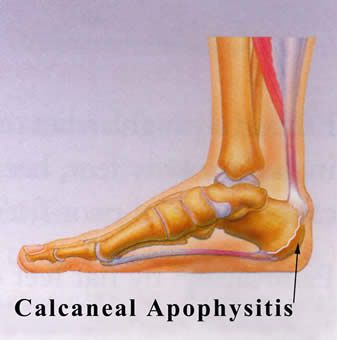
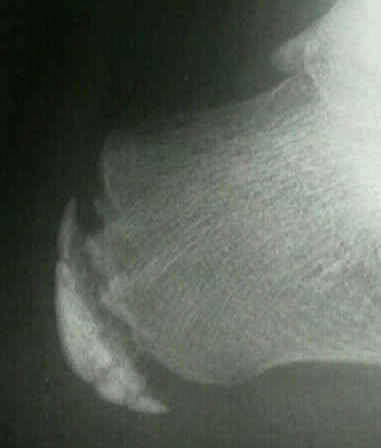
Deformities of the toes are common in the pediatric population. Generally they are congenital in nature with both or one of the parents having the same or similar condition. Many of these deformities are present at birth and can become worse with time. Rarely do children outgrow these deformities although rare instances of spontaneous resolution of some deformities have been reported.
Malformation of the toes in infancy and early childhood are rarely symptomatic. The complaints of parents are more cosmetic in nature. However, as the child matures these deformities progress from a flexible deformity to a rigid deformity and become progressively symptomatic. Many of these deformities are unresponsive to conservative treatment. Common digital deformities are underlapping toes, overlapping toes, flexed or contracted toes and mallet toes. Quite often a prolonged course of digital splitting and exercises may be recommended but generally with minimal gain. As the deformity becomes more rigid surgery will most likely be required if correction of the deformity is the goal.
Underlapping Toes
Description
Underlapping toes are commonly seen in the adult and pediatric population. The toes most often involved are the fourth and fifth toes. A special form of underlaping toes is calledclinodactyly or congenital curly toes. Clinodactyly is fairly common and follows a familial pattern. One or more toes may be involved with toes three, four, and five of both feet being most commonly affected.
The exact cause of the deformity is unclear. A possible etiology is an imbalance in muscle strength of the small muscles of the foot. This is aggravated by a subtle abnormality in the orientation on the joints in the foot just below the ankle joint called the subtalar joint. This results in an abnormal pull of the ligaments in the toes causing them to curl. With weight bearing the deformity is increased and a folding or curling of the toes results in the formation of callus on the outside margin of the end of the toe. Tight fitting shoes can aggravate the condition.
Treatment
The age of the patient, degree of the deformity and symptoms determine treatment. If symptoms are minimal, a wait and see approach is often the best bet. When treatment is indicated the degree of deformity determines the level of correction. When the deformity is flexible in nature a simple release of the tendon in the bottom of the toe will allow for straightening of the toe. If the deformity is rigid in nature then removal of a small portion of the bone in the toe may be necessary. Both of these procedures are common in the adult patient for the correction of hammertoe deformity. If skin contracture is present a derotational skin plasy may be required.
Overlapping Toes - Overlapping Fifth Toe
Description
This deformity is characterized by one toe lying on top of an adjacent toe. The most common toe involved is the fifth toe. When one of the central toes is involved the second toe is most commonly affected. The etiology of the condition is not well understood. It is though that it may be caused by the position of the fetus in the womb during development. The condition my run in families so there may be a hereditary component to the deformity.
Treatment
Effective conservative treatment depends upon how early the diagnosis is made. In infancy, passive stretching and adhesive tapping is most commonly used. This may require 6 to 12 weeks to accomplish and reoccurrence is not uncommon. Rarely will the deformity correct itself. As the individual matures the deformity becomes fixed. When surgical correction is warranted a skin plasty is required to release the contracture of the skin associated with the deformity. Additionally a tendon release and a release of the soft tissues about the joint at the base of the fifth toe may be required. In severe cases the toe may require the placement of a pin to hold the toe in a straightened position. The pin, which exits the tip of the toe, may be left in place for up to three weeks. During this period of time the patient must curtail their activities significantly and wear either a post-operative type shoe or a removable cast. Excessive movement at the surgical site can result in a less than desirable result. The pin can be easily removed in the doctor's office with minimal discomfort. Following removal of the pin splinting of the toe may be required for an additional two to three weeks.
