January 2021
Dr. Brandon Nelson Discusses Minimally Invasive Intermetatarsal Nerve Decompression for Morton’s Neuroma
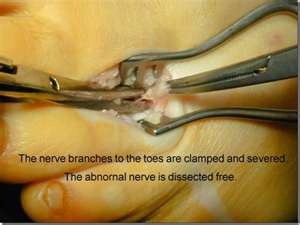
Morton’s neuroma or inner metatarsal neuralgia is a common nerve entrapment of the foot. If left untreated, it can become extremely painful to exercise or wear shoes. There are quite a few nonsurgical approaches to do with the nerve, however not every patient can find relief from these. There are 2 categories of surgical procedures for Morton’s neuroma including decompression and neurectomy. A decompression refers to releasing the structures around the more given more space to decrease inflammation and pain. The neurectomy involves removing portion of the nerve so that the nerve this cannot cause long-term pain. The nerve that is removed is sometimes called is a nerve that provides sensory input, it does not control any motor movement of the toes or foot.
Nerve decompression has been around for quite a long period of time. It is most commonly used for carpal tunnel or tarsal tunnel and has shown good long-term success. This technique was applied to the nerve in the foot and revolves around releasing intermetatarsal ligament to create space for the nerve. The majority of patients to get relief from the nerve decompression have a fairly small neuroma and the long-term data as to whether or not this provides relief has not been ordered.
The traditional surgery or the neurectomy of the Morton’s neuroma involves an incision between the third and fourth metatarsals. Dissection is then carried out in the intermetatarsal ligament is released like with the compression however that a portion of the nerve is removed as well. Long-term success of this procedure has been well established this is considered to be the standard approach for most neuromas.
If you have a Morton’s neuroma and are interested in conservative measures or surgical measures we are here to help. Our on-site surgery center makes it convenient for our patients. Please call us at 425-391-8666 or make an appointment online today.
Dr. Timothy Young, A Board Certified Bunion Surgery Expert Talks About Avoiding Post-op Infections
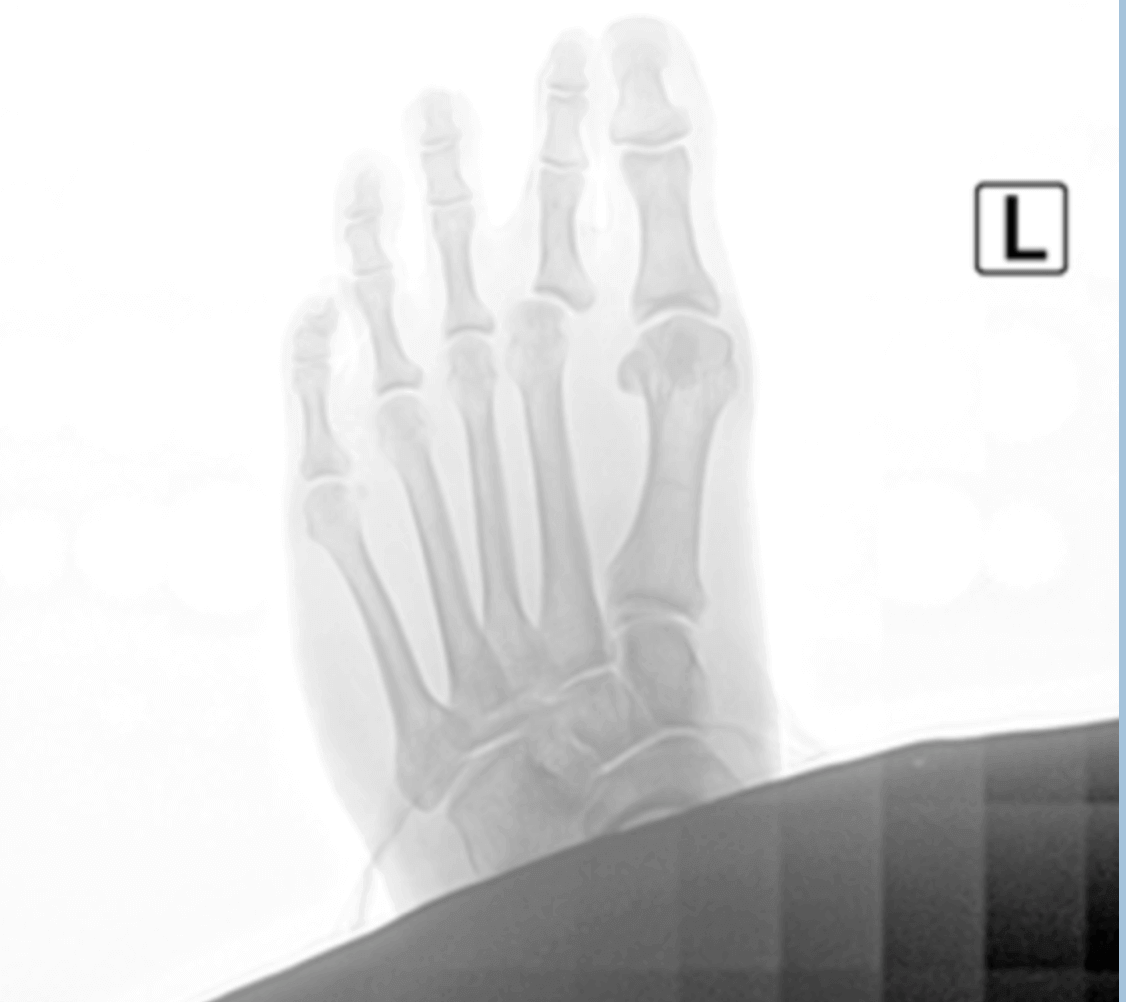
Complications from foot surgery are not common and many of them can be avoided with careful planning and following your doctor’s recommendations. Keeping your foot dry after surgery and until after your sutures are removed is recommended. During the first few days after surgery the incision site will still create a pathway for bacteria to get into the deeper tissue layers.
