October 2021
Dr Brandon Nelson, A Board Certified Physician and Surgeon, Discusses Achilles Tendonitis
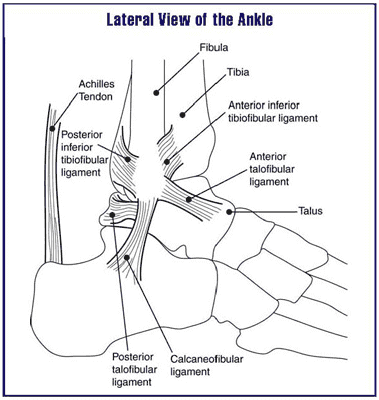
The Achilles tendon is the primary tendon utilized in gait. Meaning that every step, every jump, every run you take you puts mechanical pressure on it. This can result in a lot of wear and tear on this tendon. This can begin to manifest as some pain and even swelling in the Achilles. The irritation usually begins where it attaches to the foot or a few inches above the ankle. Most people that experience Achilles’ tendon pain will be avid exercises. Additionally, it seems to be men rather than woman and between the ages of 40-60.
Evaluating the condition of the tendon before treatment is important. A thorough exam by a physician is essential. There are a lot of factors that play a role in Achilles’ tendonitis and these need to be addressed. These range from foot structure, to training errors to tight muscles. An x-ray or even and MRI may need to be part of the evaluation process. Once the deforming forces and anatomical issues are identified a recovery program can begin.
I encourage anybody with Achilles’ tendon pain to seek help from a physician. This tendon is known to often take months before returning to a normal state. While it is inflamed you run the risk of rupturing the tendon. If the tendon ruptures surgery is required and it can take 6-12 months to completely heal from that scenario.
Give us a call at 425-391-8666 or make an appointment online today.
Dr. Timothy Young, Board Certified Foot Surgeon Talks About How His Capsulitis of the Second Toe Was Treated
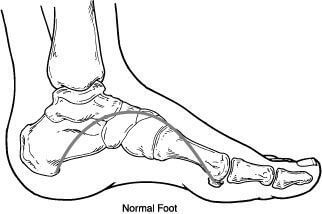
Capsulitis of the second toe and the second MTP joint is one of the more common conditions that we see and treat. Much of this problem is mechanical in nature. Some it has to do with the foot structure itself and it can also be an overuse injury. There is essentially too large a stress load going to this one joint (2nd MTP) disproportionate to the adjacent joints. The traditional treatments that are still critically important include prescription orthotics and good shoes that have forefoot rocker such as a Hoka shoe or Altra shoe. Other treatments include stretching the calf with a night splint and there are other treatments such as taping.
This can be a chronic and frustrating condition to treat. For the most intense problems where there is inflammation of the capsule we often consider adjunctive treatments. One of the simplest treatments that can be done that does not involve an injection is shockwave therapy. The goal of the shockwave therapy is to do intense treatment and the body essentially receives this treatment and believes there has been more trauma. The body reacts by increasing the blood flow to the local tissues including the capsule.
Also some the local healing factors, become more available to this tissue. This is very similar in some ways to other treatments that help the body regenerate. There are other treatments that can be done such as injections. Injections of Supartz which is sympathetic joint lubricant can be very helpful especially if some of the problem is actually intra-articular and not just the capsule but inflammation and pain of the actual joint itself including cartilage pathology and degenerative joint disease. Other injections may include Traumeel which is a non-cortisone based anti-inflammatory. In severe cases the plantar plate can be damaged an MRI may be indicated. These cases often require surgical repair.
Give us a call at 425-391-8666 or make an appointment online today.
How to Care for Diabetic Foot
Millions of people are affected by diabetes each year. Diabetes damages blood vessels in all parts of the body, especially the feet. The legs and feet may develop slow blood flow, which causes neuropathy, or nerve damage. Once a diabetic patient develops neuropathy, it is important that the feet are well taken care of. Otherwise, the lower limbs may have to be amputated. This only happens in drastic cases, but it shows how seriously diabetic foot care should be taken.
