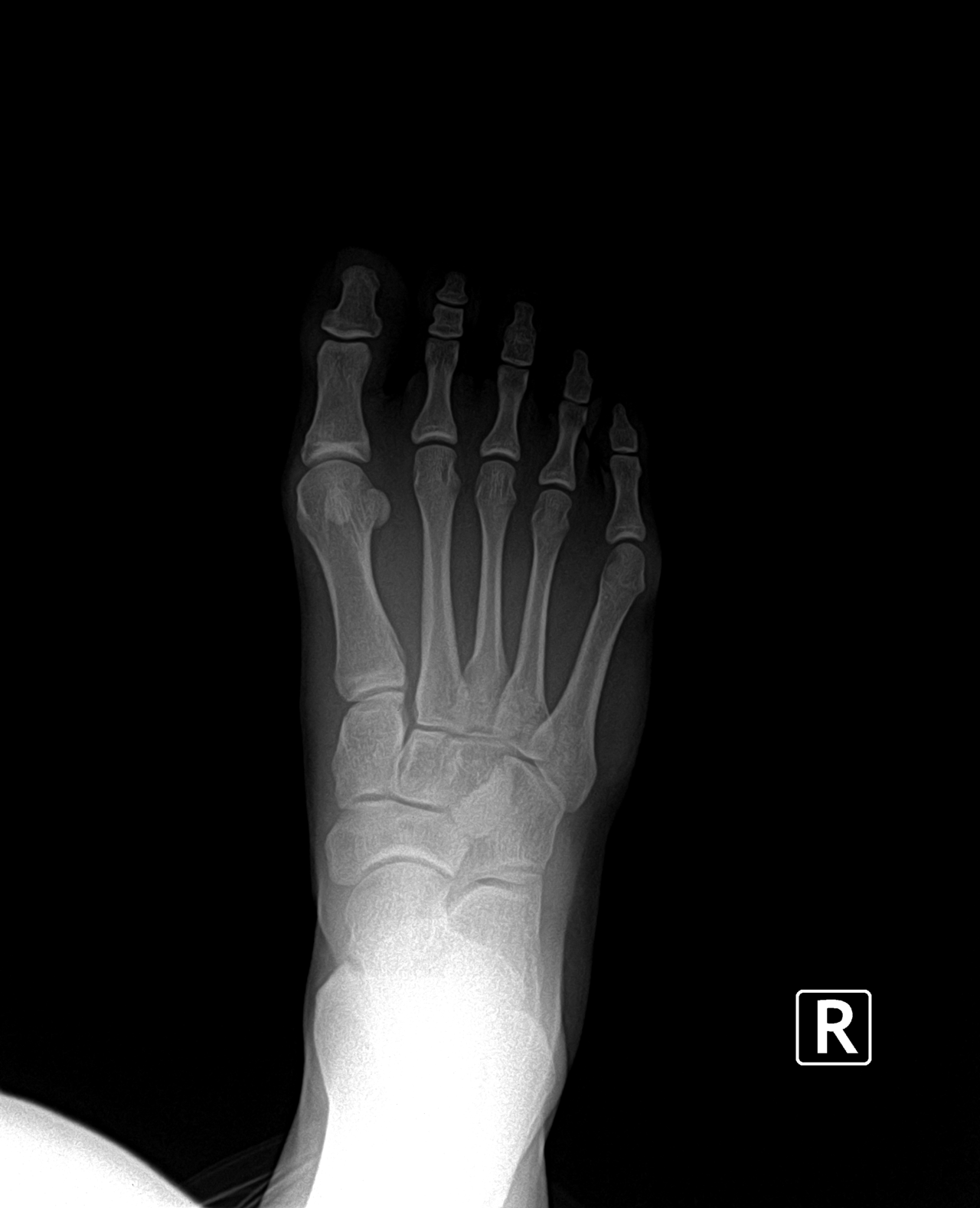
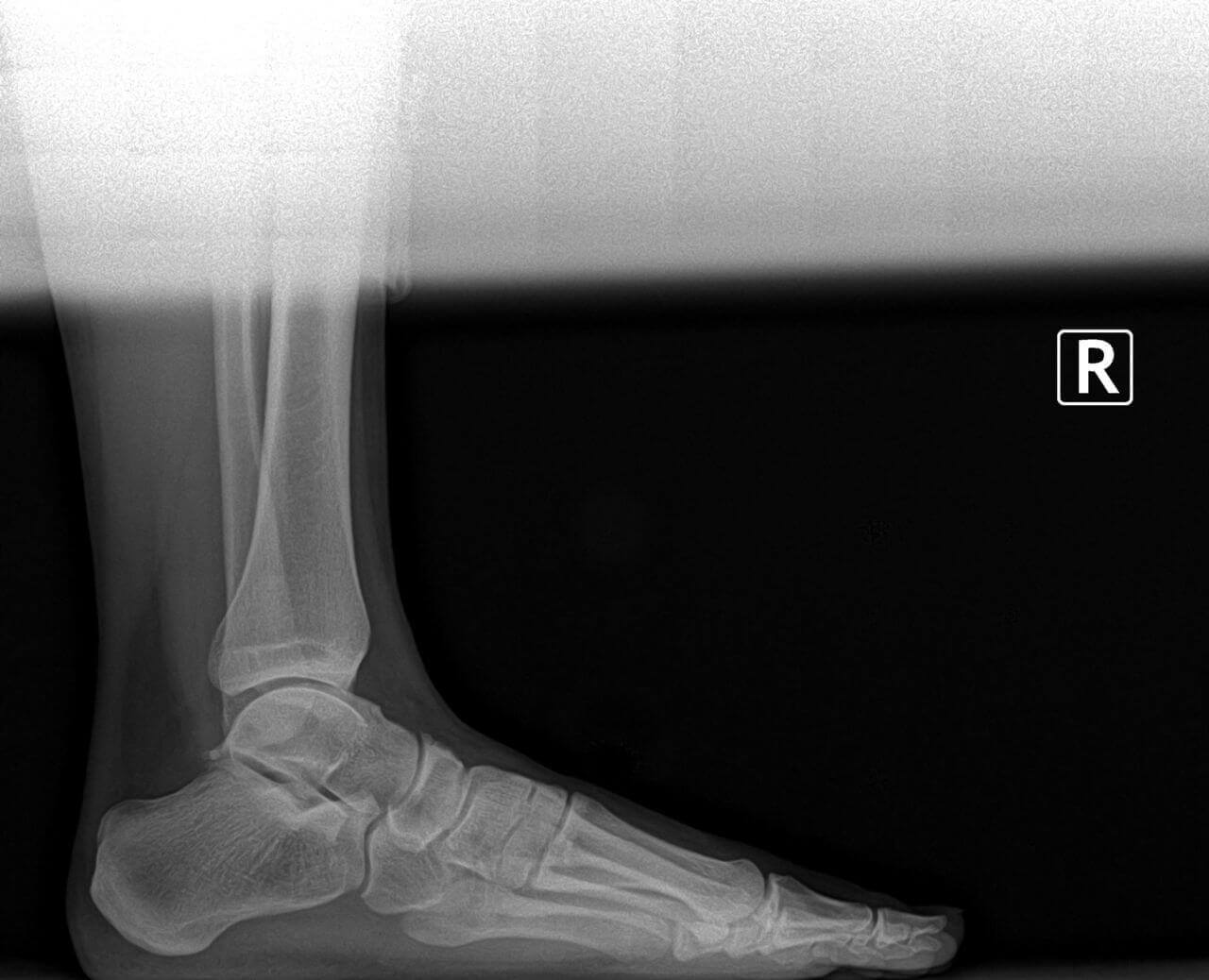
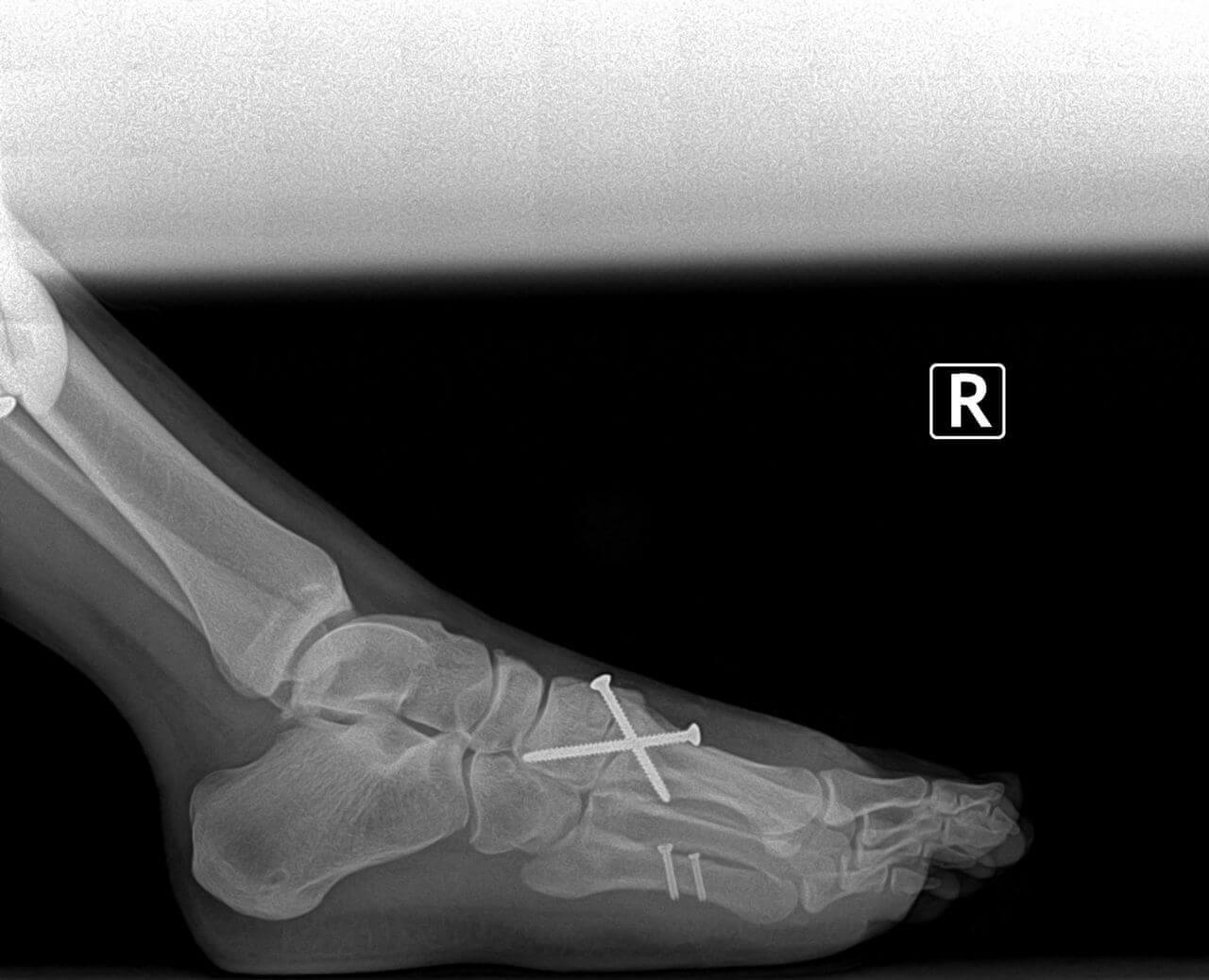
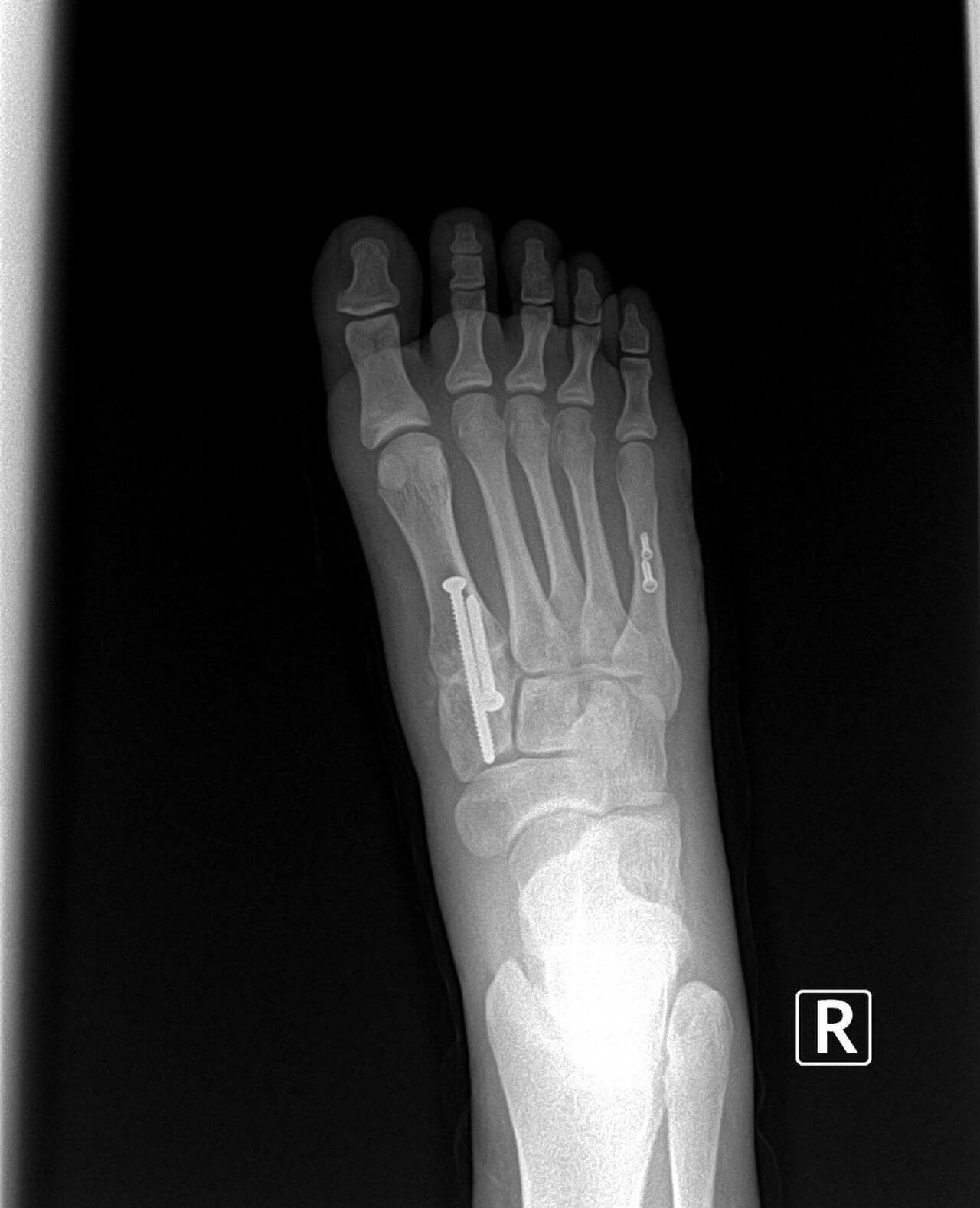
The soft corn is caused by a section of bone in the fifth toe pressing against the bone in the base of the fourth toe. When this occurs, the skin between the toes is pinched excessively and becomes damaged. Because of moisture between the toes, the "corn" is soft. The skin is often white in appearance. On occasion, a small ulceration can form and the area can become infected. Surgical treatment for this condition is similar to the surgical correction for hammertoes.
Description of the Surgery
An incision is placed on the top of the fifth toe. The ligaments about the joint in the toe are released to allow exposure of the head of the bone called the proximal phalanx. It is this section of the fifth toe bone that is pressing on the base of the fourth toe. The head of the proximal