Sutures also penetrate a deeper layer and if they get wet or are contaminated they could create a direct pathway for bacteria to travel deep and cause an infection. We do not recommend allowing the incision site to get wet with bathing until after sutures are removed. Use a special cast protector for bathing and make sure that it is on correctly. A garbage bag with rubber bands may leak and fill with water-not good! Follow your doctor’s advice on wound care. At our clinic, after surgery we change our patient's dressings at our clinic to make sure it is done using sterile technique, for example a postop infection is certainly going to be more of a risk if you have an open wound or one that still has sutures and you get your foot wet such as bathing.
If you have questions about bunion surgery, and would like a consultation please let us know.
Give us a call today at 425-391-8666 or make an appointment online.
Wound Care
Diabetics must be wary of all wounds, regardless of depth or size. Diabetes, a chronic disease in which the body cannot properly use glucose the way it normally would, causes various complications that make wounds difficult to heal. Nerve damage or neuropathy will cause diabetics to have trouble feeling the pain of a blister or cut until the condition has significantly worsened or become infected. A diabetic’s weakened immune system can make even the most minor of wounds easily susceptible to infection. Diabetics are also more prone to developing narrow, clogged arteries, and are therefore more likely to develop wounds.
Wounds should be taken care of immediately after discovery, as even the smallest of wounds can become infected if enough bacteria build up within the wound. To remove dirt, wounds should be first rinsed under running water only. Soap, hydrogen peroxide, or iodine can irritate the injury and should be avoided. To prevent infection, apply antibiotic ointment to the wound and cover it with a bandage. The bandage should be changed daily. The skin around the wound may be cleaned with soap.
To prevent further exacerbation, see a doctor—especially if you have diabetes. Minor skin conditions can become larger problems if not properly inspected. As the wound heals, make sure to avoid applying pressure to the affected area.
