September 2023
Dr Timothy Young reviews Shockwave Therapy: The Ultimate Solution for Stubborn Plantar Fasciitis
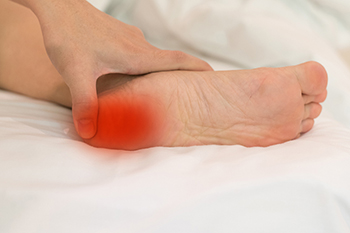
Dr Timothy Young reviews Shockwave Therapy: The Ultimate Solution for Stubborn Plantar Fasciitis
Introduction
Plantar fasciitis is a painful and persistent condition that can severely impact one's quality of life. Characterized by intense heel pain, especially during the first steps in the morning or after prolonged periods of rest, it's a condition that affects millions of people worldwide. While there are various treatment options available, shockwave therapy has emerged as a leading choice for those struggling with stubborn plantar fasciitis. In this blog, we'll explore why shockwave therapy is often considered the best treatment for this challenging ailment.
Understanding the Frustration of Stubborn Plantar Fasciitis
Plantar fasciitis occurs when the plantar fascia, a thick band of tissue that runs along the bottom of the foot, becomes inflamed or damaged. This condition can be particularly frustrating because it often resists traditional treatments, such as rest, ice, and stretching exercises. When conservative measures fail to provide relief, individuals may face ongoing pain, reduced mobility, and decreased quality of life.
Why is Shockwave Therapy the Best Option for Stubborn Plantar Fasciitis?
Non-Invasive and Minimally Disruptive: Unlike surgical options, shockwave therapy is a non-invasive procedure. Patients can undergo treatment without the need for incisions, anesthesia, or a lengthy recovery period. This makes it an attractive option for those looking to avoid the risks and downtime associated with surgery.
High Success Rates: Numerous studies and clinical trials have demonstrated the effectiveness of shockwave therapy for stubborn plantar fasciitis. Many patients experience significant pain reduction and improved function after a series of shockwave sessions.
Stimulates Natural Healing: Shockwave therapy works by delivering high-energy shockwaves to the affected area. These shockwaves create microtrauma within the damaged tissue, stimulating the body's natural healing response. This process promotes tissue regeneration and reduces inflammation.
Quick and Convenient: A typical shockwave therapy session lasts only 15-20 minutes, and most patients can resume their daily activities immediately afterward. The procedure is typically performed in an outpatient setting, making it a convenient option for those with busy schedules.
Addresses the Root Cause: Unlike some treatments that merely mask the pain, shockwave therapy targets the root cause of plantar fasciitis. By promoting healing and reducing inflammation, it offers long-term relief rather than just temporary pain management.
Minimal Side Effects: The side effects of shockwave therapy are generally mild and short-lived. Some patients may experience temporary soreness or bruising at the treatment site, but these effects are typically minor compared to the potential benefits.
Reduced Reliance on Medications: Shockwave therapy can often reduce the need for pain medications, which can have side effects and long-term risks. This is particularly important for individuals seeking to avoid the potential downsides of pharmaceutical interventions.
Conclusion
Stubborn plantar fasciitis can be an incredibly frustrating and painful condition, but there is hope. Shockwave therapy has emerged as a highly effective and non-invasive treatment option, offering relief and improved quality of life for those who have struggled for far too long. If you've been dealing with the relentless discomfort of plantar fasciitis, consult with a healthcare professional to discuss whether shockwave therapy is a suitable treatment for you. While no treatment is guaranteed to work for everyone, shockwave therapy has proven to be a game-changer for many individuals, providing the opportunity to regain their mobility and enjoy life without the constant burden of pain. Please contact our clinic to see if this treatment is right for you. Give us a call at 425-391-8666 or make an appointment online.
Plantar Fasciitis Treatment Success with Shockwave Therapy

Plantar Fasciitis Treatment Success with Shockwave Therapy
Introduction
Plantar fasciitis is a common and often debilitating condition characterized by heel pain, especially in the morning or after prolonged periods of standing or walking. It occurs when the plantar fascia, a thick band of tissue that runs along the bottom of the foot, becomes inflamed or damaged. While there are several treatment options available, one that has gained increasing attention for its success is shockwave therapy. In this blog, we'll explore plantar fasciitis and delve into how shockwave therapy has emerged as a highly effective treatment option, offering hope and relief to those individuals suffering from this condition.
