July 2020
Dr. Timothy Young Talks About Shockwave Therapy And How Long It Lasts
Shockwave therapy is one of the newer and most effective treatments for stubborn plantar fasciitis. It is also an excellent treatment for Achilles tendinitis and other tendon and musculoskeletal problems that we see. It is typical for shockwave therapy to be done anywhere from 3-5 treatments usually with 1-2 week intervals. The treatment results in progressive reduction in your symptoms over a period of 3–4 months from the onset of treatment. Once the treatment is complete most patients do not need additional treatment in this regard.
There are a few exceptions where a short mini series of 2 or 3 treatments may be done at 3 or 4 months from the start of treatment for exceptionally stubborn cases. For the majority of our patients that have this treatment they are pain-free and do not have recurrence of the plantar fasciitis symptoms for a period of years. It is important to keep doing proactive "maintenance such as making sure that you wear your orthotics, stretching your calf, and not going barefoot at home. Failure to do some of these treatments could result in recurrence of plantar fasciitis or reinjury.
Can Stretching the Foot Help Plantar Fasciitis Pain?
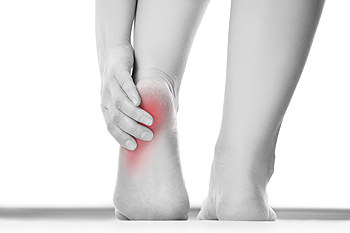 Patients who have the medical condition that is known as plantar fasciitis are often familiar with the severe discomfort this ailment can cause. The pain that is associated with plantar fasciitis is felt in the heel and it can cause difficulty walking. Daily activities may be hard to complete as the day continues, and this can be a result of existing heel pain. This condition can gradually develop from standing for extended periods of time throughout the day, or from wearing shoes that do not fit properly. Moderate relief may be found when the affected foot is stretched. An effective stretch consists of rolling the sole of the foot on a golf ball, and this may help to alleviate a portion of the tension that is commonly associated with this type of foot pain. If you are experiencing any type of heel pain, it is suggested that you consult with a podiatrist as soon as possible who can properly diagnose plantar fasciitis and offer you the correct treatment options.
Patients who have the medical condition that is known as plantar fasciitis are often familiar with the severe discomfort this ailment can cause. The pain that is associated with plantar fasciitis is felt in the heel and it can cause difficulty walking. Daily activities may be hard to complete as the day continues, and this can be a result of existing heel pain. This condition can gradually develop from standing for extended periods of time throughout the day, or from wearing shoes that do not fit properly. Moderate relief may be found when the affected foot is stretched. An effective stretch consists of rolling the sole of the foot on a golf ball, and this may help to alleviate a portion of the tension that is commonly associated with this type of foot pain. If you are experiencing any type of heel pain, it is suggested that you consult with a podiatrist as soon as possible who can properly diagnose plantar fasciitis and offer you the correct treatment options.
Plantar fasciitis can be very painful and inconvenient. If you are experiencing heel pain or symptoms of plantar fasciitis, contact the podiatrists from Issaquah Foot & Ankle Specialists. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is the inflammation of the thick band of tissue that runs along the bottom of your foot, known as the plantar fascia, and causes mild to severe heel pain.
What Causes Plantar Fasciitis?
- Excessive running
- Non-supportive shoes
- Overpronation
- Repeated stretching and tearing of the plantar fascia
How Can It Be Treated?
- Conservative measures – anti-inflammatories, ice packs, stretching exercises, physical therapy, orthotic devices
- Shockwave therapy – sound waves are sent to the affected area to facilitate healing and are usually used for chronic cases of plantar fasciitis
- Surgery – usually only used as a last resort when all else fails. The plantar fascia can be surgically detached from the heel
While very treatable, plantar fasciitis is definitely not something that should be ignored. Especially in severe cases, speaking to your doctor right away is highly recommended to avoid complications and severe heel pain. Your podiatrist can work with you to provide the appropriate treatment options tailored to your condition.
If you have any questions, please feel free to contact one of our offices located in Issaquah, WA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Plantar Fasciitis
The plantar fascia is a connective tissue in the heel that stretches across the bottom length of your foot. Plantar fasciitis occurs when the connective tissue becomes inflamed, causing heel pain and discomfort during physical activity. Although the condition is completely treatable, traditional methods can take up to a year to start becoming effective.
Plantar fasciitis is caused by a number of everyday activities, so understanding the condition is important for managing and treating it. One of the most common causes of plantar fasciitis is excessive running, especially with improper fitting or non-supportive shoes. Too much exercise can lead to the plantar fascia being overworked and overstretched, which can cause tears in the tissue. Along with improper fitting shoes, pronation, the rolling of the feet inward, is a common cause of plantar fasciitis. If not treated properly, the plantar fascia becomes overstretched and starts to tear, causing inflammation.