It is very important to always wash and dry the feet thoroughly, especially in between the toes, if you’re a diabetic. Secondly, examining your feet and toes for redness or sores must be done, even if you do not feel pain. You may also want to examine your feet from the bottom. Try to avoid wearing colored socks to prevent infections that may occur from the dye. Well-fitting socks are also highly recommended.
A diabetic’s physician should always monitor their blood levels to test how well blood sugars are being maintained. In addition to giving advice about everyday eating habits and foot care, a physician may prescribe medicine to help with the diabetic patient’s neuropathy. It is also advised to see a podiatrist if experiencing any feet conditions. Toenails may also need to be taken care of by a podiatrist. This prevents patients from cutting too deeply around their cuticles, which can lead to infection.
A person can take care of their feet at home by following the instructions of their physician. Using creams on one’s feet is also an effective way to heal dryness. Proceed with caution when using tools to remove calluses, as severe diabetics may not be able to feel pain on their feet. If any complications arise do not hesitate to contact a podiatrist.
On a daily basis, diabetic feet must be checked. If you are ever concerned about something, contact your health care professional. You never want to wait until a wound becomes too severe to treat. If left untreated, gangrene may develop. Gangrene is a serious infection that can lead to sepsis or amputation. It is also important for diabetics to be on the lookout for ulcers. Ulcers are sores that develop from tissue loss on the skin. They can be quite painful and require intensive treatment. Early treatment and everyday inspection are imperative to staying healthy.
The Importance of Foot Care For Diabetics
 Neuropathy, a form of nerve damage, is known for causing a loss of feeling in the feet, and roughly half of all diabetic patients have some type of neuropathy. Because of this lack of feeling, many small problems with the feet may not be noticed and thus lead to the development of serious issues. To help avoid missing the small issues that can occur with the feet, there are some daily things that diabetic patients can do. Daily checks for cuts and wounds, regularly washing the feet, wearing shoes that fit right, and avoiding going barefoot are a few of the things that can be done to help care for the feet once they have lost some feeling. Along with regular checkups, diabetic patients should consult with a podiatrist if they notice a loss of sensation in the feet, a change in shape or color to the feet, or loss of hair on the feet.
Neuropathy, a form of nerve damage, is known for causing a loss of feeling in the feet, and roughly half of all diabetic patients have some type of neuropathy. Because of this lack of feeling, many small problems with the feet may not be noticed and thus lead to the development of serious issues. To help avoid missing the small issues that can occur with the feet, there are some daily things that diabetic patients can do. Daily checks for cuts and wounds, regularly washing the feet, wearing shoes that fit right, and avoiding going barefoot are a few of the things that can be done to help care for the feet once they have lost some feeling. Along with regular checkups, diabetic patients should consult with a podiatrist if they notice a loss of sensation in the feet, a change in shape or color to the feet, or loss of hair on the feet.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact the podiatrists from Issaquah Foot & Ankle Specialists. Our doctors can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
- Routinely inspect your feet for bruises or sores.
- Wear socks that fit your feet comfortably.
- Wear comfortable shoes that provide adequate support.
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions, please feel free to contact one of our offices located in Issaquah, WA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Dr Brandon Nelson, A Board Certified Physician & Surgeon, Discusses When to Get Bunion Surgery
This is probably one of the most common questions I hear when patients come in for a consultation. I think this question is easy to answer, however does have a few details that need to be addressed. I think the most important details are family history, activity level and expectations.
Family history, most bunions have a family history component. There is usually a parent or grandparent that has had a bunion. I think of this as the future of one’s foot structure. Does a relative take off their shoe and all their toes are crossing over? Is there a history of other members having their bunions fixed? These are good questions to answer and can be helpful in deciding to fix your bunion.
Activity level is another important thing to consider. Are you having a hard time exercising due to the pain? Is it getting difficult to fit shoes or boots? I also like patients to think about what your long-term fitness goals are. Will your feet hold up for these? It is vital for our overall health and sense of well being to stay active.