Winter Wound Care Prevention
 Foot wound prevention and care can be slightly more difficult during the cold winter season than during the rest of the year. A common cause of foot wounds in the wintertime is, perhaps ironically, excessive heat. When trying to warm up during the winter, you may not notice excess heat from a hot bath or space heater potentially burning your feet, especially if you have reduced sensation due to conditions like diabetes. Another culprit of foot wounds in the wintertime is dry skin. The cold winter air can make the skin of the feet dry and more likely to crack, thereby increasing the risk of developing foot wounds. It is important to monitor the health of your feet in the winter and all year round, checking regularly for any cuts, scrapes, sores, or other abnormalities. If you notice any changes in your feet, please consult with a podiatrist.
Foot wound prevention and care can be slightly more difficult during the cold winter season than during the rest of the year. A common cause of foot wounds in the wintertime is, perhaps ironically, excessive heat. When trying to warm up during the winter, you may not notice excess heat from a hot bath or space heater potentially burning your feet, especially if you have reduced sensation due to conditions like diabetes. Another culprit of foot wounds in the wintertime is dry skin. The cold winter air can make the skin of the feet dry and more likely to crack, thereby increasing the risk of developing foot wounds. It is important to monitor the health of your feet in the winter and all year round, checking regularly for any cuts, scrapes, sores, or other abnormalities. If you notice any changes in your feet, please consult with a podiatrist.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with the podiatrists from Issaquah Foot & Ankle Specialists. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions please contact one of our offices located in Issaquah, WA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Dr. Brandon Nelson, A Bunion Surgery Expert, Discusses When to Consider Bunion Surgery
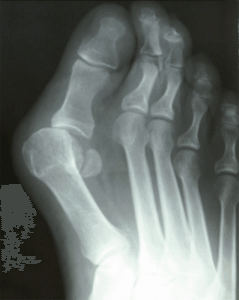
Bunions are painful enlargements around one’s big toe joint. They can be uncomfortable in shoes and with exercise. The majority of pain is usually associated with swelling, throbbing and sometimes redness. Most people with a bunion will have a family history of foot disorders and have a parent with a bunion. Commonly patients will have tried larger shoes or wider shoes and most will continue to have pain despite these measures. I get a lot of questions about the timing of bunion surgery and when to fix the bunion deformity. I will answer some of the most common questions to help others make this decision.
1. When should I have bunion surgery?
The majority of patients I see already have bunion pain and that is why they are in the office. I always have the discussion with patients about whether the bunion is causing pain daily or interfering with the activities they want to enjoy. If these are occurring it is time to fix the bunion. This deformity can make life challenging especially from a physical activity standpoint. If your bunion is preventing you from exercising, it is time to fix it.
2. How long is my recovery?
It depends on the bunion procedure that is utilized. The majority of bunion surgeries patients can begin to walk when they can tolerate it. Surgery will cause some pain and swelling. I like to have my patients aggressively treat the swelling as this will create a quicker return to activities. I also like my patients that are athletic to maintain some sort of activity, like riding a stationary bike. Runners will most likely need about 2-3 months before they can return.
If you are suffering from a bunion and need a consultation to discover what conservative or surgical options are available schedule an appointment online or give us a call at 425-391-8666 today.
Dr. Timothy Young Talks About Using Tylenol After Bunion Surgery or Foot Surgery
Don’t forget that if you take narcotic pain medication, it may have Tylenol in it. Medication such as Percocet and Vicodin may have Tylenol in it and there’s a maximum daily dose of Tylenol, approximately 3000 mg per day. This is why it’s important to keep a log of your medications. If you’re not comfortable with this then make sure to ask your doctor for narcotic pain medication that is a stand-alone item such as pure oxycodone instead of Percocet.
It’s recommended to have a family member help you keep track of these pain medications with a log. Set your clock or phone so that you have a schedule because you want to stay on top of the pain.