Despite the common causes of plantar fasciitis, there are many different treatment options. For less severe cases, conservative home remedies include taking anti-inflammatory drugs to alleviate pain, applying ice packs to the bottom of your foot and heel, slowly stretching and exercising your feet to re-strengthen the tissue, and using orthotic devices are all ways to help manage your plantar fasciitis.
For more severe cases, shockwave therapy has become a common solution for plantar fasciitis. Shockwave therapy can effectively break up the tissue on the bottom of your foot which facilitates healing and regeneration. This fights the chronic pain caused by plantar fasciitis. Even if this doesn’t work, surgery is always a final option. Surgery on the tissue itself can be done to permanently correct the issue and stop the inflammation and pain in your heels.
No matter what the case may be, consulting your podiatrist is the first and best step to recovery. Even the slightest amount of heel pain could be the first stage of plantar fasciitis. Untreated symptoms can lead to the tearing and overstretching of tissue. Because the tearing of tissue can be compounded if it remains ignored, it can evolve into a severe case. The solution is early detection and early treatment. Talk to your podiatrist about the possibilities of plantar fasciitis if you’re experiencing heel pain.
Dr. Brandon Nelson Discusses The Best Treatment Option For Neuromas
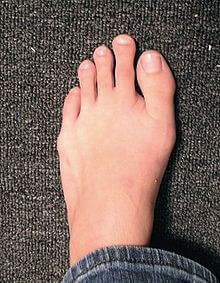
Neuromas often cause a considerable amount of pain for patients. Typically a neuroma will cause a burning pain between the 3rd and 4th digit. Patients often experience increased pain with wearing shoes and walking. A common phrase we hear is a patient will feel like their sock is balled up in their shoe. Neuromas typically progress and become increasingly painful. I find it to be important to treat them early, this seems to help my patients to get back to normal activities as soon as possible.
I find alcohol injection therapy to be the most effective tool in getting rid of neuromas. I see patients that have had multiple cortisone injections and physical therapy all to no avail. The sclerosing injection therapy works extremely well for patients. The literature success rate is reported to be almost 90%. I find it to be helpful even for patients that are contemplating surgical removal of the neuroma. If you have burning or tingling in your toes or have been diagnosed with a neuroma we can help.
Give us a call at 425-391-8666 or make an appointment online.
Bunion Information Center
What is a Bunion?
A bunion is often described as a bump on the side of the big toe. However, a bunion is more than that. The visible bump actually reflects changes in the bony framework of the front part of the foot. The big toe leans toward the second toe, rather than pointing straightahead. This throws the bones out of alignment – producing the bunion’s “bump.”
Causes
Bunions are a progressive disorder. They begin with a leaning of the big toe, gradually changing the angle of the bones over the years and slowly producing the characteristic bump, which becomes increasingly prominent. Symptoms usually appear at later stages, although some people may never have symptoms. Bunions are a common foot deformity that can be inherited or occur as a result of repeated stress to the joint. It is not the bunion itself that is inherited, but certain foot types that make a person prone to developing a bunion. Not wearing proper sized footwear that crowd one’s toes will not cause bunions, however it can contribute to the progression of the deformity. As a result, symptoms may appear sooner with improper footwear.
Symptoms
Symptoms, which occur at the site of the bunion, may include:
• Pain or soreness
• Inflammation and redness
• A burning sensation
• Possible numbness
Symptoms occur most often when wearing shoes that crowd the toes, such as shoes with a tight toe box or high heels. This may explain why women are more likely to have symptoms than men. In addition, spending long periods of time on your feet can aggravate the symptoms of bunions.
Diagnosis
Bunions are readily apparent – the prominence is visible at the base of the big toe or side of the foot. However, to fully evaluate the condition, the foot and ankle surgeon may take x-rays to determine the degree of the deformity and assess the changes that have occurred. Because bunions are progressive, they don’t go away, and will usually get worse over time. But not all cases are alike – some bunions progress more rapidly than others. Once your surgeon has evaluated your bunion, a treatment plan can be developed that is suited to your needs.
Non-Surgical Treatment
Most people however, find relief from wearing soft, pliable shoes, and arch supports, and from applying ice to the sore toe joint Sometimes observation of the bunion is all that’s needed. To reduce the chance of damage to the joint, periodic evaluation and x-rays by your surgeon are advised.
When Should I See A Doctor For My Toe Injury?