Understanding Plantar Fasciitis
Before reviewing shockwave therapy, it's essential to understand what plantar fasciitis is and why it can be so challenging to treat. The plantar fascia is a crucial component of the foot's structure, acting as a shock absorber and supporting the arch of the foot. When this tissue becomes damaged or inflamed, it can lead to persistent heel pain and reduced mobility.
Common Causes of Plantar Fasciitis:
Overuse or repetitive strain on the plantar fascia, often due to activities like running or standing for extended periods.
Obesity, as excess weight puts extra stress on the feet.
Improper footwear with inadequate arch support.
Tight calf muscles or Achilles tendon.
Traditional Treatment Approaches
Plantar fasciitis treatment typically begins with conservative methods, including:
Rest: Reducing activity levels to allow the plantar fascia to heal.
Ice: Applying ice to the affected area to reduce inflammation.
Stretching exercises: Focusing on calf stretches to improve flexibility.
Orthotics: Custom shoe inserts to provide arch and biomechanical support.
Non-steroidal anti-inflammatory drugs (NSAIDs): Medications to manage pain and inflammation.
While these methods can be effective for some individuals, others find themselves facing chronic, persistent pain that doesn't respond well to these treatments. This is where shockwave therapy comes into play.
Shockwave Therapy for Plantar Fasciitis
Shockwave therapy, also known as extracorporeal shockwave therapy (ESWT), is a non-invasive procedure that has shown remarkable success in treating plantar fasciitis when other treatments have failed. Here's how it works:
Application of Shockwaves: During the procedure, high-energy shockwaves are directed at the affected area. These shockwaves create microtrauma within the damaged tissue, stimulating the body's natural healing response.
Pain Reduction and Healing: Shockwave therapy has been shown to reduce pain by disrupting pain signals and improving blood flow to the damaged tissue. This, in turn, promotes tissue regeneration and healing.
Quick Procedure with Minimal Downtime: Shockwave therapy sessions typically last 15-20 minutes, and most patients can resume their regular activities shortly afterward. Five weekly sessions typically offer optimal results.
Success with Shockwave Therapy
The success of shockwave therapy in treating plantar fasciitis is supported by numerous patient testimonials and clinical studies. Here are a few reasons why it has gained popularity:
High Success Rate: Many patients experience significant pain reduction and improved mobility after undergoing shockwave therapy.
Non-Surgical: Shockwave therapy is non-invasive, eliminating the need for surgery and its associated risks and recovery time.
Long-Lasting Relief: For many, the benefits of shockwave therapy are long-lasting, providing relief from chronic pain.
Improved Quality of Life: Patients who have struggled with plantar fasciitis for years often find that shockwave therapy finally allows them to regain their quality of life and return to their favorite activities.
Available treatment: We have been proving this treatment at our clinic with high success for over 8 years
Conclusion
Plantar fasciitis can be a stubborn and painful condition, but there is hope for those who have tried various treatments without success. Shockwave therapy has emerged as an effective and non-invasive option, offering relief and improved quality of life for individuals suffering from this condition. If you're struggling with plantar fasciitis, please contact our clinic at 425-391-8666 or make an appointment online.
Symptoms and Effective Treatment for Sever’s Disease
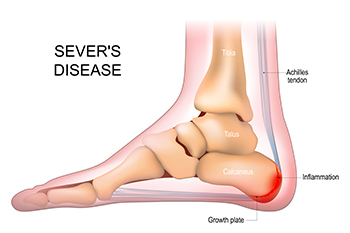
Sever's disease, also known as calcaneal apophysitis, is a common but often misunderstood condition affecting children and adolescents, especially those active in sports. It is not a traditional disease but rather a painful growth plate disorder. Understanding its symptoms and appropriate treatment is vital for parents and young athletes. The hallmark symptom of Sever's disease is heel pain, typically at the back or along the bottom of the heel. Pain tends to worsen during or after physical activities and may cause limping or discomfort when walking or running. The condition arises when the growth plate at the back of the heel bone becomes inflamed due to repetitive stress. Fortunately, Sever's disease is treatable. Getting adequate rest and taking over-the-counter pain relievers can help alleviate discomfort. Stretching exercises and may also be recommended to improve flexibility, and strengthen the calf muscles. Wearing supportive footwear with cushioned insoles may help reduce heel pressure. By recognizing the symptoms and seeking appropriate treatment, parents and young athletes can manage Sever's disease effectively, allowing for a smoother path to recovery and a return to their favorite activities. If your active child has heel pain, it is strongly suggested that you consult a podiatrist who can accurately diagnose and treat Sever’s disease.