Expectations should be clearly stated and discussed with your surgeon. Do you expect your bunion foot to be exactly like the foot without a bunion? What are your time frames regarding healing? Do you have any up coming obligations like a vacation or wedding? I think taking a critical look at how you hope the surgery goes and how you want to recover can be helpful
These are not inclusive of every detail to help with decision making but are a good place to start. The most important thing is to have your foot evaluated and discuss your goals with your surgeon. If you have a bunion and want to have it evaluated and a detailed plan put in place please give us a call at 425-391-8666 or make an appointment today.
Dr Brandon Nelson, A Board-Certified Surgeon and Physician, Discusses Hammertoes
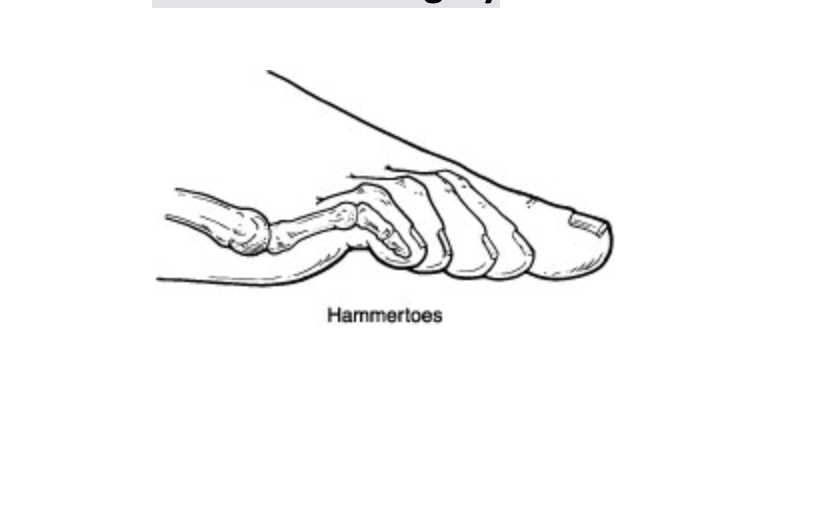
Hammertoes are when your digits on your feet begin to curl. Typically, this is seen with a flat foot or a bunion deformity. However, they can occur in isolation or because of trauma. The deformity itself is usually progressive and can become increasing painful and more severe.
Conservative measures, there are very few available for hammer toes. Some people may find a change in shoe gear can provide some relief. Others will try pads and splints to cushion the toes are create some space. I have never seen these provide long term solutions are change in the hammer toe itself.
Surgical repair continues to be the only long-term solution. Surgery for a hammer toe is relatively straight forward and can provide excellent correction. It is important to consider other underlying factors or pathologies that are contributing to the toes position. I recommend having these addressed at the same time.
If you have some painful digits, we can help.
Give us a call at 425-391-8666 or make an appointment online today today.
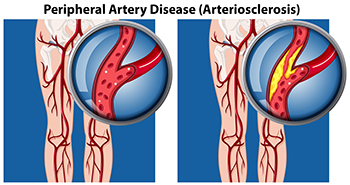
Vascular Testing in Podiatry
In foot care, vascular testing may be required in the diagnosing and treatment of certain podiatric conditions. Vascular testing is particularly relevant for patients with high-risk diabetes, poor circulation, peripheral artery disease (PAD), and chronic venous insufficiency (CVI). Procedures typically involve the examination of blood vessels throughout the body for blockages or buildup.
Vascular testing is very important for the diagnosis of various conditions, including peripheral artery disease and chronic venous insufficiency, as these conditions can greatly affect one’s quality of life and cause pain in the lower limbs. Circulatory problems in the feet and ankles can reflect issues throughout the body, making testing of the blood vessels pertinent.
Testing methods vary between practitioners and can be specific to certain foot and ankle problems. Modern technology has brought about the ability to perform vascular testing using non-invasive methods, such as the cuff-based PADnet testing device. This device records the Ankle-Brachial Index (ABI)/Toe-Brachial Index (TBI) values and Pulse Volume Recording (PVR) waveforms. Contact your podiatrist to determine what vascular testing is available for your needs.