Hammertoes and Mallet Toes
Description
Another common digital deformity is contracture of the toes in the formation of hammertoes and mallet toes. Hammertoes are described in depth in another article. Mallet toes are a result of contracture of the last joint in the toe. In the pediatric population it is often flexible and not painful. Over time the deformity becomes rigid and a callus may form on the skin overlying the joint at the end of the toe. Additionally the toenail may become thickened and deformed form the repetitive jamming of the toe while walking. The deformity usually involves one or two toes, with the second toe most commonly affected. Mallet toes have several etiologies. Longer toes that are forced against a short toe box in the shoe will, over time, develop a contracture of the last joint in the toe causing a mallet toe.
Treatment
Conservative treatment consists of padding and strapping the toes into a corrected position. This treatment may alleviate the symptoms but will not correct the deformity. Diabetic patients often develop ulcerations on the ends of their toes secondary to mallet toe deformity and the pressure that results from the toe jamming into the shoe. When standing, the toe will demonstrate a contracture, with the tip of the toe facing downward into the floor. If the deformity is flexible a simple release of the tendon in the bottom of the toe will allow straightening of the toe. Following the procedure the patient must avoid shoes that cause jamming of the toe or the deformity can reoccur. When the deformity is rigid surgical correction requires the removal of a small section of bone in the last joint of the toe. On occasion fusion of the last two bones in the toe may be necessary. This requires removing the cartilage from the last joint in the toe and pinning the bones together. When the bone heals it forms a single bone and the toe remains in a straightened position. Healing time is dependent upon the procedure selected. If a tendon release is performed the patient my return to a roomy shoe within a week. If the toe is straightened by removing a section of the bone in the toe it make ten days to three weeks for a patient to return to normal shoes. If a fusion is performed to straighten the toe, the patient may not return to normal shoes for 6 to 8 weeks. Time off from work will depend upon the type of shoe gear that must be worn and the level of activity necessary to perform the job. A minimum of three to four days off from work is generally recommended and longer if the job responsibilities can not be modified to accommodate the normal healing time for the surgery.






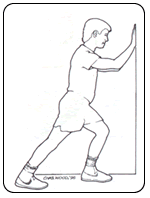 Calf muscle stretching is very useful in the treatment of many foot disorders and for the prevention of foot problems. The typical runners stretch, by leaning into a wall, is helpful. An alternative method of stretching is to stand approximately two feet from a wall. Facing the wall, turn your feet inward so you are pigeon toed. Lean forward into the wall keeping your heels on the floor and the knees extended. Also keep your back straight and do not bend at the hips. Hold the stretch for 10 seconds and do the stretch ten times in a row. Do the stretching three times each day. Always stretch the calf muscles following any form of exercise. If the stretching causes pain it should not be performed. The stretch should be felt in the body of the muscle not in the Achilles tendon or the back of the knee. If you are unable to perform the stretch properly consult with a doctor or physical trainer.
Calf muscle stretching is very useful in the treatment of many foot disorders and for the prevention of foot problems. The typical runners stretch, by leaning into a wall, is helpful. An alternative method of stretching is to stand approximately two feet from a wall. Facing the wall, turn your feet inward so you are pigeon toed. Lean forward into the wall keeping your heels on the floor and the knees extended. Also keep your back straight and do not bend at the hips. Hold the stretch for 10 seconds and do the stretch ten times in a row. Do the stretching three times each day. Always stretch the calf muscles following any form of exercise. If the stretching causes pain it should not be performed. The stretch should be felt in the body of the muscle not in the Achilles tendon or the back of the knee. If you are unable to perform the stretch properly consult with a doctor or physical trainer.