Sever's disease often occurs in children and teens. If your child is experiencing foot or ankle pain, see the podiatrists from Issaquah Foot & Ankle Specialists. Our doctors can treat your child’s foot and ankle needs.
Sever’s Disease
Sever’s disease is also known as calcaneal apophysitis, which is a medical condition that causes heel pain I none or both feet. The disease is known to affect children between the ages of 8 and 14.
Sever’s disease occurs when part of the child’s heel known as the growth plate (calcaneal epiphysis) is attached to the Achilles tendon. This area can suffer injury when the muscles and tendons of the growing foot do not keep pace with bone growth. Therefore, the constant pain which one experiences at the back of the heel will make the child unable to put any weight on the heel. The child is then forced to walk on their toes.
Symptoms
Acute pain – Pain associated with Sever’s disease is usually felt in the heel when the child engages in physical activity such as walking, jumping and or running.
Highly active – Children who are very active are among the most susceptible in experiencing Sever’s disease, because of the stress and tension placed on their feet.
If you have any questions, please feel free to contact one of our offices located in Issaquah, WA . We offer the newest diagnostic and treatment technologies for all your foot and ankle injuries.
Sever's Disease
Sever’s disease, also known as calcaneal apophysitis is a common bone disorder that occurs during childhood. The disease is defined as an inflammation of the growth plate in the heel. When a child has a growth spurt, his heel bone grows faster than the muscles, tendons, and ligaments in his leg. This disease is a result of overuse. The people who are most likely to be affected by this disease are children who are in a growth spurt, especially boys who are from the ages of 5 to 13 years old. 60% of children with Sever’s disease have both heels involved.
Symptoms of this disease are heel pain that intensifies during running and jumping activities. The pain is typically localized to the posterior part of the heel. Symptoms may be severe, and they can easily interfere with daily activities. Children who play soccer, baseball, and basketball are more likely to develop Sever’s disease.
Your doctor will diagnose your child based on his or her symptoms, x-rays are generally not helpful in diagnosing this disease. Your doctor may examine both heels and ask your child questions about his or her activity level in sports. Your doctor may then use the squeeze test on your child’s heel to see if there is any pain. Nevertheless, some doctors might still use x-rays to rule out any other issues such as fractures, infections, and tumors.
Sever’s disease can be prevented by maintaining good flexibility while your child is growing. Another prevention method is to wear good-quality shoes that have firm support and a shock-absorbent sole. Sever’s disease can be treated by ceasing any activity that causes heel pain. You should apply ice to the injured heel for 20 minutes 3 times a day. Additionally, orthotics should be used for children who have high arches, flat feet, or bowed legs.
If you suspect your child has Sever’s disease, you should make an appointment with your podiatrist to have his or her foot examined. Your doctor may recommend nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen or naproxen to relieve pain. In more severe cases, your child may need a cast to rest his or her heel. Fortunately, Sever’s disease does not cause long-term foot problems. After treatment, your child should start to feel better within two weeks to two months.
Dr Brandon Nelson, A Board-Certified Physician & Surgeon Discusses Bunion Surgery/Best Long-Term Outcomes
Bunion surgery has been around for over 100 years. Historically, there were about 120 different types of bunion surgeries that could be performed. This has changed over the years as long-term data became available and we could see different outcomes with different procedures. This has shaped bunion surgery and now there are only about 4 commonly used procedures in the United States with 2 of the 4 being the most popular.
The first one is called an Austin bunionectomy. This procedure is executed at the head of the 1st metatarsal. It involved cutting the bone and realigning the joint. It is usually secured with 1 or 2 screws. Most patients can walk on this in a boot following surgery. The average time to heal is typically 4-8 weeks. This procedure is primarily reserved for smaller bunions. It is the most popular bunion procedure done to date.