 Some foot injuries can be serious and may require a visit to the doctor, for example a broken toe. If you have injured your toe and have experienced swelling that has not decreased within five days, noticed a change in the color of your toe, or continued to feel pain days after the initial injury, it may be time to seek professional care. Other worrisome symptoms of a more severe toe injury can include numbness, tingling, or a burning sensation, which could indicate nerve damage, deformation of the toe, or pain so severe that you are unable to walk normally. If you find yourself experiencing any of these symptoms, seek help from a podiatrist, who specializes in foot care and will assess and treat your injury.
Some foot injuries can be serious and may require a visit to the doctor, for example a broken toe. If you have injured your toe and have experienced swelling that has not decreased within five days, noticed a change in the color of your toe, or continued to feel pain days after the initial injury, it may be time to seek professional care. Other worrisome symptoms of a more severe toe injury can include numbness, tingling, or a burning sensation, which could indicate nerve damage, deformation of the toe, or pain so severe that you are unable to walk normally. If you find yourself experiencing any of these symptoms, seek help from a podiatrist, who specializes in foot care and will assess and treat your injury.
A broken toe can be very painful and lead to complications if not properly fixed. If you have any concerns about your feet, contact the podiatrists from Issaquah Foot & Ankle Specialists. Our doctors will treat your foot and ankle needs.
What to Know About a Broken Toe
Although most people try to avoid foot trauma such as banging, stubbing, or dropping heavy objects on their feet, the unfortunate fact is that it is a common occurrence. Given the fact that toes are positioned in front of the feet, they typically sustain the brunt of such trauma. When trauma occurs to a toe, the result can be a painful break (fracture).
Symptoms of a Broken Toe
- Throbbing pain
- Swelling
- Bruising on the skin and toenail
- The inability to move the toe
- Toe appears crooked or disfigured
- Tingling or numbness in the toe
Generally, it is best to stay off of the injured toe with the affected foot elevated.
Severe toe fractures may be treated with a splint, cast, and in some cases, minor surgery. Due to its position and the pressure it endures with daily activity, future complications can occur if the big toe is not properly treated.
If you have any questions please feel free to contact one of our offices located in Issaquah, WA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
What to Know About a Broken Toe
Trauma to the foot, especially the toes, can occur in many ways. Banging them, stubbing them, or dropping something on them are a few different ways this trauma can occur. Given the fact that toes are positioned in front of the feet, they typically sustain the brunt of such trauma. When trauma occurs to a toe, the result can be a painful break or fracture. Another type of trauma that can break a toe is repeated activity that places stress on the toe for prolonged periods of time.
Broken toes can be categorized as either minor or severe fractures. Symptoms of minor toe fractures include throbbing pain, swelling, bruising on the skin and toenail, and the inability to move the toe with ease. Severe toe fractures require medical attention and are indicated when the broken toe appears crooked or disfigured, when there is tingling or numbness in the toe, or when there is an open, bleeding wound present on the toe.
Generally, a minor toe break will heal without long-term complications. However, it is important to discontinue activities that put pressure on the toe. It is best to stay off of the injured toe and immediately get a splint or cast to prevent any more additional movement of the toe bones. You can also immobilize your toe by placing a small cotton ball between the injured toe and the toe beside it. Then, tape the two toes together with medical tape. Swelling can be alleviated by placing an ice pack on the broken toe directly as well as elevating your feet above your head.
Severe toe fractures may be treated with a splint, cast, and in some cases, minor surgery, especially when the big toe has been broken. Due to its position and the pressure the big toe endures with daily activity, future complications can occur if it is not properly treated. Pain associated with minor toe fractures can be managed with over-the-counter pain medications. Prescription pain killers may be necessary for severe toe fractures.
The healing time for a broken toe is approximately four to six weeks. In severe cases where the toe becomes infected or requires surgery, healing time can take up to eight weeks or more. While complications associated with a broken toe are immediately apparent, it is important to note that there are rare cases when additional complications, such as osteoarthritis, can develop over time. You should immediately speak with your podiatrist if you think you have broken your toe due to trauma. They will be able to diagnose the injury and recommend the appropriate treatment options.
Dr. Young Talks About Lateral Column Pain and Lateral Overload

Dr. Young Talks About Lateral Column Pain and Lateral Overload
This is a subject that I have talked about previously. I wanted to revisit this and summarize this problem and condition. The lateral column of the foot encompasses the fourth and fifth metatarsals. This is the outside of the foot that includes the fifth toe and the fifth metatarsal phalangeal joint. It also includes the fifth metatarsal base which is the insertion point for the peroneal brevis tendon. Finally it also includes the cuboid bone and some patients with this may be diagnosed with "cuboid syndrome".
