July 2021
Dr Timothy Young Talks About Tight Calves and Foot Problems
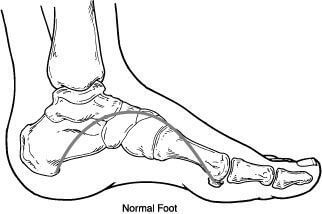
Dr Timothy Young Talks About Tight Calves and Foot Problems
As mentioned, the mechanical load on the foot from the calf and ultimately the Achilles is tremendous. So, with equinus ( a tight calve and or Achilles) there are many problems. Think of a woman who wears high heel shoes every day for many years and over time the calf gets less flexible. Now with that tight calf, her gait has changed. As she walks, with each step going forward that tight calf pulls, and her heel comes off the ground early. Early heel off with gait leads to early transfer of weight and force to the front of the foot. Over time, this extra pressure on the front of the foot can cause problems. This is like the childhood toewalker, but with adult body size and weight.
If you are experiencing any foot or ankle pain, give us a call today at 425-391-8666 or make an appointment online.
Dr Brandon Nelson, A Board Certified Surgeon, Discusses Ankle Surgery
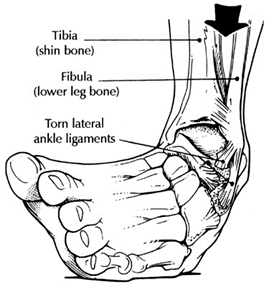
Surgery of the ankle is a fairly common procedure. The majority of ankle surgeries have to do with the outside of the ankle or the lateral ankle complex. The lateral ankle complex is composed of the lateral ankle ligaments and the peroneal tendons. The ligaments on the outside of the ankle are the most important ligaments for stability. These ligaments are often injured with an ankle sprain or ankle fracture. The peroneal tendons work to dynamically stabilize the ankle with activities. These tendons can also be injured with repetitive use or chronic ankle sprains. It is important for anybody that has more than 1 ankle sprain a year to have the structural integrity of their ankle evaluated.
Evaluation of the ankle usually involves and x-ray and a physical examination. In addition, I will often order and MRI to get a better appreciation of the structural components of the ankle. I like an MRI because one can see what the ligaments and tendons look like. This is extremely helpful for evaluation of what needs to be repaired for surgery and what the tissue consistency looks like for the repair.
The surgical procedure itself, or the repair, can be relatively straight forward as in just a ligament stabilization or more complex included bone work. The most common ankle procedure is the lateral ligament reconstruction or the Brostrum procedure. This is a great procedure for anybody with chronic ankle sprains. With this procedure there is a chance you may need the tendons repaired as well.
If you are experiencing frequent ankle sprains or have pain on the outside of the ankle I can help. Make an appointment today and we will get you back on the road to recovery. Give us a call at 425-391-8666.
Bunionettes: The Pinky Toe Bunions
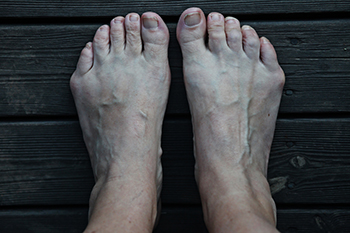 You may have heard of bunions, which sometimes pop up at the base of the big toe joint, but what is a bunionette? Bunionettes, also known as tailor’s bunions, are small, bony bumps that occur at the base of the pinky toe joints. Much like regular bunions, bunionettes can be painful, swollen, and red. Finding comfortable shoes that don’t rub up against the affected area may be difficult. Without treatment, bunionettes usually worsen over time. Fortunately, conservative treatments such as wearing wider shoes, a toe spacer, padding, and activity modifications, are often effective in managing the condition. Surgery to correct a bunionette may be beneficial for a smaller percentage of people. To learn more about bunionettes and what treatment methods are best for you, please consult with a podiatrist.
You may have heard of bunions, which sometimes pop up at the base of the big toe joint, but what is a bunionette? Bunionettes, also known as tailor’s bunions, are small, bony bumps that occur at the base of the pinky toe joints. Much like regular bunions, bunionettes can be painful, swollen, and red. Finding comfortable shoes that don’t rub up against the affected area may be difficult. Without treatment, bunionettes usually worsen over time. Fortunately, conservative treatments such as wearing wider shoes, a toe spacer, padding, and activity modifications, are often effective in managing the condition. Surgery to correct a bunionette may be beneficial for a smaller percentage of people. To learn more about bunionettes and what treatment methods are best for you, please consult with a podiatrist.