Using Ultrasound to Diagnose Peripheral Artery Disease
Peripheral artery disease (PAD) is a circulatory disease that narrows arteries and restricts blood flow in the extremities. This can cause cramping in the legs when exercising, which usually subsides when you stop. PAD can also cause pain, numbness, swelling, and discoloration in the feet, and can be a prelude to more dangerous complications. One of the tests a podiatrist may use to test the blood flow through arteries and veins is a duplex ultrasound. There are two components to a duplex ultrasound. The first is traditional ultrasound which creates an image by bouncing sound waves off of blood vessels. The second is doppler ultrasound which measures sound waves reflected off of flowing blood to visualize its direction and speed. Duplex ultrasounds are non-invasive. The patient remains still as the podiatrist hovers a wand (transducer) over the area to be tested which sends out sound waves. These sound waves are then reflected back and translated into images. To learn more about PAD and various ways to test for it, please make an appointment with your local podiatrist.
Vascular testing plays an important part in diagnosing disease like peripheral artery disease. If you have symptoms of peripheral artery disease, or diabetes, consult with the podiatrists from Issaquah Foot & Ankle Specialists. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
What Is Vascular Testing?
Vascular testing checks for how well blood circulation is in the veins and arteries. This is most often done to determine and treat a patient for peripheral artery disease (PAD), stroke, and aneurysms. Podiatrists utilize vascular testing when a patient has symptoms of PAD or if they believe they might. If a patient has diabetes, a podiatrist may determine a vascular test to be prudent to check for poor blood circulation.
How Is it Conducted?
Most forms of vascular testing are non-invasive. Podiatrists will first conduct a visual inspection for any wounds, discoloration, and any abnormal signs prior to a vascular test.
The most common tests include:
- Ankle-Brachial Index (ABI) examination
- Doppler examination
- Pedal pulses
These tests are safe, painless, and easy to do. Once finished, the podiatrist can then provide a diagnosis and the best course for treatment.
If you have any questions, please feel free to contact one of our offices located in Issaquah, WA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Dr Brandon Nelson, A Board Certified Surgeon, Discusses the Most Successful Non-Surgical Neuroma Treatment

Neuromas usually present as forefoot pain that is common in woman between the ages of 40-60. Most patients describe a burning or tingling that is worse in shoes. This is most common between the 3rd and 4th toes but can also be present between the 2nd and 3rd. This is primarily do to the anatomical design of the foot and the coming together of nerves in that location.
There are many different treatment options for neuromas and to date one is the most successful. Treatments options can range from toe spacers to injections and physical therapy. The most successful seem to be injection therapies and offloading of the nerve. A well-made prescription orthotic can be extremely helpful for active patients.
Injection therapy is the mainstay of neuroma treatments. Currently the most successful by far is alcohol injections. Alcohol injections work via osmosis by dehydrating the nerve. Our nerves are primarily composed of water and if alcohol is injected adjacent to the nerve over time the nerve will shrink. The nerves that are involved with neuroma formation are sensory nerves. This means these nerves provide pain input and do not contribute to any movement of the toes. The most promising part of alcohol injections is the success rate. The literate states these injections are 89% successful. This is a great option for anybody not wanting surgery.
I have been utilizing alcohol injection therapy for more than 10 years. I can tell you it is highly successful but user dependent. What I mean by that is you need to have a physician that is doing a lot of these to get the best result. I also advise do not have a physician inject without the use of an ultrasound. An ultrasound is key to the successful outcome. Ultrasound helps to identify the nerve and then one can watch the needle placement and the injection will be highly successful. Again I cannot stress that enough, find a physician with an ultrasound so you have the best possible outcome!
Give us a call at 425-391-8666 or make an appointment online today.