phalanx in the fifth toe is then cut and removed. If the toe is contracted or curled, then the tendon in the bottom of the fifth toe is released. On occasion, the surgeon will also make a small incision at the base of the fourth toe and smooth the bone in this area. In rare instances, the skin between the fourth and fifth toes may be so badly damaged that correcting the bone problem alone will not cure the soft corn. In this instance, the damaged skin between the toes must be removed. This procedure called a syndactylism necessitates removing the damaged skin between the toes and sewing the fourth and fifth toes together. This may sound like a drastic procedure, but it produces no loss of foot function. The procedure can be performed to leave a good cosmetic result. Surgery to correct soft corns can be performed in the doctor's office or in an outpatient surgery center. A local anesthetic is adequate for this surgery in most cases. Recovery from this procedure is much the same as for the correction of hammertoes. At the conclusion of surgery, a gauze dressing is applied.
What to Expect Following the Surgery
The patient should stay off their foot, keeping it elevated above their heart for a minimum of three days. Limited activity is recommended for two to three weeks. The stitches are removed in ten to fourteen days. During this period of time, the foot should be kept dry to reduce the risk of infection. A postoperative shoe is used to accommodate the bandage, and should be worn whenever the patient walks on their foot. Neglecting to wear the shoe while walking will cause the bandage to come loose, resulting in excessive movement at the surgical site, which will cause swelling, delays in healing, and possible infection. Once the stitches are removed, bathing the foot is permitted. Barefoot walking is discouraged for three weeks from the time of surgery. The patient should wear the postoperative shoe until they are able to wear normal shoes comfortably. This may take three to four weeks from the time of surgery. Some patients are able to return to normal shoes as early as two weeks.
Possible Complications
There are relatively few complications associated with this surgery. Excessive swelling which delays the healing process is the most common problem associated with the surgery. Postoperative infection rates are low but the risk increases if the surgical site is not kept dry. A reoccurrence of the condition is possible if enough bone is not removed or if the patient returns to wearing shoes that are too tight. If too much bone is removed then the toe may be floppy. It is normal for the toe to feel floppy for a few weeks following the surgery. The toe generally stiffens over time.


 Unfortunately, a small percentage of people that develop
Unfortunately, a small percentage of people that develop