If you are suffering from bunions, contact the podiatrists of Issaquah Foot & Ankle Specialists. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
A bunion is formed of swollen tissue or an enlargement of boney growth, usually located at the base joint of the toe that connects to the foot. The swelling occurs due to the bones in the big toe shifting inward, which impacts the other toes of the foot. This causes the area around the base of the big toe to become inflamed and painful.
Why Do Bunions Form?
Genetics – Susceptibility to bunions are often hereditary
Stress on the feet – Poorly fitted and uncomfortable footwear that places stress on feet, such as heels, can worsen existing bunions
How Are Bunions Diagnosed?
Doctors often perform two tests – blood tests and x-rays – when trying to diagnose bunions, especially in the early stages of development. Blood tests help determine if the foot pain is being caused by something else, such as arthritis, while x-rays provide a clear picture of your bone structure to your doctor.
How Are Bunions Treated?
- Refrain from wearing heels or similar shoes that cause discomfort
- Select wider shoes that can provide more comfort and reduce pain
- Anti-inflammatory and pain management drugs
- Orthotics or foot inserts
- Surgery
If you have any questions, please feel free to contact one of our offices located in Issaquah, WA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
What Are Bunions?
Bunions are large bony bumps at the base of the big toe. Medically known as hallux valgus, a bunion is a misalignment of the metatarsophalangeal joint, or big toe joint. The misalignment will generally worsen with time if left untreated.
The exact cause of bunions is unknown, with genetics seen as a potential cause. High heels and poorly-fitted footwear, rheumatoid arthritis, and heredity all seem to be potential factors behind the exacerbation of bunions. Women have been found to be more likely to develop bunions in comparison to men.
Bunions do not always produce symptoms. The best way to tell is if the big toe is pushing up against the next toe and there is a large protrusion at the base of the big toe. You may or may not feel pain. Redness, swelling, and restricted movement of the big toe may be present as well.
Podiatrists use a variety of methods to diagnose bunions. If there are symptoms present, podiatrists will first consider that it is a bunion. If not, a physical examination will be conducted to check function of the big toe. Finally, an X-ray may be taken to view the extent of the bunion and confirm it is a bunion.
Typically, nonsurgical methods are used to treat bunions, unless the bunion has become too misaligned. Orthotics, icing and resting the foot, roomier and better fitted shoes, taping the foot, and pain medication are usually utilized first. If the bunion doesn’t go away or causes extreme pain, surgery may be required. Surgeons will either remove part of the swollen tissue or bone to straighten the toe out.
If you have a bunion, it is recommended to see a podiatrist. The longer it is left untreated, the worse it may get. Podiatrists can properly diagnose and treat a bunion before it gets worse.
Dr. Timothy Young Discusses Stubborn Capsulitis Part 2

Again, I have had this problem before and as mentioned in prior blogs I did many of the appropriate initial treatments listed in my previous blogs. The next step to consider is some of the other alternative treatments. We used to do cortisone injections for this, and we do that very rarely now. There is a non-cortisone anti-inflammatory called Injectable Sterile Traumeel that has much decreased potential risk for damaging the capsule (unlike cortisone). There is also PRP–platelet rich plasma. This can be very effective especially when combined with shockwave treatment. Shockwave treatment can also be done as a stand-alone procedure. The problem with some of these additional treatment options is that they often take several months to really be effective. That's where it's hard to do this but one needs to have patience. Again, that's where cross training can be helpful such as cycling or aqua jogging. For my capsulitis as mentioned, I did the typical initial treatments. I wore special orthotics modified for the capsulitis, I have shoes with a good rocker design, I don't go barefoot at home. I work on stretching my calf and I have a night splint . I stopped running for exercise and only did walking.
Dr Brandon Nelson, A Board Certified Surgeon, Discusses The Best Questions To Ask Your Surgeon Before Having Bunion Surgery
I try to let my patients know that I understand how scary or nervous it can feel to think about surgery. I think as surgeons sometimes we can forget that for us this is routine, however for the patient it can seem overwhelming. Bunion surgery itself is relatively straight forward and can provide great results. I have thought it could be helpful to have a few questions to ask your surgeon.