If you are experiencing foot or ankle pain, give us a call today at 425-391-8666 or make an appointment online.
Falls Prevention
Elderly Americans are very susceptible to falls as they get older. Everyone experiences decreases in flexibility, balance, strength, and the senses as they age. This correlates to some eye-opening statistics. 1 in 4 Americans aged 65 and older fall each year. An elderly American is being treated for a fall in an emergency room every 11 seconds. In light of these striking statistics, one can see the importance of taking steps to prevent falls.
Finding an exercise program for the elderly is an excellent way to reduce the likelihood of falls. Look for an exercise program that improves strength and balance. Elderly people who live a more sedentary lifestyle, with little physical activity, are at an increased risk of falling. Wearing well-fitted footwear that provides good foot support and cushion will help prevent falls from poorly fitted shoes. Talking to a podiatrist about your susceptibility to falls and about inspecting your prescriptions will help to avoid any medication that could make falls more likely. Due to a decline in the senses among the elderly, having your eyes and hearing checked is recommended.
Around half of all falls occur in the household. Removing tripping hazards in the home and making it more accommodating to older persons can significantly reduce falls. Some notable household changes include increasing lighting around the house, installing grab bars in the shower and bathroom, and making sure the floor is clear of clutter. Other smart options include installing a shower chair, using rubber-bottomed rugs, and placing railings on both sides of stairwells.
Finally, discuss with a doctor and your family about your fear of falling. This will help to increase awareness among the population on the need for fall prevention. A lack of awareness on the matter, and a downplaying of importance are what increase the risks of falling. Following these tips can help to reduce the risk for yourself and your loved ones.
Techniques That May Help to Prevent Falling
 Falling episodes among elderly people is a common occurrence worldwide. Many patients' feet are affected, and may endure a broken foot or sprained ankle as a result of an unexpected fall. Effective prevention techniques can consist of improving lighting in the household and getting regular physical examinations. Maintaining correct medications which may affect your vision can also reduce the risk of falling. Additionally, many patients find it is beneficial to install grab bars in the shower and toilet area, as this provides the necessary stability that can help to prevent falling. If you or a loved one is concerned about how falling can affect the feet, it is suggested that you speak with a podiatrist who can help you with proper prevention techniques.
Falling episodes among elderly people is a common occurrence worldwide. Many patients' feet are affected, and may endure a broken foot or sprained ankle as a result of an unexpected fall. Effective prevention techniques can consist of improving lighting in the household and getting regular physical examinations. Maintaining correct medications which may affect your vision can also reduce the risk of falling. Additionally, many patients find it is beneficial to install grab bars in the shower and toilet area, as this provides the necessary stability that can help to prevent falling. If you or a loved one is concerned about how falling can affect the feet, it is suggested that you speak with a podiatrist who can help you with proper prevention techniques.
Preventing falls among the elderly is very important. If you are older and have fallen or fear that you are prone to falling, consult with the podiatrists from Issaquah Foot & Ankle Specialists. Our doctors will assess your condition and provide you with quality advice and care.
Every 11 seconds, an elderly American is being treated in an emergency room for a fall related injury. Falls are the leading cause of head and hip injuries for those 65 and older. Due to decreases in strength, balance, senses, and lack of awareness, elderly persons are very susceptible to falling. Thankfully, there are a number of things older persons can do to prevent falls.
How to Prevent Falls
Some effective methods that older persons can do to prevent falls include:
- Enrolling in strength and balance exercise program to increase balance and strength
- Periodically having your sight and hearing checked
- Discuss any medications you have with a doctor to see if it increases the risk of falling
- Clearing the house of falling hazards and installing devices like grab bars and railings
- Utilizing a walker or cane
- Wearing shoes that provide good support and cushioning
- Talking to family members about falling and increasing awareness
Falling can be a traumatic and embarrassing experience for elderly persons; this can make them less willing to leave the house, and less willing to talk to someone about their fears of falling. Doing such things, however, will increase the likelihood of tripping or losing one’s balance. Knowing the causes of falling and how to prevent them is the best way to mitigate the risk of serious injury.
