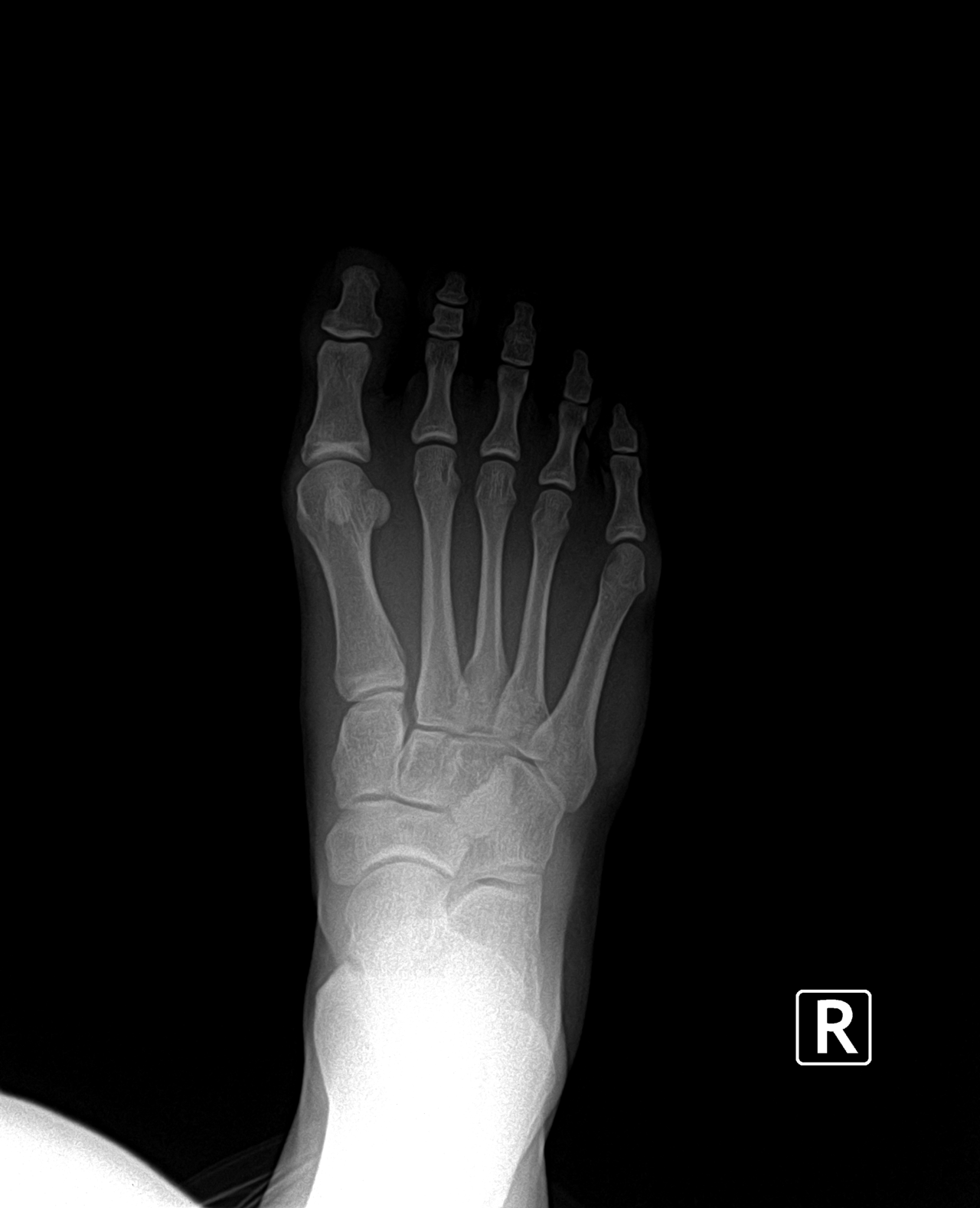
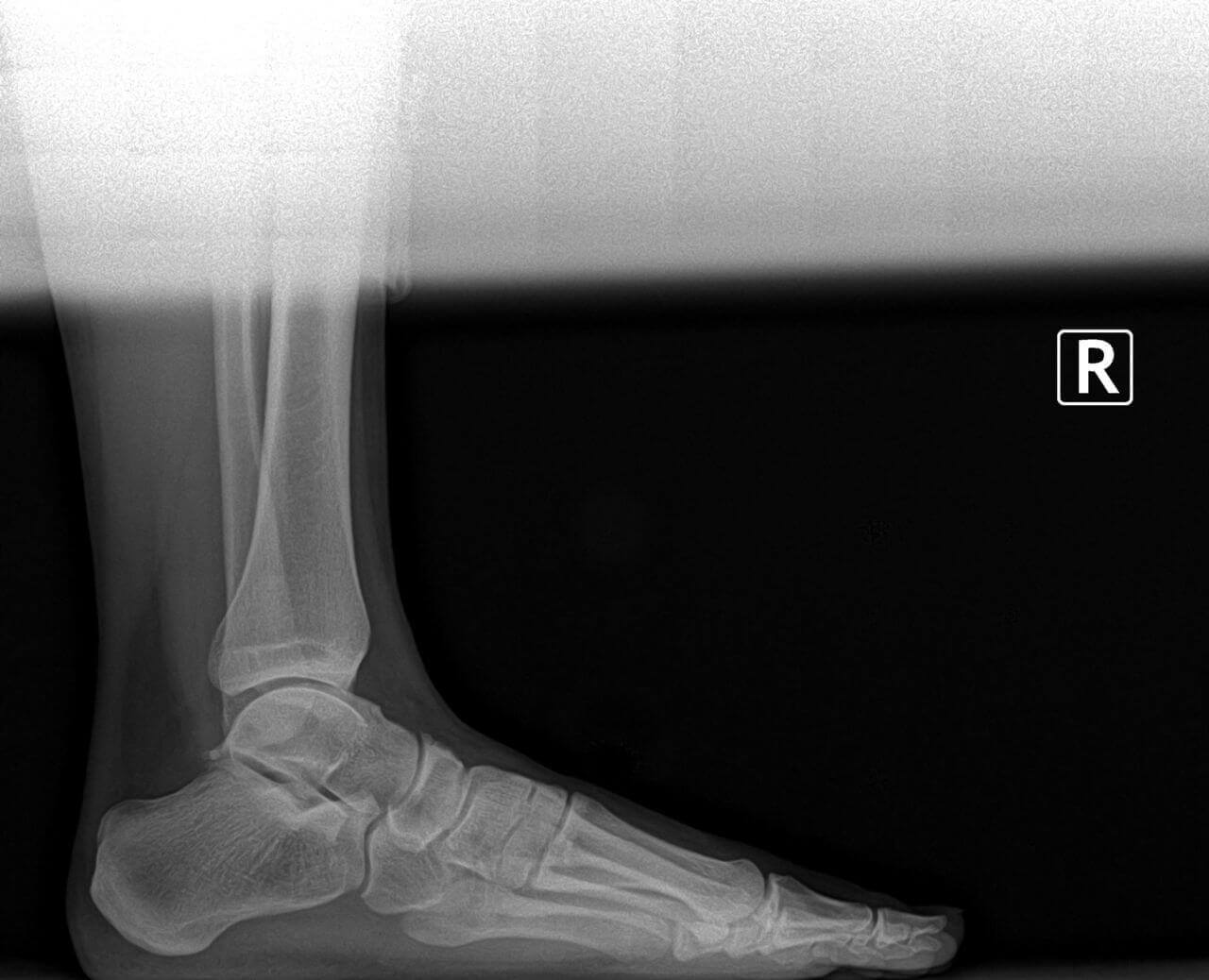
There are five metatarsal bones in each foot. These bones are the long bones behind each toe. The metatarsal bone behind the big toe is called the first metatarsal. The metatarsal bone behind the little toe is called the fifth metatarsal. The most common metatarsal surgery is preformed on the first metatarsal for the correction of bunion deformity. The second most common metatarsal surgery is on the fifth metatarsal for the correction of tailor's bunion deformity. This article will address metatarsal surgery of the other metatarsals.
Surgery on the remaining metatarsal bones is performed infrequently. When surgery is performed on the second, third, or fourth metatarsal bones, it is generally for the treatment of painful callouses on the bottom of the foot or for the treatment of non-healing ulcerations on the ball of the foot. Patients with rheumatoid arthritis may require surgery of the metatarsals, which is discussed in another section. Also surgery of the metatarsals may be necessary in instances of trauma of the foot where the metatarsal bones may have been fractured. This article will discuss elective metatarsal surgery.
