What is Capsulitis of the Second Toe?
Ligaments surrounding the joint at the base of the second toe form a “capsule,” which helps the joint to function properly. Capsulitis is a condition in which these ligaments have become inflamed.
Although capsulitis can also occur in the joints of the third or fourth toes, it most commonly affects the second toe. This inflammation causes considerable discomfort and, if left untreated, can eventually lead to a weakening of surrounding ligaments that can cause dislocation of the toe. Capsulitis—also referred to as predislocation syndrome—is a common condition that can occur at any age.
Causes
It is generally believed that capsulitis of the second toe is a result of abnormal foot mechanics, where the ball of the foot beneath the toe joint takes an excessive amount of weight-bearing pressure.
Certain conditions or characteristics can make a person prone to experiencing excessive pressure on the ball of the foot. These most commonly include a severe bunion deformity, a second toe longer than the big toe, an arch that is structurally unstable, and a tight calf muscle.
Symptoms
Because capsulitis of the second toe is a progressive disorder and usually worsens if left untreated, early recognition and treatment are important. In the earlier stages—the best time to seek treatment—the symptoms may include:
- Pain, particularly on the ball of the foot. It can feel like there’s a marble in the shoe or a sock is bunched up
- Swelling in the area of pain, including the base of the toe
- Difficulty wearing shoes
- Pain when walking barefoot
In more advanced stages, the supportive ligaments weaken leading to failure of the joint to stabilize the toe. The unstable toe drifts toward the big toe and eventually crosses over and lies on top of the big toe—resulting in “crossover toe,” the end stage of capsulitis. The symptoms of crossover toe are the same as those experienced during the earlier stages. Although the crossing over of the toe usually occurs over a period of time, it can appear more quickly if caused by injury or overuse.
Diagnosis
An accurate diagnosis is essential because the symptoms of capsulitis can be similar to those of a condition called Morton’s neuroma, which is treated differently from capsulitis.
In arriving at a diagnosis, the foot and ankle surgeon will examine the foot, press on it, and maneuver it to reproduce the symptoms. The surgeon will also look for potential causes and test the stability of the joint. X-rays are usually ordered, and other imaging studies are sometimes needed.
Non-surgical Treatment
The best time to treat capsulitis of the second toe is during the early stages, before the toe starts to drift toward the big toe. At that time, non-surgical approaches can be used to stabilize the joint, reduce the symptoms, and address the underlying cause of the condition.
The foot and ankle surgeon may select one or more of the following options for early treatment of capsulitis:
- Rest and ice. Staying off the foot and applying ice packs help reduce the swelling and pain. Apply an ice pack, placing a thin towel between the ice and the skin. Use ice for 20 minutes and then wait at least 40 minutes before icing again.
- Oral medications. Nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen, may help relieve the pain and inflammation.
- Taping/splinting. It may be necessary to tape the toe so that it will stay in the correct position. This helps relieve the pain and prevent further drifting of the toe. The Dr may provide you with a temporary splint.
- Stretching. Stretching exercises may be prescribed for patients who have tight calf muscles. A night splint can be employed as well.
- Shoe modifications. Supportive shoes with stiff soles are recommended because they control the motion and lessen the amount of pressure on the ball of the foot
- Prescription Orthotic devices. Custom orthotic devices that fit into the shoe provide support for the arch, and may play a role in preventing future symptoms. These are not over the counter inserts these are prescription medical devices made by a physician.
- No barefeet. We highly recommend not going barefoot around the house, Vionic slippers or flip-flops work extremely well.
- Cortisone Injections. These are often very useful in alleviating symptoms
- Immobilization. In some severe cases of pediatric heel pain, a cast may be used to promote healing while keeping the foot and ankle totally immobile.
When is Surgery Needed?
Once the second toe starts moving toward the big toe, it will never go back to its normal position unless surgery is performed. The foot and ankle surgeon will select the procedure or combination of procedures best suited to the individual patient.
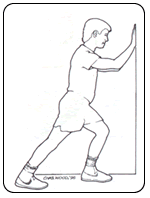 Calf muscle stretching is very useful in the treatment of many foot disorders and for the prevention of foot problems. The typical runners stretch, by leaning into a wall, is helpful. An alternative method of stretching is to stand approximately two feet from a wall. Facing the wall, turn your feet inward so you are pigeon toed. Lean forward into the wall keeping your heels on the floor and the knees extended. Also keep your back straight and do not bend at the hips. Hold the stretch for 10 seconds and do the stretch ten times in a row. Do the stretching three times each day. Always stretch the calf muscles following any form of exercise. If the stretching causes pain it should not be performed. The stretch should be felt in the body of the muscle not in the Achilles tendon or the back of the knee. If you are unable to perform the stretch properly consult with a doctor or physical trainer.
Calf muscle stretching is very useful in the treatment of many foot disorders and for the prevention of foot problems. The typical runners stretch, by leaning into a wall, is helpful. An alternative method of stretching is to stand approximately two feet from a wall. Facing the wall, turn your feet inward so you are pigeon toed. Lean forward into the wall keeping your heels on the floor and the knees extended. Also keep your back straight and do not bend at the hips. Hold the stretch for 10 seconds and do the stretch ten times in a row. Do the stretching three times each day. Always stretch the calf muscles following any form of exercise. If the stretching causes pain it should not be performed. The stretch should be felt in the body of the muscle not in the Achilles tendon or the back of the knee. If you are unable to perform the stretch properly consult with a doctor or physical trainer.

 New treatment for plantar fasciitis: Dry needling combined with a cortisone injection, guided ultrasound imaging-the alternative to plantar fasciitis surgery. Researchers state that this approach has a 95% success rate. They also state that the ultrasound guidance makes the procedure very safe. They recommend the procedure combined with orthotic treatment and advised that 42/44 of their study patients were cured of their symptoms within 2-3 weeks of treatment. The dry needling technique allows for increased blood flow to the symptomatic plantar fascia region. This helps it heal faster. Traditionally structures like the plantar fascia, tendons and ligaments do not have a lot of blood flow, so they tend to heal slowly. The premise behind this is quite similar to the APC percutaneous growth factor procedure that we also utilize. One difference is that this new procedure is much less costly and can be done right in our exam rooms with local anesthetic.
New treatment for plantar fasciitis: Dry needling combined with a cortisone injection, guided ultrasound imaging-the alternative to plantar fasciitis surgery. Researchers state that this approach has a 95% success rate. They also state that the ultrasound guidance makes the procedure very safe. They recommend the procedure combined with orthotic treatment and advised that 42/44 of their study patients were cured of their symptoms within 2-3 weeks of treatment. The dry needling technique allows for increased blood flow to the symptomatic plantar fascia region. This helps it heal faster. Traditionally structures like the plantar fascia, tendons and ligaments do not have a lot of blood flow, so they tend to heal slowly. The premise behind this is quite similar to the APC percutaneous growth factor procedure that we also utilize. One difference is that this new procedure is much less costly and can be done right in our exam rooms with local anesthetic.