If you have any questions, please feel free to contact one of our offices located in Issaquah, WA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Solutions for Cracked Heels
Cracked heels may make you want to think twice about showing off your feet in warmer weather. However, cracked heels may be harmful to more than just the appearance of your feet. If deep fissures and cracks develop in your heels, they may make walking and standing painful for you. Additionally, these openings make way for germs to enter through your skin and cause infection.
There are several different causes of cracked heels. One of the most common reasons for this ailment is dry skin. This problem may make your keeps feel rough tight and itchy. Dry skin may be caused by cold air, extremely hot water, harsh soaps, and aging. Skin disorders such as eczema and psoriasis may eventually lead to dry skin. In some cases, complications may arise from cracked heels. Some of these complications are a loss of feeling in the heel, cellulitis, or a diabetic foot ulcer.
There are ways you can try to prevent getting cracked heels. One of the best ways to do so is to avoid wearing flip flops and sandals because these shoes increase your risk of drying out your feet. You should also avoid wearing shoes with a tall skinny heel, because these shoes cause your heel to expand sideways. At night, you should slather on a thick moisturizing cream on your feet and then cover them in socks to keep your feet moisturized overnight. Drinking water to stay hydrated is also a good way to ensure that your skin doesn’t become dry.
If you suffer from a severe case of cracked feet, you should make an appointment with your podiatrist to see what treatment methods are best for you.
What Can Cause Cracked Heels?
 A foot condition that can cause pain, discomfort, and an unsightly appearance can be described as cracked heels. It can occur as a result of wearing shoes that have an open back, or possibly from specific medical conditions. These can include thyroid disorders, diabetes, or kidney concerns. Additionally, people who are overweight may experience cracked heels from the excess weight and pressure the heels endure. Mild relief may be found when the feet are soaked in warm water, followed by applying a good moisturizer on them. Research has indicated it may help to add a vitamin regime into your daily routine, in addition to drinking plenty of fresh water. If you have cracked heels, it is suggested that you confer with a podiatrist who can offer effective treatment options.
A foot condition that can cause pain, discomfort, and an unsightly appearance can be described as cracked heels. It can occur as a result of wearing shoes that have an open back, or possibly from specific medical conditions. These can include thyroid disorders, diabetes, or kidney concerns. Additionally, people who are overweight may experience cracked heels from the excess weight and pressure the heels endure. Mild relief may be found when the feet are soaked in warm water, followed by applying a good moisturizer on them. Research has indicated it may help to add a vitamin regime into your daily routine, in addition to drinking plenty of fresh water. If you have cracked heels, it is suggested that you confer with a podiatrist who can offer effective treatment options.
If the skin on your feet starts to crack, you may want to see a podiatrist to find treatment. If you have any concerns, contact the podiatrists from Issaquah Foot & Ankle Specialists. Our doctors can provide the care you need to keep you pain-free and on your feet.
Cracked Heels
It is important to moisturize your cracked heels in order to prevent pain, bleeding, and infection. The reason cracked heels form is because the skin on the foot is too dry to support the immense pressure placed on them. When the foot expands, the dry skin on the foot begins to split.
Ways to Help Heal Them
- Invest in a good foot cream
- Try Using Petroleum Jelly
- Ease up on Soaps
- Drink Plenty of Water
Ways to Prevent Cracked Heels
- Moisturize After Showering
- Skip a Shower
- Keep Shower Water Lukewarm
- Don’t Scrub Your Feet
If you are unsure how to proceed in treating cracked heels, seek guidance from a podiatrist. Your doctor will help you with any questions or information you may need.
If you have any questions, please feel free to contact one of our offices located in Issaquah, WA . We offer the newest diagnostic and treatment technologies for all your foot care needs.