Painful callouses on the ball of the foot are due to an abnormal alignment of the metatarsal bones. If a metatarsal bone is lower than the others, excessive weight is placed on this area of the foot, and a painful callous may form. In people with diabetes, these areas of excessive pressure may break down and form open sores or ulcerations. Initial treatment generally consist of using a functional or accommodative orthotic to reduce the pressure to these areas. If this is not successful, metatarsal surgery may be considered.
The Surgery
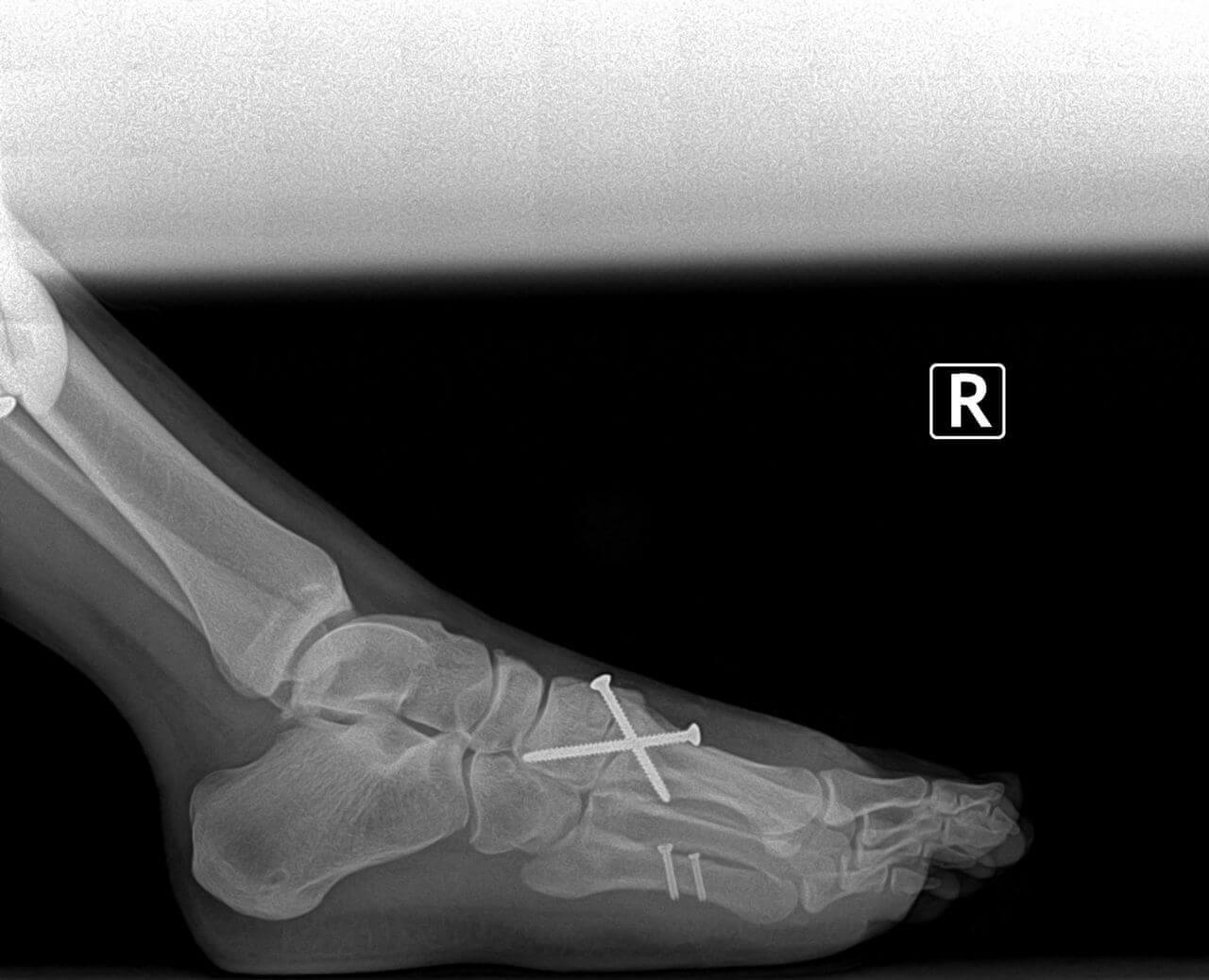
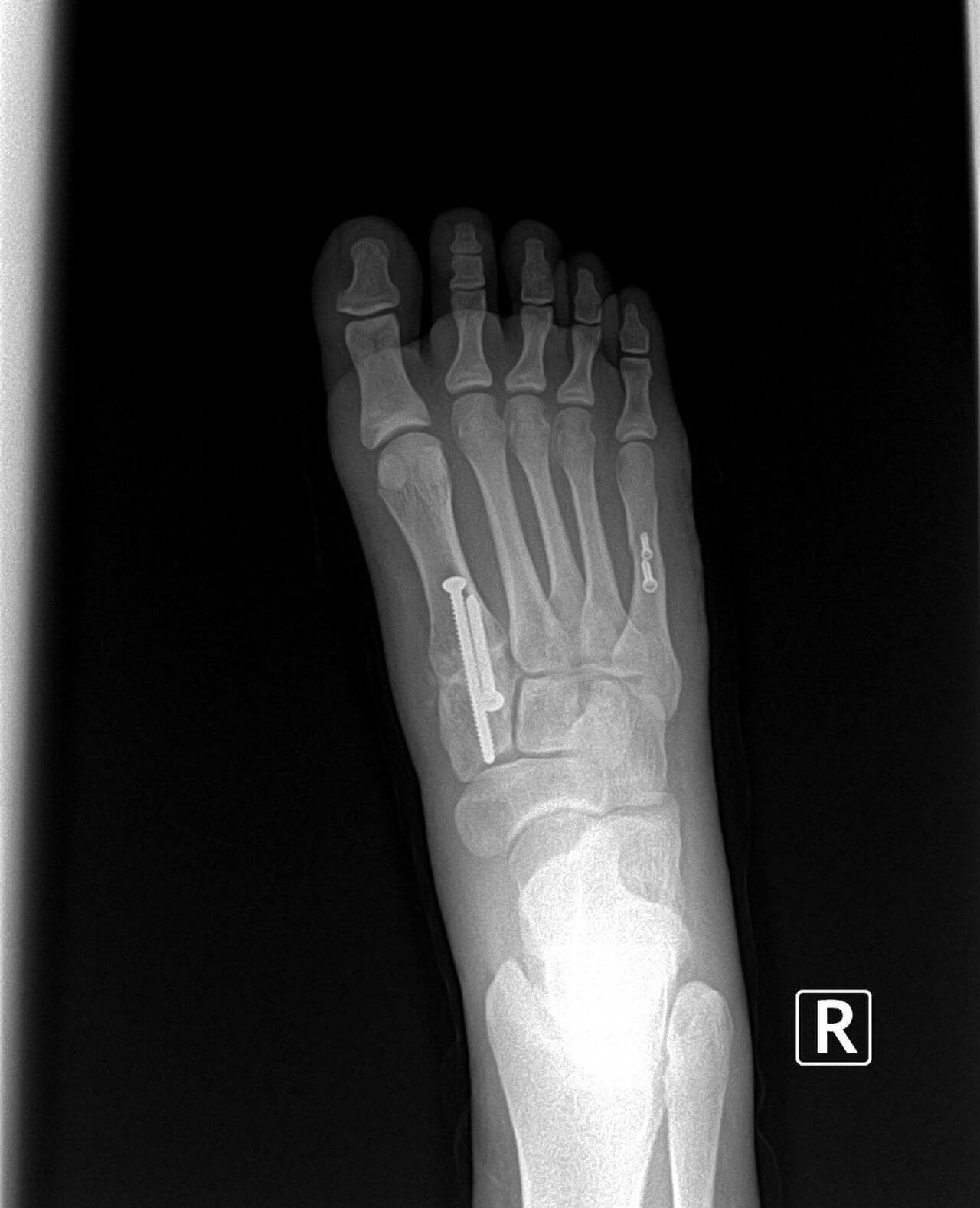
The surgery consists of cutting the metatarsal bone just behind the toe. Generally, the bone is cut all the way through, and then manually elevated and held in its corrected position with a metal pin or screw. Following the surgery, the patient may be placed in a cast, or may be required to use crutches for several weeks. If a pin is used to hold the bone in place, it is generally removed in three to four weeks. Removal of the pin can be done in the doctor's office without the need for anesthesia. While the pin is in place, the patient should keep the foot dry to prevent infection. Generally it takes a total of six to eight weeks, or longer, for the bone to heal. During this healing period, the foot should be protected from excessive weight bearing. Walking prematurely on the foot can cause the bone to shift and heal in an incorrect position. This is the most common cause of failure with this surgery. Some studies indicate a failure rate as great as 60%. If the bone shifts downward, or is not elevated enough at the time of surgery, the painful callous may return. If the bone is elevated too much, a painful callous may form under the metatarsal next to the one which was operated on.