However, some of us surgeons that do a lot of bunion surgery have been utilizing a procedure called the Lapidus bunionectomy. It is a little more technically challenging but has better long-term outcomes. This type of bunion correction holds up the best and is best for people with large bunions or young children. Recently Treace Medical has come out with a system to make the Lapidus easier and more reproducible for surgeons. This system is called Lapiplasty. I have found it can be helpful and is getting a lot of traction in health care currently.
If you have bunion pain I can help, call to make an appointment with me at 425-391-8666 or fill out a contact form online.
Sincerely,
American College of Foot & Ankle Surgeons
Dr Brandon Nelson, A Board-Certified Physician & Surgeon Discusses Bunion Pain
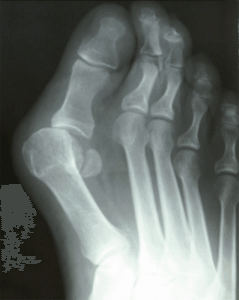
Bunions are a common presentation in my office. I see at least one new bunion patient a day. It is a common condition that can produce pain daily. We know that many bunions are inherited and get larger with time. They usually become painful as time goes on and the bunion spreads affecting the forefoot making activities uncomfortable.
Bunions are a separation of the first metatarsal from the second metatarsal. The first metatarsal begins to shift away from the other metatarsals or towards the other foot. When this occurs the big toe then begins to deviate in a direction away from the arch or towards the second toe. This is when things begin to change rapidly. If the first toe now slides under the second a crossover toe formation begins and the bunion changes in size rapidly. This is when most people present to my office and need help with the pain.
There are some conservative measures that are helpful for bunions including wider shoes and not going barefoot. It is important to note that no conservative measures will change the size of the bunion. I see all sorts of online appliances come into the office. These include splints, strapping devices and other items that state they will fix a bunion. But remember a bunion is from a bone moving out of alignment and this is impossible to correct on the outside of the foot.
If you have bunion pain I can help, call to make an appointment with me at 425-391-8666 or fill out a form online.
Sincerely,
American College of Foot & Ankle Surgeons
Psychological Effects of Toenail Fungus
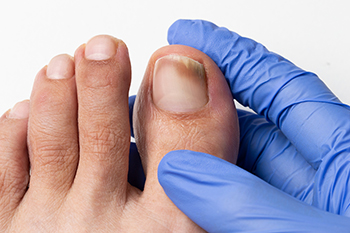
Onychomycosis, commonly known as toenail fungus, is the most prevalent nail disorder, with a growing incidence, particularly among the elderly. This condition is notorious for its stubbornness, requiring prolonged and often ineffective treatments, with frequent recurrences. Beyond affecting the nail's normal function, fungal nail infections can bring pain, an unsightly appearance, disruption of daily life, and negative psycho-social consequences. Patients often grapple with embarrassment, diminished self-esteem, and social withdrawal due to toenail fungus. Recent advances in treatment have emerged, offering more effective solutions. If you suffer from toenail fungus, it is suggested that you make an appointment with a podiatrist to discuss the physical and psychological effects of this condition. Honesty with this medical professional about how much it impacts your life is important in obtaining a more holistic approach to treatment.
For more information about treatment, contact the podiatrists of Issaquah Foot & Ankle Specialists. Our doctors can provide the care you need to keep you pain-free and on your feet.
Toenail Fungus Treatment
Toenail fungus is a condition that affects many people and can be especially hard to get rid of. Fortunately, there are several methods to go about treating and avoiding it.
Antifungals & Deterrence
Oral antifungal medicine has been shown to be effective in many cases. It is important to consult with a podiatrist to determine the proper regiment for you, or potentially explore other options.
Applying foot powder on the feet and shoes helps keep the feet free of moisture and sweat.
Sandals or open toed shoes – Wearing these will allow air movement and help keep feet dry. They also expose your feet to light, which fungus cannot tolerate. Socks with moisture wicking material also help as well.