I think one of the most important questions to ask your surgeon is, “How many bunion surgeries you have done and how often you do them?”. I think most likely you are seeing a Podiatrist and we perform the most bunion surgeries out of any other specialty. I can tell you in residency alone I probably did over 500 and now into private practice for over 10 years I am sure the number is over 1000.
Another important question is, “What are some of the most common complications that occur?”. Every surgery has complications this is part of practicing medicine. The most important aspect of this is how they handle it and how quickly a surgeon responds to these. One of the most common is probably infection and this is rare, the literature state about 3% of all patients will experience this.
Additional question could include, “Why did you select this procedure?” There are numerous different bunion procedures and why we select a particular one is important. This is because they all have different correction abilities and time frames for healing. The majority of bunion procedures can be categorized as head or base procedures. Lastly, “What is my recovery time?”, be specific are you talking about back to exercising or just into a normal shoe.
I hope this was helpful, please feel free to schedule an appointment with me if you would like a consultation of second opinion. Give our office a call at 425-391-8666.
How Can I Prevent Foot Ulcers?
Diabetic foot ulcers (DFUs) are a common complication of diabetes. These foot wounds are difficult to detect in their early stages and heal slowly and poorly, creating a high risk of infection. Fortunately, it is possible to prevent DFUs. The first step in doing so is to protect your feet. Wear comfortable, well-fitting shoes and avoid walking barefoot, even in the home. Small injuries to the foot can go unnoticed and worsen over time due to the lower limb nerve damage and poor circulation that many diabetics face. Protecting your feet helps to avoid those small injuries. Another important step in preventing DFUs is to inspect the feet daily for any abnormalities, such as cuts, scrapes, sores, discoloration, pain, or strange sensations like tingling and numbness. If you notice anything unusual during a daily inspection, contact a podiatrist as soon as possible. A podiatrist can diagnose and treat foot ulcers before they become too severe.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with the podiatrists from Issaquah Foot & Ankle Specialists. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions please contact one of our offices located in Issaquah, WA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Wound Care
Diabetics must be wary of all wounds, regardless of depth or size. Diabetes, a chronic disease in which the body cannot properly use glucose the way it normally would, causes various complications that make wounds difficult to heal. Nerve damage or neuropathy will cause diabetics to have trouble feeling the pain of a blister or cut until the condition has significantly worsened or become infected. A diabetic’s weakened immune system can make even the most minor of wounds easily susceptible to infection. Diabetics are also more prone to developing narrow, clogged arteries, and are therefore more likely to develop wounds.
Wounds should be taken care of immediately after discovery, as even the smallest of wounds can become infected if enough bacteria build up within the wound. To remove dirt, wounds should be first rinsed under running water only. Soap, hydrogen peroxide, or iodine can irritate the injury and should be avoided. To prevent infection, apply antibiotic ointment to the wound and cover it with a bandage. The bandage should be changed daily. The skin around the wound may be cleaned with soap.
To prevent further exacerbation, see a doctor—especially if you have diabetes. Minor skin conditions can become larger problems if not properly inspected. As the wound heals, make sure to avoid applying pressure to the affected area.
Why Live with Pain and Numbness in Your Feet?
Dr. Timothy Young Discusses Stubborn Capsulitis

I have had this condition myself. We are talking about capsulitis of the second metatarsal phalangeal joint (MTP joint) in the ball of the foot, near the base of the second toe. There have been previous blogs about the potential cause of this problem. Treatment has to address the underlying cause and foot structure as much as possible. If the calves are tight, then they have to be stretched and use a night splint or even have a gastroc recession surgery. If there is a bunion and the whole first metatarsal is not bearing is fair share weight then it can cause stress overload to the next in line second metatarsal. Orthotics and foot taping often help this.
Sometimes it's not enough and sometimes especially if there is damage to the capsule such as the plantar plate, we then have to correct the bunion and consider surgery on the second metatarsal. But there are other cases that don't require surgery. It still imperative to do all the other treatments. The correct shoes with a forefoot rocker, sometimes zero drop shoe such as Altra Shoes can also help. Avoiding the activity that seems to aggravate this also can be critical. For example, if you're runner or speed walker, you may have to put that on hold or do cross training until her symptoms have completely resolved. For myself, this seemed to come on after I had resumed running after several months off. I had to make sure my orthotics were still appropriate for this problem. I wore correct shoes. I had to stop running and cross train. I worked on stretching my calf and I have a night splint also.
If you are experiencing foot or ankle pain, give us a call at 425-391-8666 or make an appointment online today.