This is a common condition that I see in our clinic. It is frustrating for our patients because often this is not something that comes with a real nice clear diagnosis like let's say a bunion. But what happens is the patient will present to our clinic and say that they have pain on the outside of their foot (lateral column). Often times the patient will have a high arch foot or they will have compensated for another problem such that the weight is shifted to the outside of the foot. The lateral column is not designed for significant weightbearing. This is primarily the function and job for the great toe joint and the medial column. Therefore all it takes is a small change in weightbearing or the pattern of gait and the extra load going through the outside of the foot causes pain and symptoms. It is very rare to have a stress fracture in this location but that can happen. What can happen as there is just fatigue and pain on the lateral column and the stress load is such that it is short of that needed to cause a stress fracture. So stress fracture rarely occurs in this location. It is possible to develop pain at the insertion of the peroneal tendon of the fifth metatarsal base. It's also possible to have a tailor's bunion and have that pain flareup.
Our patients will have an x-ray to make certain there is no other pathology in this location. This condition responds very well to prescription orthotics tuned to shift the pressure off the lateral column of the foot, especially if it is a chronic condition. Some athletic shoes are better than others for this also. If there is a component of peroneal tendon symptoms, and there is a special ankle brace that may be helpful also.
These are some the conditions that may be associated with lateral column pain:
-Tailor's bunion or pain affecting the fifth MTP joint
-Stress fracture of the fourth or fifth metatarsal (rare)
-Stress reaction of bone of the fourth and fifth metatarsal (rare)
-Nonspecific Bone "fatigue and pain" of the fourth and fifth metatarsal (common)
-Insertional peroneal brevis tendinitis
-Cuboid area pain "cuboid syndrome"
If you have foot pain and need evaluation, please see myself Dr. Timothy Young, or my partner Dr. Brendon Nelson. Give us a call at 425-391-866 or make an appointment online.
Dr. Brandon Nelson Discusses Plantar Fasciitis, Arch Pain and Heel Pain Essential Considerations for Treatment
Most foot and ankle physicians, podiatrist and sports medicine doctors like me will see a considerable amount of heel pain and heel spurs during their career. The majority of this heel pain will be caused by plantar fasciitis and present with multiple symptoms including burning, stabbing and throbbing of the heel. However, it is important to rule out other causes of heel pain including nerve entrapments, stress fractures and bursitis. It is essential to see a physician to get the correct diagnosis before implementing treatment plans.
Often times patients spend a considerable amount of time on the Internet to implement treatment in this can be detrimental to their long-term well-being in healing of the pathology. I recommend seeing your foot and ankle physician, podiatrist in order to get a correct diagnosis. The patient workup often includes physical examination and x-rays and a detailed history. Patients with complicated heel pain may benefit from more advanced studies like an MRI or EMGs NCV’s. If you’re suffering from heel pain, heel spurs or plantar fasciitis we would like to help you be pain free.
Give us a call at 425-391-8666 or make an appointment online today.
The Importance of Practicing Foot Care for Diabetic Patients
 Patients who are diabetic may be fearful of losing a toe or foot due to their condition. Foot complications can occur as a result of elevated blood sugar levels and can cause the feet to feel numb or minimal sensation. This may lead to the inability to feel existing cuts or bruises on the feet, and diabetic ulcers may develop. It is beneficial to implement a daily foot care routine. This can consist of washing the feet every day, properly trimming the toenails, and maintaining steady blood circulation. It is helpful to smooth corns and calluses by utilizing a pumice stone, and this can aid in preventing foot infections from developing. If you have diabetes, it is strongly suggested that you are under the care of a podiatrist who can guide you toward proper management techniques.
Patients who are diabetic may be fearful of losing a toe or foot due to their condition. Foot complications can occur as a result of elevated blood sugar levels and can cause the feet to feel numb or minimal sensation. This may lead to the inability to feel existing cuts or bruises on the feet, and diabetic ulcers may develop. It is beneficial to implement a daily foot care routine. This can consist of washing the feet every day, properly trimming the toenails, and maintaining steady blood circulation. It is helpful to smooth corns and calluses by utilizing a pumice stone, and this can aid in preventing foot infections from developing. If you have diabetes, it is strongly suggested that you are under the care of a podiatrist who can guide you toward proper management techniques.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact the podiatrists from Issaquah Foot & Ankle Specialists. Our doctors can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
- Routinely inspect your feet for bruises or sores.
- Wear socks that fit your feet comfortably.
- Wear comfortable shoes that provide adequate support.
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions, please feel free to contact one of our offices located in Issaquah, WA . We offer the newest diagnostic and treatment technologies for all your foot care needs.


