot. This can often be confused with plantar fasciitis and the two can be difficult to distinguish.
I saw a few patients this last week that had Baxter’s neuritis and it made me want to write a few words about it. This condition was brought to popularity by Dr Baxter and prior to that this pathology was often thought of as plantar fasciitis. It should be noted that many patients I see have both conditions present. The most notable difference seems to be the burning pain and radiating nerve pain that can be reproduced by tapping the nerve. However, a nerve study can be helpful to confirm the diagnosis and help with planning treatment.
There are a few conservative measures that can provide pain relief. Orthotics, injections, and some medications prove to be successful. However, some patients do not find any improvement and surgical decompression of the nerve is done at that point. The constricting structures around the nerve are freed up and the pain typically resolves. I always recommend trying conservative measures first before considering surgical intervention.
If you have burning heel pain I can help, call to make an appointment with me at 425-391-8666 or schedule an appointment online.
carpet cleaning seattle
Sincerely,
American College of Foot & Ankle Surgeons
Plantar Fasciitis Treatment Success with Shockwave Therapy

Plantar Fasciitis Treatment Success with Shockwave Therapy
Introduction
Plantar fasciitis is a common and often debilitating condition characterized by heel pain, especially in the morning or after prolonged periods of standing or walking. It occurs when the plantar fascia, a thick band of tissue that runs along the bottom of the foot, becomes inflamed or damaged. While there are several treatment options available, one that has gained increasing attention for its success is shockwave therapy. In this blog, we'll explore plantar fasciitis and delve into how shockwave therapy has emerged as a highly effective treatment option, offering hope and relief to those individuals suffering from this condition.
Understanding Plantar Fasciitis
Before reviewing shockwave therapy, it's essential to understand what plantar fasciitis is and why it can be so challenging to treat. The plantar fascia is a crucial component of the foot's structure, acting as a shock absorber and supporting the arch of the foot. When this tissue becomes damaged or inflamed, it can lead to persistent heel pain and reduced mobility.
Common Causes of Plantar Fasciitis:
Overuse or repetitive strain on the plantar fascia, often due to activities like running or standing for extended periods.
Obesity, as excess weight puts extra stress on the feet.
Improper footwear with inadequate arch support.
Tight calf muscles or Achilles tendon.
Traditional Treatment Approaches
Plantar fasciitis treatment typically begins with conservative methods, including:
Rest: Reducing activity levels to allow the plantar fascia to heal.
Ice: Applying ice to the affected area to reduce inflammation.
Stretching exercises: Focusing on calf stretches to improve flexibility.
Orthotics: Custom shoe inserts to provide arch and biomechanical support.
Non-steroidal anti-inflammatory drugs (NSAIDs): Medications to manage pain and inflammation.
While these methods can be effective for some individuals, others find themselves facing chronic, persistent pain that doesn't respond well to these treatments. This is where shockwave therapy comes into play.
Shockwave Therapy for Plantar Fasciitis
Shockwave therapy, also known as extracorporeal shockwave therapy (ESWT), is a non-invasive procedure that has shown remarkable success in treating plantar fasciitis when other treatments have failed. Here's how it works:
Application of Shockwaves: During the procedure, high-energy shockwaves are directed at the affected area. These shockwaves create microtrauma within the damaged tissue, stimulating the body's natural healing response.
Pain Reduction and Healing: Shockwave therapy has been shown to reduce pain by disrupting pain signals and improving blood flow to the damaged tissue. This, in turn, promotes tissue regeneration and healing.
Quick Procedure with Minimal Downtime: Shockwave therapy sessions typically last 15-20 minutes, and most patients can resume their regular activities shortly afterward. Five weekly sessions typically offer optimal results.
Success with Shockwave Therapy
The success of shockwave therapy in treating plantar fasciitis is supported by numerous patient testimonials and clinical studies. Here are a few reasons why it has gained popularity:
High Success Rate: Many patients experience significant pain reduction and improved mobility after undergoing shockwave therapy.
Non-Surgical: Shockwave therapy is non-invasive, eliminating the need for surgery and its associated risks and recovery time.
Long-Lasting Relief: For many, the benefits of shockwave therapy are long-lasting, providing relief from chronic pain.
Improved Quality of Life: Patients who have struggled with plantar fasciitis for years often find that shockwave therapy finally allows them to regain their quality of life and return to their favorite activities.
Available treatment: We have been proving this treatment at our clinic with high success for over 8 years
Conclusion
Plantar fasciitis can be a stubborn and painful condition, but there is hope for those who have tried various treatments without success. Shockwave therapy has emerged as an effective and non-invasive option, offering relief and improved quality of life for individuals suffering from this condition. If you're struggling with plantar fasciitis, please contact our clinic at 425-391-8666 or make an appointment online.
Dr Brandon Nelson, A Board-Certified Physician & Surgeon Discusses Heel Pain That Will Not Get Better

I have had heel pain in the past, specifically plantar fasciitis and it really was challenging to go about your day. My pain when I got out of bed was uncomfortable until it loosened up but if I sat down for any period of time it came right back. Does this sound familiar? If it does and this pain just will not go away, I can help.
Plantar fasciitis is by far the leading cause of heel pain. The plantar fascia is a tough soft tissue structure that provides the most structural support to your foot. It works to prevent your foot from flattening out and helps control your foot for the gait cycle. It is vital for foot function and is under chronic tension. These factors make it one of the most common causes of foot pain.
Treating plantar fasciitis can often be difficult as well. There are many people that have seen a physician and still have been or have been working on their pain at home. I encourage you if this is you to see a physician that specializes in heel pain. I have been working with heel pain patients for over 15 years. I have seen every type of pain and can help cure even the most stubborn cases. If you want to get your life back and live without heel pain I can help, call to make an appointment with me at 425-391-8666.
Sincerely,
American College of Foot & Ankle Surgeons
Dr Brandon Nelson, A Board-Certified Physician & Surgeon Discusses Why Your Heel Pain Will Not Go Away
Heel pain is always a challenge to deal with as a patient. It can be very tiring on one’s nerves. It is hard to wake up in pain and go to sleep in pain. Especially if you have first step pain, that pain when you put your foot on the ground when getting and it makes you just want to just crawl back into bed. Plantar fasciitis is challenging and can take time and effort to get rid of it. The good news is that I can help. I have seen 1000s of patients with heel pain. I can help whether you have had it for a week or for a year.
It is important to understand the cause of the pain. Is it the fascia, is it the Achilles tendon or is it a pinched nerve. Regardless of the reason, a thorough workup is paramount to helping fix the underlying cause. At the very least an x-ray is useful and the first place to start. New types of shoe gear and changes in training can be informative as well. Additionally, what does the pain feel like, what have you tried so far and how long has it been present. These are all great things to share with your provider and helpful in coming up with a treatment plan.
If you have heel pain and it is not getting better I can help. Make an appointment online or call us today at 425-391-8666.
Sincerely,
Dr Brandon Nelson, A Board Certified Physician & Surgeon, Discusses Chronic Heel Pain and How to Get Rid of It

The number one cause of heel pain is Plantar Fasciitis. Plantar Fasciitis is an inflammation of a band of tissue on the bottom of one’s foot. The most common reason is overuse. Overuse can come in many forms, people that work on their feet, or avid exercisers and even just long term wear and tear on your feet. It is important to know that your fascia is the main supporting network of one’s feet and is under chronic mechanical load.
It is important in the process of trying to cure plantar fasciitis to identify any outlying reasons for fasciitis. These outliers can be systemic causes, training errors or general overuse injuries. I think an x-ray is always warranted as well as an overall skeletal exam. The earlier one sees a foot and ankle physician the faster we can get you on the road to recovery.
Once an exam has been performed the next stop is how do we fix the underlying causes and cure the fascia long term. There are many options you can read about but the mainstay is reducing mechanical burdens and inflammation. I have a protocol I have used for more than 10 years and on 1000’s of patients. The majority of my patients are 50-70% better within the first week of seeing me.
Then there are the patients that have chronic fasciitis or long term fasciitis. The workup for these patients should be a little different and more extensive. Once plantar fasciitis has been identified as the root problem more advanced modalities will usually cure the fasciitis. The focus of these modalities is usually to stimulate one’s own biology to actively heal the underlying inflammation. These are some of the most cutting edge techniques and technologies available and our office has the 2 most effective modalities to fix your heel pain.
If you have heel pain, schedule an appointment with me, Dr. Nelson and I will get you fixed and ready to enjoy your summer! Give us a call at 425-391-8666 or make an appointment online.
Voted by Holistic Magazine as a top holistic provider.
Sincerely,
Board Certified Physician & Surgeon