If you have any questions please contact one of our offices located in Issaquah, WA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Treating Toenail Fungus
Fungal infection of the toenail, or onychomycosis, typically appears as a gradual change in a toenail’s texture and color that involves brittleness and darkening. The fungal infection itself occurs beneath the surface of the nail. Aside from discoloration, other symptoms include the collection of debris beneath the nail plate, white marks on the nail plate, and a foul odor emanating from the nail. If ignored, the infection can spread into other nails and the skin; in severe cases, it can hinder one’s ability to work or walk.
The toenails are particularly vulnerable to contracting infection in moist environments where people are likely to be walking barefoot, such as around swimming pools, public showers, and locker rooms. Fungal infection may also be more likely to occur in nail beds that have been injured, and sufferers of chronic diseases such as diabetes, circulatory problems, or immunodeficiency conditions are particularly prone to developing fungal nails.
Fungal nails can be primarily prevented by practicing proper hygiene and regularly examining the feet and toes. Carefully washing the feet with soap and water and thoroughly drying the feet afterwards are essential. Other tips include wearing shower shoes in public areas, changing shoes and socks daily, keeping toenails clipped at a short length, wearing breathable shoes that fit properly, wearing moisture-wicking socks, and disinfecting home pedicure tools and instruments used to cut nails.
Fungal nail treatment may vary between patients and the severity of the condition. Your podiatrist may suggest a daily routine of cleansing that spans over a period of time to ease mild infections. Over-the-counter or prescription antifungal agents may also be prescribed, including topical and/or oral medications. Debridement, or the removal of diseased nail matter and debris, may also be performed. In more severe cases, surgical treatment may be needed. In some instances, the temporary removal of the fungal nail allows for the direct application of a topical antifungal to the nail bed. In other cases, a chronically painful fungal nail that has not responded to other treatments may be permanently removed; this allows the infection to be cured and avoids the growth of a deformed nail.
Dr Brandon Nelson, A Board-Certified Physician & Surgeon Discusses Heel Pain That Will Not Get Better

I have had heel pain in the past, specifically plantar fasciitis and it really was challenging to go about your day. My pain when I got out of bed was uncomfortable until it loosened up but if I sat down for any period of time it came right back. Does this sound familiar? If it does and this pain just will not go away, I can help.
Plantar fasciitis is by far the leading cause of heel pain. The plantar fascia is a tough soft tissue structure that provides the most structural support to your foot. It works to prevent your foot from flattening out and helps control your foot for the gait cycle. It is vital for foot function and is under chronic tension. These factors make it one of the most common causes of foot pain.
Treating plantar fasciitis can often be difficult as well. There are many people that have seen a physician and still have been or have been working on their pain at home. I encourage you if this is you to see a physician that specializes in heel pain. I have been working with heel pain patients for over 15 years. I have seen every type of pain and can help cure even the most stubborn cases. If you want to get your life back and live without heel pain I can help, call to make an appointment with me at 425-391-8666.
Sincerely,
American College of Foot & Ankle Surgeons
Dr Brandon Nelson, A Board-Certified Physician & Surgeon Discusses Why You Should Have the Lapiplasty Procedure to Fix Your Bunion

Bunion surgery has been around for more than 100 years. It is one of the most common surgeries performed in the United States. Over 100,000 are done annually and the majority are on women. In recent years new advancements have been made to speed recovery and success of the operation.
The Lapiplasty system by Treace Medical is at the forefront of bunion repair. This system has taken years to develop and has undergone evolution as it has been utilized. It has now proven to be one of the work horses of bunion surgery. It provides reproducible results and long-term correction. It has an ease of use that makes the surgical procedure faster and improves recovery. This has changed bunion surgery for patients and surgeons. The Lapiplasty system is based on a long-standing surgical technique.
This long-standing technique was first described around the turn of the century by Paul Lapidus. He advocated that the bunion started from the tarsometatarsal joint, and correction needed to occur there. Since his original thought we have only worked to improve and support this theory in the surgical community. It has been shown this is the center of most bunions and the correction is best done here. If you have a bunion the time has never been better to have it fixed.
Lapiplasty is by far the most successful bunion surgery technique I have seen. If you are experiencing bunion pain, I can help call to make an appointment with me at 425-391-8666.
Sincerely,
American College of Foot & Ankle Surgeons