Dr Brandon Nelson, A Board Certified Physician and Surgeon, Discusses the Best Long Term Treatment for Plantar Fasciitis
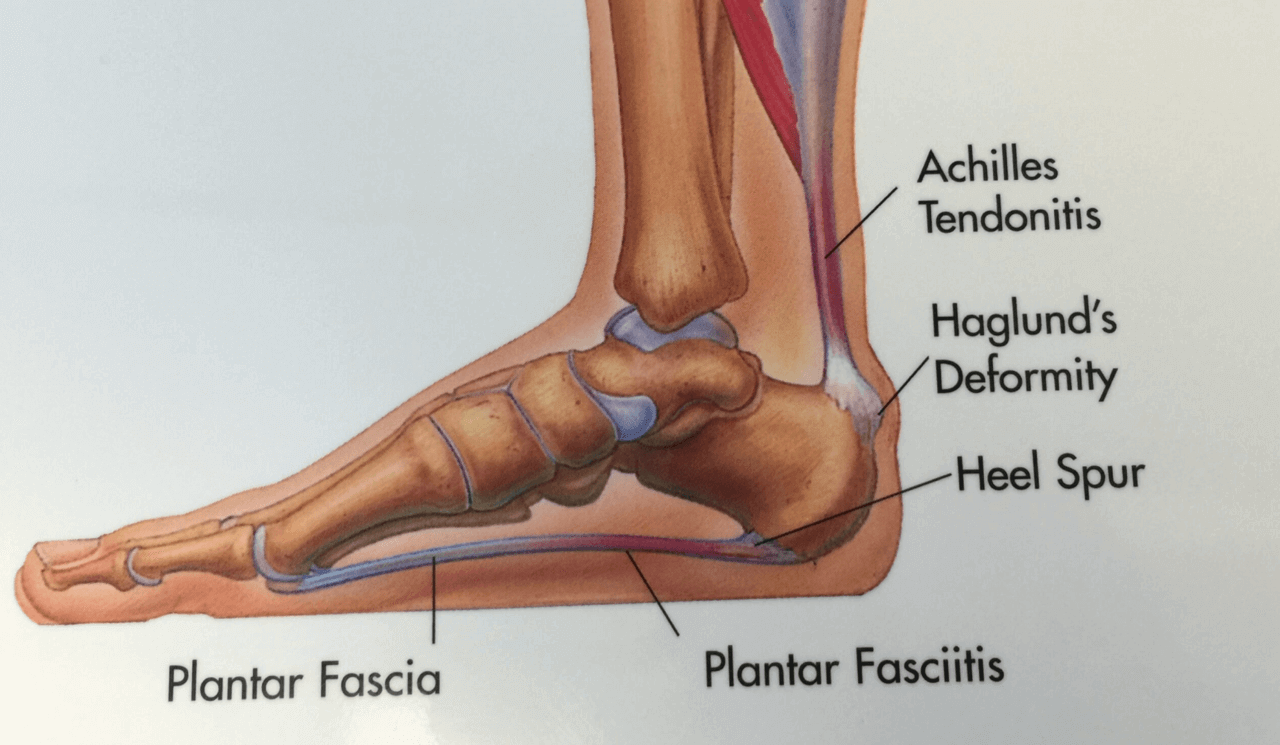
Plantar fasciitis continues to be the most common source of heel pain. The majority of our heel pain patients are still presenting with fasciitis. Patients usually feel pain in the morning or after sitting for a short period of time. The symptoms can range from burning and tingling in the heel to a bruised like sensation when walking. There does not need to be any history of trauma or even an increase in exercise. The major causes continue to be anatomical and foot structure related.
I can tell you I have been treating plantar fasciitis now for almost 15 years. I would say a conservative estimate is probably close to 10,000 patients that I have treated for heel pain. I have learned a lot with this time and quantity. I continue to read and learn and study each patient. This has provided me with a unique perspective. I would say I am probably one of the foremost experts on heel pain.
The best long-term treatment to date that I have discovered is utilizing one’s own biology to heel the plantar fasciitis. This condition is created when the fascia is overworked and needs to be strengthened structurally and functionally. The technique I utilize is unique to my practice and has taken years to perfect. Basically I harness a patient’s natural ability to heal and utilize that to repair the fascia. There is no down time, and the success rate is close to 97%. If you suffer from fasciitis make an appointment today and I will help.
Give us a call at 425-391-8666 or make an appointment online today.