Some surgeons will also cut out the painful callous on the bottom of the foot when they perform the metatarsal surgery. Rarely will a foot surgeon remove the painful callous without also performing the metatarsal surgery. Without correcting the metatarsal alignment, the painful callous is almost certain to return.
Most surgeons prefer to do the surgery in an outpatient surgery center or hospital. In this setting, intra-venous sedation or general anesthesia can be used for the patient’s comfort.
At the conclusion of the surgery, the surgeon places a gauze bandage on the foot. Generally, the bandage stays in place until the patient’s first follow up visit with the doctor. The skin stitches are removed in ten to fourteen days. If there are stitches in the bottom of the foot, they may remain in place for three weeks. The foot should be kept dry while the stitches and/or pin are in place to help prevent infection. May surgeons will have the patients wear a below the knee cast and/or use crutches for six to eight weeks. Other surgeons will allow the patient to wear a stiff-sole post-operative shoe, and allow limited walking on the foot.
Recovery Time
The time required to be off work will vary with the demands of the person’s job. A minimum of one week off work would be advisable with the patient staying at home with the foot elevated above the heart.
Possible Complications
Complications associated with this surgery are: infection, failure of the bone to heal in its correct position resulting in the return of the painful callous or transfer of the callous to a new location, delays or failure of bone healing, stress fractures of adjacent metatarsals, or excessive swelling. A common occurrence following the surgery is elevation of the toe associated with the elevated metatarsal bone that was operated on.
Metatarsal Surgery to Treat Diabetic Ulcerations
Diabetic patients with non-healing ulcerations on the ball of the foot may undergo a different type of metatarsal surgery. In this instance, the section of the metatarsal bone associated with the excessive pressure, called the metatarsal head, may be removed entirely. This is a relatively common and successful surgery that aids in the healing of the ulceration on the bottom of the foot. Possible complications with this surgery include infection, failure of the procedure to heal the ulceration, or the development of new ulcerations in adjacent areas on the ball of the foot. If the patient has poor circulation, further complications may be failure of the surgical sight to heal, or gangrene with partial loss of the foot or leg.
In most instances of metatarsal surgery, the patient should use an orthoticin their shoe after the surgery has healed. This is especially important for the diabetic patient. The orthotic will reduce the risk of reoccurrence or the development of new areas of callous formation or tissue break down.
 Unfortunately, a small percentage of people that develop plantar fasciitis will not have success with conservative therapies. We have an established treatment protocol for heel pain, making us a premier location for the treatment of plantar fasciitis. The standard of care is six months to a year of conservative therapy before surgical intervention should be considered. We have multiple surgical modalities available for patients with recalcitrant plantar fasciitis. These surgical procedures can be performed with mild sedation in our outpatient surgery center that can save you both time and money by not having to go to the hospital or ambulatory surgery centers. The procedures include:
Unfortunately, a small percentage of people that develop plantar fasciitis will not have success with conservative therapies. We have an established treatment protocol for heel pain, making us a premier location for the treatment of plantar fasciitis. The standard of care is six months to a year of conservative therapy before surgical intervention should be considered. We have multiple surgical modalities available for patients with recalcitrant plantar fasciitis. These surgical procedures can be performed with mild sedation in our outpatient surgery center that can save you both time and money by not having to go to the hospital or ambulatory surgery centers. The procedures include: